Introduction
Psoriasis is a common chronic cutaneous disease
involving an abnormal inflammatory response characterised by an
increase in proinflammatory cytokines consequential to the
hyperproliferation of keratinocytes. Both environmental and genetic
factors interfere in the pathogenesis of psoriasis. The course of
the disease usually involves a long period of cutaneous lesions
which can result in psychological implications and severe impact on
the quality of life.
The treatment based on the radiations of the UVB
spectrum implies apoptosis of T lymphocytes and immunosuppressive
effects resulting in clinical improvement of immune skin diseases.
The 308 nm laser excimer represents a viable treatment option of
inflammatory skin diseases such as vitiligo, atopic dermatitis,
alopecia areata and psoriasis. It has been used in patients with
psoriatic lesions that affect <10% of the body area,
recalcitrant plaques, or difficult to treat areas. Patients
diagnosed with psoriasis may achieve clearance using the excimer
laser technology more rapidly than using narrow-band UVB. Reduced
number of sessions are necessary for treatment which signifies a
lower cumulative dose than that in the UVB narrow band therapy.
Known as lepra graecorum in the ancient
times, it was well described as a clinical condition in 1808 by the
British physician Robert Willan. At present, due to many
improvements in the research fields, the pathogenesis, genetical
implications and risk factors are mainly known. Nearly 125 million
people are suffering from psoriasis, currently, as shown by the
International Federation of Psoriasis Associations (1). The data determined from the USA and
European countries, suggest a prevalence estimated between 0.91 and
8.5% (2). Being a common disease, it
is a subject of great interest in many fields of human
research.
Early onset of psoriasis is associated with the
expression of HLA-Cw6 (3-7),
classified as type I psoriasis and is frequently seen in
individuals younger than 40 years of age with positive family
history of this disease. Type II psoriasis is associated with later
onset, usually after the age of 40(7).
The clinical appearance is divided into the
following: the most common form is plaques psoriasis, which affects
the majority of patients; another clinical presentation is guttate
psoriasis which is associated with acute onset and is often
detected in children after a streptococcal episode. The pustular
form is characterised by amicrobial pustules and can affect
different percentages of the body (localised or generalised). The
life-threatening form of psoriasis is the erythrodermic form which
consists of generalized erythema and suggests a low treatment
compliance. The use of UVB therapy is indicated in the treatment of
chronic plaques psoriasis and pustular psoriasis.
Concerning the anatomical body zones affected,
psoriatic lesions can be observed on the scalp, palmoplantar sites,
genital and nail sites. Usually, the nail involvement is observed
in patients that often suffer from psoriatic arthritis as well
(3,8). Difficult to treat areas such as scalp,
palmoplantar sites or auricular sites are easy to access using the
excimer treatment. The ability to focus the radiation on the
affected area represents an advantage of the excimer laser over the
UVB narrow band.
Regarding the pathogenesis of psoriasis, many
theories have been considered over time. The latest information
concludes that an unknown trigger, on a genetically predisposed
individual, starts a cascade of inflammatory and immune responses
which lead to the formation of psoriatic plaques. Numerous immune
cells have been found to have certain functions in the devilment of
psoriatic lesions. Plasmacytoid dendritic cells production of
interferon-α, as well as tumor necrosis factor and interleukin 6
lead to the activation of dermal dendritic cells. These cells act
as cell-presenting antigen to the naïve T cells in the lymph nodes.
At that point, T cells differentiate into T helper 1 cells, T
helper 17 and T helper 22 cells. The migration from the lymph nodes
to the dermis through blood vessels, as well as lymphatics, is due
to different cytokines secreted by keratinocytes. It promotes the
formation of cutaneous lesions presented as psoriasis. The
inflammatory response is maintained by the secretion of
proinflammatory interleukins, nitric oxide radicals, vascular
endothelial growth factor and angiopoietin which cause
keratinocytic hyperproliferation and increased epidermal turnover.
The understanding of these key elements leads to better therapeutic
approaches (3,4).
Another aspect fitting the pathogenesis of psoriasis
is the more recent research based on studies on the cutaneous
microbiome. The importance of Streptococcal upper respiratory tract
infections are well known in the exacerbations of guttate
psoriasis. It has been considered that a structural analogy between
the K14 cytokeratin and the Streptococcal M protein is implicated
in the formation of new guttate plaques (5). Additional link between plaque formation
and the microorganisms that harbour our skin is demonstrated by the
application of Malassezia ovalisto suspensions to the perilesional,
unaffected, skin of an individual suffering from psoriasis. This
led to the formation of new psoriatic lesions that improved after
treatment with systemic antifungals (6).
The clinical appearance of psoriasis vulgaris
consists of well demarcated erythematous scally plaques, with
irregular outline, involving the elbows, knees, extensor surfaces
and scalp. Annular or gyrate figures are present when the plaques
coalesce, important characteristics which are valuable for the
diagnosis of psoriasis on the scalp or genital region. The abundant
white-silvery scales are easily removed, exposing small bleeding
points (Auspitz sign) which correspond to the dilated blood vessels
in the upper dermis (3).
Histologically, psoriasis is defined as epidermal
thickening as a result of keratinocyte proliferation. The epidermal
turnover is accelerated due to the releasing of multiple cytokines
by immune cells, especially T lymphocytes. In lesional skin,
dilated and elongated blood vessels are observed in the papillary
dermis. Perivascular infiltrate is observed consisting mainly of
lymphocytes and macrophages (3).
Lesion development in psoriatic patients involve a
strong connection between the innate and the adaptive immune
system. T helper cells are strongly involved in psoriatic
pathogenesis. The secreted cytokines such as interleukin-17,
interleukin-20, tumor necrosis factor-α, have implications in
maintaining the activation and hyperproliferation of keratinocytes,
angiogenesis and chemoattractant for inflammatory cells such as
neutrophils.
The cytotoxic role of the UVB treatments result in
immunosuppressive effects achieving clinical improvement in
psoriasis and in other inflammatory diseases.
Case report
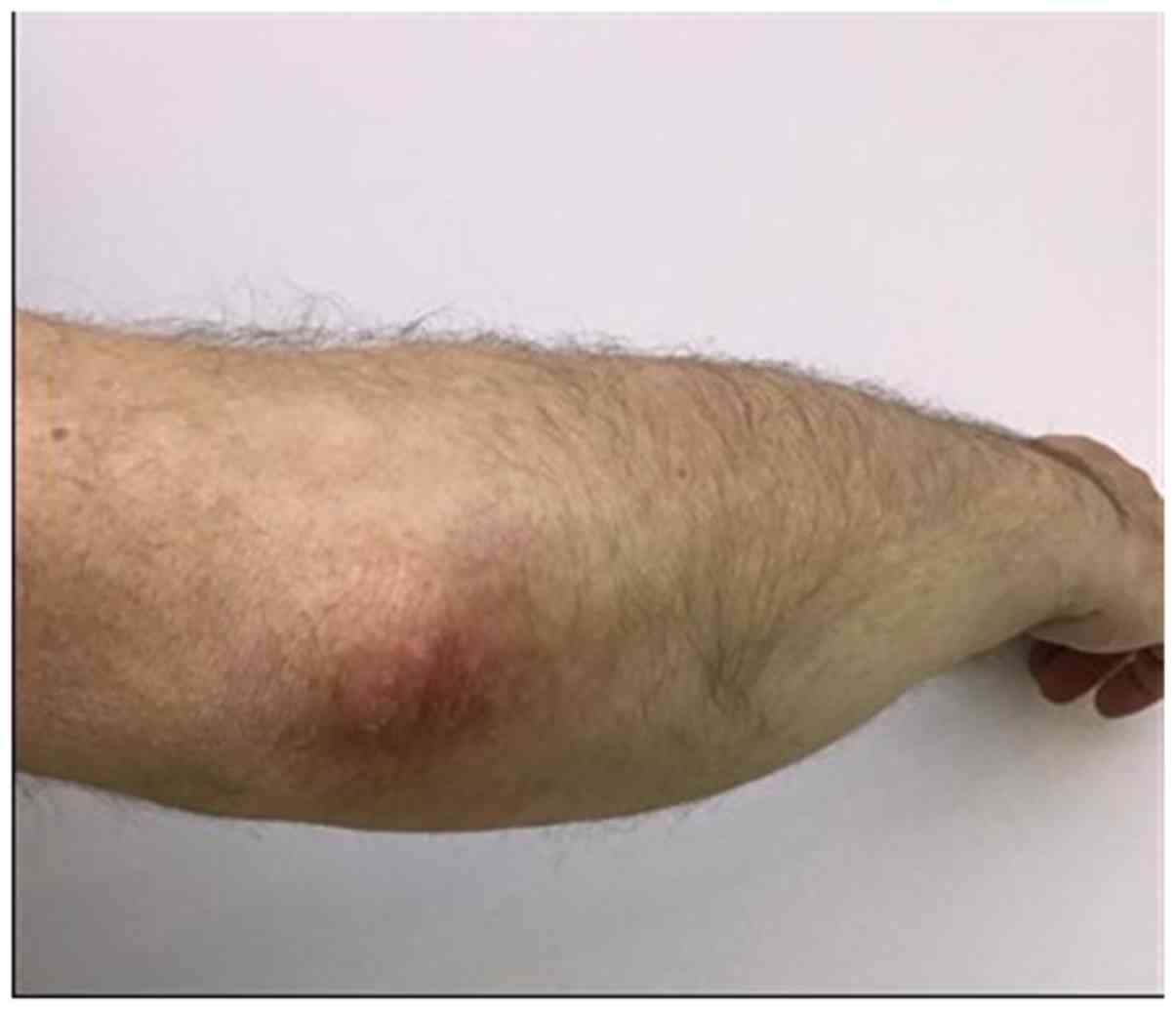
We present the case of a 62-year old, male patient,
which was referred to our clinic due to presence of widespread,
sharply demarcated, erythematous plaques, with adherent silvery
white scales on the surface of the lesions, irregularly shaped,
ranging from 4 to 8 cm, localised symmetrically on the elbows. The
lesions had a tendency to coalesce into larger plaques (Fig. 1).
On the scalp region, the patient presented discrete
erythematous scally patches, mainly in the temporal regions. The
patient reported the onset of the lesions since childhood and has
been in topical treatment with poor outcome. The treatment with
excimer laser was proposed. The used dose regimen for each session
was 400 mJ/cm2 according to minimal erythema dose
protocol. After 5 weeks, 1 session per week, the condition
significantly improved (Fig. 2).
The study was approved by the Ethics Committee of
the Romanian College of Physicians Galati County and the Aesthetic
Plastic Surgery Clinic. Written informed consent was obtained from
the patient prior to publication.
Discussion
Treatment options in psoriasis are divided in three
main groups: topical therapy, systemic therapy and phototherapy.
These therapies can be used separately or in combination. The
choice is based upon the body surface affected by the disease and
the patients' comorbidities.
The mechanism of action concerning phototherapy
implies depletion of lymphocytes, especially those in the
epidermis. It has been observed that after exposure to ultraviolet
light, T helper 1 lymphocyte response shifts to T helper 2 response
in lesional skin. The wavelength spectrum for psoriasis treatment
ranges between 300 and 313 nm as shown in previous studies.
The use of 308-nm excimer laser has multiple
purposes in dermatological diseases. It has been used in the
treatment of vitiligo, alopecia areata, lichen planus, atopic
dermatitis, eczema, prurigo and even mycosis fungoides (9,10). In
psoriasis it has shown efficiency in the treatment of recalcitrant
plaques localised especially on the knees and elbows. It is
indicated in moderate to severe psoriasis that affects <10% of
the body surface. Difficult to treat areas can be easily accessed
using the laser therapy such as nose, ears and palpebral region
that are hard to treat using conventional phototherapy. Other
differences between phototherapy and excimer laser consists of
lower UV exposer, decreased period of time of the treatment and the
possibility to focus on the lesional skin, avoiding unaffected
areas (11-13).
The 308-nm excimer laser induces lymphocytic
apoptosis and decreases the proliferation rate of these cells
obtaining a durable remission of the disease. Excimer derives from
‘excited dimer’ and is generated by a noble gas and halide
(10-12).
There are multiple protocols that evaluate the clinical response to
treatment: the induration protocol, the minimal erythema dose and
the minimal blistering dose.
The induration protocol refers to the treatment
dosing. Taneja et al (14)
used a primary dose regimen according to the induration of the
plaques. Therefore, the dose regimen can be modified with the
response to the treatment. The minimal erythema dose protocol
implies testing the unaffected skin of the patient until an
erythematous macule is obtained (15).
The minimal blistering dose regimen describes the
minimal dose at which a blister is formed. The consecutive dosing
regimens imply doses less powerful (16).
The PASI score improved more rapidly with the
minimal blistering dose protocol, which implied clearance of the
skin in a shorter period of time than the other protocols. The
patient should be advised about the side effects and the formation
of blisters (15,16). The adverse reactions reported after
treatment are moderate erythema, hypopigmentation,
hyperpigmentation, and the formation of vesicles, depending on the
protocols used (10,11). Also, the adverse reactions of the
medicines used to treat comorbidities and microbiome changes should
be considered (17-25).
Sometimes, if current available treatments for psoriasis fail or
adverse reactions occur, complementary and alternative methods of
treatment are available, psychological interventions and imaging
techniques are occasionally needed (26-29).
The use of the 308-nm excimer for recalcitrant
plaques of psoriasis laser represents a viable treatment
alternative. The immunosuppression obtained by the 308-nm excimer
laser can be explained by the lymphocytic apoptosis and the
decreases of proliferation rate of these cells. In this way a
durable remission of the disease can be obtained in a short period
of time, illustrated by using the minimal blistering dose
protocol.
The side effects of the 308-nm excimer such as
erythema, blistering or hyperpigmentation occur on the body area
treated despite using UVB narrow band. Regarding the cumulative
doses of radiation, the 308-nm excimer laser therapy implies less
radiation than UVB narrow band treatment. Compared to the UV
phototherapy, the 308-nm excimer laser focus on the lesional skin
and necessitate a lower exposure period.
In conclusion, the 308-nm excimer laser has been
demonstrated as a practical therapeutic option for difficult to
treat, resistant, psoriatic lesions. It is well tolerated, and the
side effects are dose dependent. It can be used as monotherapy or
combined with topical and systemic treatments. To establish the
possibility that the excimer laser could become a first line
treatment, further studies are required.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the present
study are available from the corresponding author on reasonable
request.
Authors' contributions
The authors all had equal participation and equal
rights to this article. VA examined, treated the subject and
performed clinical photos, DSR and ALT were major contributors in
writing the manuscript. VA, DSR and ALT were involved in all the
stages of the study. All authors contributed to the conception and
design of the study, as well as revising it. All authors read and
approved the final manuscript to be published and agreed to be
accountable for all aspects of the work in ensuring that questions
related to the accuracy or integrity of any part of the work.
Ethics approval and consent to
participate
The study was approved by the Ethics Committee of
the Romanian College of Physicians Galati County and the Aesthetic
Plastic Surgery Clinic. Written informed consent was obtained from
the patient prior to publication.
Patient consent for publication
Written informed consent was obtained from the
patient prior to publication.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
International Federation of Psoriasis
Associations: World Psoriasis Day, 2015. https://ifpa-pso.com/our-actions/world-psoriasis-day.
Accessed June 27, 2019.
|
|
2
|
Griffiths CEM, van der Walt JM, Ashcroft
DM, Flohr C, Naldi L, Nijsten T and Augustin M: The global state of
psoriasis disease epidemiology: A workshop report. Br J Dermatol.
177:e4–e7. 2017.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Bolognia J, Jorizzo JL and Schaffer JV
(eds): Dermatology. Elsevier Saunders, Philadelphia, PA, 2012.
|
|
4
|
Ayala-Fontánez N, Soler DC and McCormick
TS: Current knowledge on psoriasis and autoimmune diseases.
Psoriasis (Auckl). 6:7–32. 2016.PubMed/NCBI View Article : Google Scholar
|
|
5
|
McFadden J, Valdimarsson H and Fry L:
Cross-reactivity between streptococcal M surface antigen and human
skin. Br J Dermatol. 125:443–447. 1991.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Narang T, Dogra S, Kaur I and Kanwar AJ:
Malassezia and psoriasis: Koebner's phenomenon or direct causation?
J Eur Acad Dermatol Venereol. 21:1111–1112. 2007.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Enerbäck C, Martinsson T, Inerot A,
Wahlström J, Enlund F, Yhr M and Swanbeck G: Evidence that HLA-Cw6
determines early onset of psoriasis, obtained using
sequence-specific primers (PCR-SSP). Acta Derm Venereol.
77:273–276. 1997.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Raychaudhuri SK, Maverakis E and
Raychaudhuri SP: Diagnosis and classification of psoriasis.
Autoimmun Rev. 13:490–495. 2014.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Spencer JM and Hadi SM: The excimer
lasers. J Drugs Dermatol. 3:522–525. 2004.PubMed/NCBI
|
|
10
|
Mehraban S and Feily A: 308 nm excimer
laser in dermatology. J Lasers Med Sci. 5:8–12. 2014.PubMed/NCBI
|
|
11
|
Mavilia L, Mori M, Rossi R, Campolmi P,
Puglisi Guerra A and Lotti T: 308 nm monochromatic excimer light in
dermatology: Personal experience and review of the literature. G
Ital Dermatol Venereol. 143:329–337. 2008.PubMed/NCBI
|
|
12
|
Morita A, Weiss M and Maeda A: Recent
developments in phototherapy: Treatment methods and devices. Recent
Pat Inflamm Allergy Drug Discov. 2:105–108. 2008.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Abrouk M, Levin E, Brodsky M, Gandy JR,
Nakamura M, Zhu TH, Farahnik B, Koo J and Bhutani T: Excimer laser
for the treatment of psoriasis: safety, efficacy, and patient
acceptability. Psoriasis (Auckl). 6:165–173. 2016.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Taneja A, Trehan M and Taylor CR: 308-nm
excimer laser for the treatment of psoriasis: Induration-based
dosimetry. Arch Dermatol. 139:759–764. 2003.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Mudigonda T, Dabade TS and Feldman SR: A
review of protocols for 308 nm excimer laser phototherapy in
psoriasis. J Drugs Dermatol. 11:92–97. 2012.PubMed/NCBI
|
|
16
|
Kemény L, Bónis B, Dobozy A, Bor Z, Szabó
G and Ignácz F: 308-nm excimer laser therapy for psoriasis. Arch
Dermatol. 137:95–96. 2001.PubMed/NCBI
|
|
17
|
Tatu AL, Ciobotaru OR, Miulescu M, Buzia
OD, Elisei AH, Mardarea N, Diaconu C, Robu S and Nwabudike LC:
Hydrochlorothiazide: Chemical structure, therapeutic, phototoxic
and carcinogenetic effects in dermatology Rev. Chim. 69:2110–2114.
2018.
|
|
18
|
Nwabudike LC and Tatu AL: Response to -
chronic exposure to tetracyclines and subsequent diagnosis for
non-melanoma skin cancer in a large Mid-Western US population. J
Eur Acad Dermatol Venereol. 32:e159. 2018.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Tatu AL, Ionescu MA and Nwabudike LC:
Contact allergy to topical momethasone furoate confirmed by
rechallenge and patch test. Am J Ther. 25:e497–e498.
2018.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Gheorghe I, Tatu AL, Lupu I, Thamer O,
Cotar AI, Pircalabioru GG, Popa M, Cristea VC, Lazar V and
Chifiriuc MC: Molecular characterization of virulence and
resistance features in Staphylococcus aureus clinical strains
isolated from cutaneous lesions in patients with drug adverse
reactions. Rom Biotechnol Lett. 22:12321–12327. 2017.
|
|
21
|
Tatu AL and Nwabudike LC: Reply to: Kubiak
K, et al: Endosymbiosis and its significance in dermatology.
J Eur Acad Dermatol Venereol. 32:e346–e347. 2018.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Tatu AL and Cristea VC: Pityriasis
folliculorum of the back thoracic area: Pityrosporum, keratin
plugs, or Demodex involved? J Cutan Med Surg.
21(441)2017.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Buzia OD, Fasie V, Mardare N, Diaconu C,
Gurau G and Tatu AL: Formulation, preparation, physico-chimical
analysis, microbiological peculiarities and therapeutic challenges
of extractive solution of Kombucha. Rev Chim. 69:720–724. 2018.
|
|
24
|
Tatu AL and Cristea VC: Unilateral
blepharitis with fine follicular scaling. J Cutan Med Surg.
21(442)2017.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Irimie M, Oanţă A, Irimie CA, Fekete LG,
Minea DI and Pascu A: Cardiovascular risk factors in patients with
chronic plaque psoriasis: A case-control study on the Brasov County
population. Acta Dermatovenerol Croat. 23:28–35. 2015.PubMed/NCBI
|
|
26
|
Nwabudike LC and Tatu AL: Using
complementary and alternative medicine for the treatment of
psoriasis: A step in the right direction. JAMA Dermatol.
155(636)2019.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Nwabudike LC and Tatu AL: Response to:
Murphy EC, Nussbaum D, Prussick R, Friedman AJ. Use of
complementary and alternative medicine by patients with psoriasis.
J Am Acad Dermatol. 81(e105)2019.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Modrigan M, Draganescu M, Condratovici CP,
Pavel LL and Condratovici AP: Clinical personality patterns in
young adults with HIV nosocomial infection from the region of
Southeast Romania Mater. Plast. 54:175–179. 2017.
|
|
29
|
Batani A, Brănișteanu DE, Ilie MA, Boda D,
Ianosi S, Ianosi G and Caruntu C: Assessment of dermal papillary
and microvascular parameters in psoriasis vulgaris using in vivo
reflectance confocal microscopy. Exp Ther Med. 15:1241–1246.
2018.PubMed/NCBI View Article : Google Scholar
|