Introduction
A corneal stromal lenticule is a valuable biological
material obtained through small-incision lenticule extraction
(SMILE). It has been reported that SMILE-derived corneal stromal
lenticules can be used to treat corneal ulcers and perforations, to
effectively repair corneal defects and to improve the local
inflammatory response, and they have good surgical reproducibility
(1,2). Optical coherence tomography (OCT) can
be used to assess the depth and extent of corneal lesions, and it
may be possible to change the shape of the implant according to the
cornea condition as measured by OCT to improve surgical treatment
outcomes.
Keratoconus is a common progressive,
non-inflammatory corneal degenerative disease that usually occurs
in early adolescence (3). Corneal
collagen crosslinking can be used to control the progression of
keratoconus (4,5). However, certain patients with
advanced keratoconus do not have a corneal thickness of 400 µm,
which is the minimum thickness required for corneal crosslinking
surgery (6). Corneal thickness can
however be increased through the implantation of corneal stromal
lenticules. Corneal stromal lenticules have achieved good clinical
results in the treatment of keratoconus, but the curvature of
patients after lenticule implantation has been reported to increase
as a result (7-11).
The implantation of a convex lenticule derived from SMILE for
myopia causes a steeper curvature in patients with keratoconus,
which may lead to postoperative glass intolerance, poor rigid gas
permeable contact lens matching, difficulty in refractive
reconstruction and poor patient satisfaction. Nubile et al
(12) found that customizing
lenticules by increasing their asymmetry and tailoring their
re-shaping may improve implantation outcomes in cases of eccentric
keratoconus.
Presbyopia is the most common visual condition
affecting people over 40 years of age. Studies such as that by Liu
et al (13) suggested that
corneal stromal lenticule implantation may be a feasible and safe
treatment for presbyopia (14,15).
However, a major limitation is the thickness of the corneal stromal
lenticule, which depends on the refractive status of the donor
undergoing SMILE surgery. The number of available lenticules with
lower refraction is limited. A study indicated that only 15 out of
424 patients (3.54%) with presbyopia had lenticules suitable for
reimplantation (16). In addition,
in patients with high myopia and thin corneas who are unwilling to
undergo implantable collamer lens treatment, the corneal stromal
lenticule can also be remodeled into a concave lens or a ‘donut’
and then implanted into a capsule created using a femtosecond laser
to correct refractive error. Therefore, if corneal stromal
lenticule implantation is a useful treatment for refractive and
corneal diseases, it would be beneficial to develop a technique
that meets the clinical need for corneal stromal lenticule
thickness distribution and enables its remodeling.
The corneal stromal lenticule is the anterior layer
of the central corneal stromal layer. It is composed of collagen
fibers arranged regularly. Its normal anatomical structure and
physiological function maintain the light transmittance and
biomechanics of the cornea; therefore, it has good plasticity. Luft
et al (17) assessed wound
healing, inflammation and tissue ultrastructure in the human
corneal stroma after SMILE and femtosecond laser-assisted in
situ keratomileusis (FS-LASIK), and found that both procedures
elicited virtually identical and minimal keratocyte activation,
cell death or inflammation, with the stromal bed exhibiting a
smoother surface texture after LASIK. This demonstrates that the
excimer laser has little effect on the matrix and can therefore be
used to reshape the corneal stromal lenticule according to the
patient's needs. However, there are few available studies on
ultrastructural changes after corneal stromal lenticule shaping.
The microstructure and light transmittance of the corneal stromal
lenticule after excimer laser shaping are essential for predicting
postoperative patient satisfaction, as they may be associated with
better optical quality, reduced inflammatory responses and faster
recovery. Therefore, this study used microcode to observe changes
in the light transmittance and morphological structure of corneal
stromal lenticules after shaping under an optical microscope.
Patients and methods
Study subjects and groups
This study involved 30 patients aged 19.68±1.79
years (range, 18 to 27 years) who underwent SMILE surgery at Jinan
Mingshui Eye Hospital (Jinan, China) during July 2024, including a
total of 40 eyes. All patients voluntarily came to Jinan Mingshui
Eye Hospital (Jinan, China) for refractive surgery, and none of
them had received any treatment for any eye condition. A complete
ophthalmological examination was performed before the surgery. Eyes
were grouped according to the experimental design; the same
thickness was required to be ascertained for experimental group 1
and control group 1 before corneal stromal lenticules shaping, and
for experimental group 2 and control group 2 the same thickness was
required to be ascertained after shaping. The removed corneal
stromal lenticules were divided into an experimental group
requiring excimer cutting and a control group without excimer
cutting. Tissues from experimental group 1 and control group 1 were
examined under an optical microscope after hematoxylin and eosin
(HE) staining (6 eyes in each group). The diopters of both groups
were consistent before laser shaping [experimental group 1:
-5.04±0.69 (range: -5.88 to -4.25D), control group 1: -5.23±0.65
(range: -6.13 to -4.38D)]. Light transmittance was measured for
experimental group 2 and control group 2 (14 eyes in each group)
using a microcoder to ensure that lenticule thickness was
comparable between the two groups after laser plasticity. The
equivalent spherical lens for experimental group 2 was -6.511±0.412
(range, -7.25 to -5.50D). The equivalent spherical mirror for the
control group was -3.843±0.405 (range, -4.38 to -3.25D). The study
protocol adhered to the principles of the Declaration of Helsinki
and was approved by the Medical Ethics Committee of Jinan Mingshui
Eye Hospital (Jinan, China; Ref. Ethics/2024/004). All participants
or their legal guardians consented to the use of the corneal
stromal lenticules produced during their surgery for this
study.
The inclusion criteria were as follows: i) The
patient had a desire to discoutinue glasses and had reasonable
expectations regarding surgical outcomes; ii) age, 17-30 years;
iii) stable dioptric state and an annual increase of the myopia
dioptric number within two years not exceeding 0.5D; iv) column
lens degree ≤1.00D; v) adequate pupil diameter (bright pupil ≤5 cm,
dark pupil ≤8 cm); vi) the patient had discontinued the use of soft
contact lenses for at least 10 days, of hard contact lenses for at
least a month and of orthokeratology lenses for at least three
months.
The following exclusion criteria were applied: i)
The patient was unable to place the head in a normal position; ii)
previous cornea-related surgery; iii) presence or family history of
keratoconus or glaucoma; iv) pregnancy or being at the
breastfeeding stage; v) other eye diseases or diabetes, systemic
immune diseases or neuropsychiatric disorders.
Corneal stromal lenticule acquisition
process
All patients underwent detailed ophthalmological
examinations and all procedures were performed by the same
experienced physician. Levofloxacin eye drops (Levofloxacin
Bromofenac sodium, Ruilin) were routinely used 1 day before the
operation. After routine conjunctival sac irrigation and periocular
disinfection before surgery, promecaine hydrochloride eye drops
(Unitel Nanjing Pharmaceutical Co., Ltd) were used for surface
anesthesia. Femtosecond laser for lenticule and small incision was
performed with a Visumax 500 kHz femtosecond Laser System (Carl
Zeiss AG); the energy was 130 nJ, the lenticule cutting diameter
was 6.5 mm, the corneal cap thickness was 120 µm and the length of
the small incision was 2 mm.
Corneal stromal lenticule laser
remodeling
The stromal lenticule was placed on the plate and
1-2 drops of 0.09% saline were applied to flatten it. Excess water
was quickly absorbed and the stromal lenticule was placed on the
Amaris excimer machine (Schwind Amaris 500E; Schwind) for excimer
cutting. The cutting optical area was set to 4 mm and excimer
cutting with refractive parameter 1:1 (that is, the diopter of the
excimer cutting design is equal to the effective diopter of the
lenticules) was performed based on the lenticule's equivalent
spherical power. The entire process was completed within two
minutes.
Fixation of corneal stromal lenticule
and optical observation
After the corneal stromal lenticule was removed, it
was fixed with 10% paraformaldehyde at 20˚C for 24 h and dehydrated
using an ethanol gradient. The tissue was encased in wax blocks and
sections (thickness, 3-5 µm) were prepared with a microtome. A
group of good slices was taken up with tweezers and placed on the
surface of the water in the slot of a sheet spreading machine
(water temperature, 40-45˚C); they were allowed to stretch
naturally and after the slices were flattened, the best slice was
separated. A clean slide of the corresponding tissue, which had
been numbered, was inserted into the water near the slice at an
angle, and it was slowly lifted to make the slice adhere to the
slide. The slide was baked at 37˚C for 24-48 h. Dewaxing and
rehydration were performed with xylene, an ethanol series and
steaming water. The sample was stained with hematoxylin and eosin
according to standard methods and sealed with neutral gum for light
microscopic observation.
Corneal stromal lenticule light
transmittance measurement
To ensure that the predicted thickness of the two
groups of corneal stromal lenticules was the same and to prevent
lenticule thickness from affecting light transmittance, the
predicted thickness of the control group was the thickness of the
corneal stromal lenticule calculated according to the Zeiss full
femtosecond laser surgery system (Carl Zeiss AG). The predicted
thickness of experimental group 2 was the thickness of the corneal
stromal lenticule calculated using the Zeiss full femtosecond laser
surgery system minus the laser cutting thickness calculated using
the Amaris excimer laser surgery system. The prepared corneal
stromal lenticule was placed in front of the OCT to measure its
actual thickness (the measurement was completed within one minute).
After the measurement was completed, 0.09% normal saline was
immediately placed into the corneal stroma lenticules, which were
then placed flat in a 96-well plate, and three drops of 0.09%
normal saline were added to completely cover the corneal stromal
lenticule. The absorbance of the corneal stromal lenticule was
measured using a microcoder at wavelengths of 350, 450 and 600 nm,
and each lens was measured three times. Measurements were completed
within 2 h. A greater absorbance measured was associated with a
worse light transmittance of the corneal stromal lenticule, while a
smaller absorbance, was associated with a better light
transmittance of the corneal stromal lenticule.
Statistical analysis
All data were analyzed using IBM SPSS Statistics for
Windows, version 27.0 (IBM Corp.). The normality of data
distribution was assessed with the Shapiro-Wilk test. If a normal
distribution and homogeneity of variance were met, an
independent-samples t-test was used. If not consistent with a
normal distribution and homogeneity of variance, the Mann-Whitney
U-test was used. Nonparametric values were expressed as n (%) and
compared using Fisher's exact test. P<0.05 was considered to
indicate a statistically significant difference.
Results
Basic information statistics of
patients
Demographic data and clinical statistics of patients
analyzed via optical microscopy revealed no significant differences
in age, sex or refraction between experimental group 1 and control
group 1 (Table I). For patients
undergoing light transmittance measurements, no statistically
significant differences were observed in age, sex, predicted
thickness or actual measured thickness between experimental group 2
and control group 2, while there were statistically significant
differences in diopters (Table
II).
 | Table IBasic information statistics of
patients undergoing optical microscopy. |
Table I
Basic information statistics of
patients undergoing optical microscopy.
| Variable | Totals (n=12) | Experimental group 1
(n=6) | Control group 1
(n=6) | t/Z -value | P-value |
|---|
| Agea, years | 18.92±0.79 | 18.5±0.55 | 19.33±0.82 | -1.791 | 0.073 |
| Sex | | | | 0 | >0.999 |
|
Males | 8 (66.7) | 4 (66.7) | 4 (66.7) | | |
|
Females | 4 (33.3) | 2 (33.3) | 2 (33.3) | | |
| Diopters | -5.138±0.664 | -5.043±0.68521 | -5.232±0.649 | -0.489 | 0.636 |
 | Table IIBasic information statistics of
patients with light transmittance measurements. |
Table II
Basic information statistics of
patients with light transmittance measurements.
| Variable | Totals (n=28) | Experimental group 2
(n=14) | Control group 2
(n=14) | t/Z-value | P-value |
|---|
| Agea, years | 20±2.00 | 20.5±2.35 | 19.5±1.50 | -1.636 | 0.102 |
| Sex | | | | 0 | >0.999 |
|
Males | 18 (64.3) | 9 (64.3) | 9 (64.3) | | |
|
Females | 10 (35.7) | 5 (35.7) | 5 (35.7) | | |
| Dioptersa | -5.18±1.42 | -6.51±0.41 | -3.84±0.41 | -4.521 | <0.001 |
| Predicted
thicknessa, µm | 89.82±5,80 | 90.36±4.09 | 89.29±7.24 | -0.254 | 0.799 |
| Actual measured
thickness, µm | 164.536±9.143 | 162.857±166.214 | 166.214±12.04 | -0.970 | 0.341 |
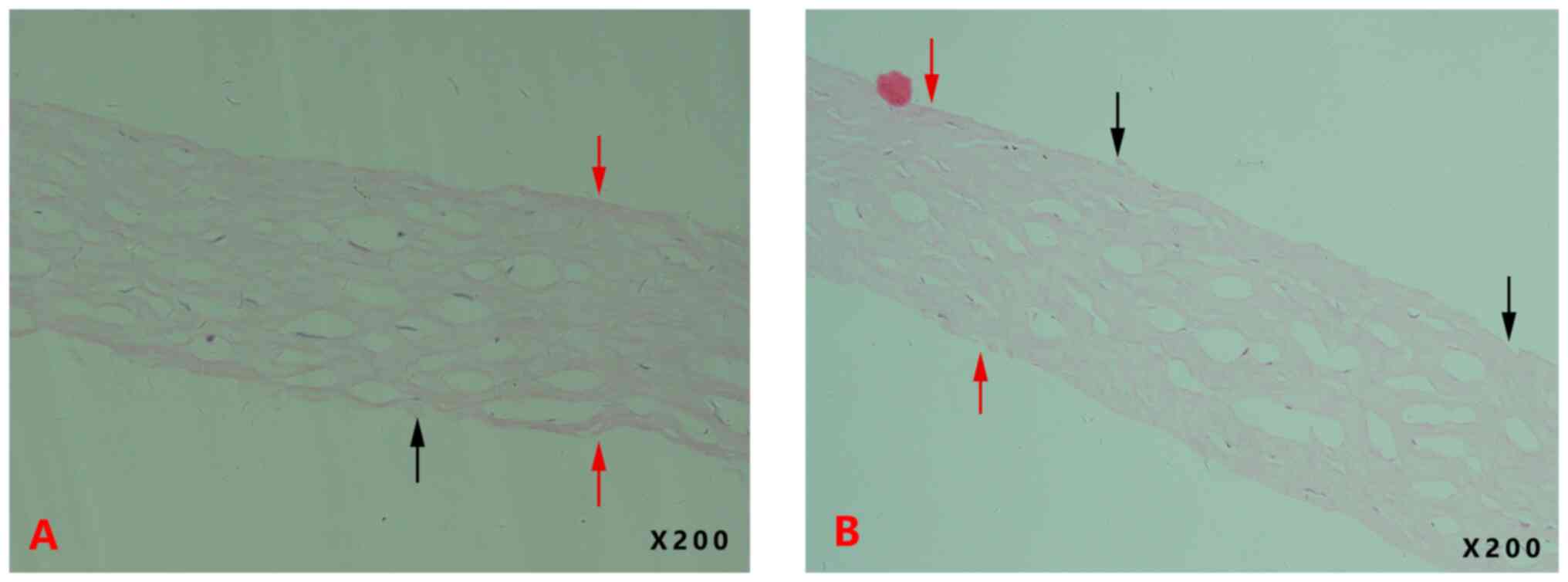
Optical microscopy results
The surface of the corneal stromal lenticules was
observed to exhibit burrs, broken fibers and bubbles under the
optical microscope. In experimental group 1, there was no visible
edema in the central area of the cornea and the stromal layer
fibers were arranged regularly (Fig.
1A). Control group 1 showed no significant edema in the central
cornea and the stromal layer fibers were also arranged regularly. A
comparison between experimental group 1 and control group 1
revealed no obvious abnormalities (Fig. 1B).
Microplate reader results
The difference in absorbance between experimental
group 2 and control group 2 was statistically significant
(P<0.05; Table III). The
absorbance of the corneal stromal lenticule in control group 2 was
greater than that in experimental group 2, indicating improved
light transmittance of the reshaped corneal stromal lenticule.
 | Table IIIComparison of absorbance [l/(g x cm)]
between control group 2 and experimental group 2. |
Table III
Comparison of absorbance [l/(g x cm)]
between control group 2 and experimental group 2.
| Wavelength, nm | Experimental group
2 | Control group
2 | t/Z-value | P-value |
|---|
| 350 | 0.243±0.023 | 0.261±0.016 | 2.307 | 0.029 |
| 450a | 0.095±0.01 | 0.105±0.008 | -2.924 | 0.003 |
| 600 | 0.069±0.006 | 0.075±0.005 | 3.205 | 0.004 |
Discussion
In corneal refractive surgery, femtoseconds achieve
a high energy density within a small area due to the strong
focusing ability of their ultrashort laser pulses. At high energy
density, the electrons and atoms in matter are separated, producing
light blasting inside the tissue, thus generating bubbles to
separate the tissue (18). The
corneal stromal lenticule is the anterior layer of the central
corneal stromal layer. It is composed of orderly arranged collagen
fibers. Its normal anatomical structure and physiological functions
ensure corneal light transmittance and biomechanics, providing
excellent plasticity. Numerous studies have shown that the smooth
surface of the corneal stromal lenticule prepared using the
femtosecond laser system exhibits predictable and high surface
quality (19,20). Excimer laser can cut the corneal
tissue with high precision, does not affect the tissue outside the
cutting area and is safe (21);
therefore, the excimer laser is used to reshape the corneal stromal
lenticule. Currently, there is a lack of research on the corneal
stromal lenticules after molecular shaping. In this experiment, an
optical microscope was used to observe the HE-stained tissue
sections and the absorbance of the microcode to explore whether the
corneal stromal lenticule microstructure changed after excimer
laser remodeling.
The surface of the lenticules was observed under the
optical microscope to exhibit burrs, broken fibers and bubbles, in
agreement with the results of previous studies (22-24).
During SMILE surgery, the lenticule surface is the ablating focus
of the femtosecond laser, and the photo-decomposing function of the
femtosecond laser makes it possible to break the chemical bonds
between molecules, resulting in a number of bubbles. Once the
bubbles expand and merge to form a separate plane in the corneal
tissue, the corneal stroma may be separated (18,25).
Some of the bubbles may be partially absorbed by the surrounding
corneal tissue or diffuse into the air, while the remaining ones
tend to become fixed in the tissue, as observed in the corneal
stroma lens under optical microscopy. Under optical microscopy, the
presence of edema of the corneal stromal lenticule and the fiber
arrangement of the stroma were observed. Thermal damage to corneal
tissue, if present, would be indicated by deep staining or tissue
loss in HE-stained tissue sections. No significant differences in
the degree of edema and stromal layer fiber arrangement were noted
between the two groups. The reasons why there is no difference
between the two groups are speculated to be the low excimer laser
energy, emitted energy in the order of nanojoules and a very short
time of action. Therefore, when the laser thermal effect and heat
transfer focused on the tissue are small, the instantaneous thermal
damage and mechanical damage to the corneal tissue can be
minimized, so the excimer laser shaping minimally damages the
corneal stromal lenticule.
Corneal light transmittance is a critical property
of a healthy cornea, reflecting changes such as edema or
inflammation, which may lead to opacity, increased corneal density
and reduced corneal light transmittance. Therefore, corneal light
transmittance serves as a valuable indicator of early corneal
pathological changes and can be used to monitor the postoperative
stromal response and keratinocyte activation. It is a reliable
predictor of visual acuity and visual quality (26,27).
In the present study, the absorbance of the corneal stromal
lenticules was measured using a microcoder and the light
transmittance of the stromal lenticules was evaluated. The results
indicated that the lenticule light transmittance after excimer
shaping was better under the condition that there was no
statistically significant difference in lenticule thickness between
the experimental group 2 and the control group 2 after excimer
shaping. Before Agca et al (28) used live confocal microscopy and
compared SMILE with FS-LASIK, it was found that corneal light
transmittance after FS-LASIK was better than that after SMILE. On
the one hand, this may be due to a smoothing effect of the excimer
laser ablation that is implicit in the FS-LASIK technique. On the
other hand, the less straightforward surgical dissection of the
lenticule plane in SMILE through a 3-mm incision compared with the
flap-lifting maneuver in FS-LASIK must not be overlooked as a
contributing factor to the increased roughness of the lenticule
bed. Lazaridis et al (29),
Han et al (30) and Wei
et al (31), using
Scheimpflug corneal densitometry, compared the corneal light
transmittance after SMILE and FS-LASIK and found a shorter
postoperative corneal density and more transparent cornea after
FS-LASIK. These findings are consistent with the present results,
which showed improved lenticule light transmittance following
excimer laser shaping. This discrepancy may result from the
differing mechanisms of action between the two surgical methods. In
SMILE, femtosecond lasers primarily use photo disruption to
generate plasma, shock waves and cavitation bubbles. However, in
FS-LASIK, in the process of excimer laser photoablation, when the
excimer laser destroys the organic molecular bond in the corneal
tissue, unlike the femtosecond laser, the 193 nm wavelength light
pulse is absorbed by the corneal tissue, causing thermal and
secondary radiation damage. The total energy applied to the corneal
stroma during SMILE was higher than that applied to the corneal
stroma during LASIK using the same platform.
In summary, to better use corneal stromal lenticule
implantation as a treatment method for refractive and corneal
diseases in the future, an excimer laser was selected in the
present study to cut the corneal stromal lenticule. The convex
lenticule of the corneal matrix can be shaped into a parallel or a
concave lenticule. In this way, the thickness of the cornea in
patients with keratoconus can be increased and curvature of the
cornea can be avoided, which is more conducive to refractive
reconstruction. The corneal matrix lenticule can also be shaped and
reused according to the needs of individual patients, and instead
of thinning and weakening, corneal laser surgery can be used
instead to thicken and strengthen the tissue, providing a new
treatment alternative for patients with thin corneal ametropia. In
the present study, optical microscopy and light transmittance
detection of the cut corneal stromal lenticule were performed. The
degree of edema and the regularity of the matrix fiber arrangement
did not change after excimer cutting. The absorbance decreased and
the light transmittance improved. However, this study only examined
the corneal stromal lenticule in vitro and did not explore a
series of changes after implantation into the receptor pouch.
Further studies are needed to determine whether the ideal
refractive correction effect can be achieved after excimer shaping
and whether corneal biomechanics can be effectively increased.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The data generated in the present study may be
requested from the corresponding author.
Authors' contributions
YL contributed to the conception and design of the
study. ML, JH, JZ, LY, XL and XW acquired and interpreted study
data. XW conducted statistical analysis and drafted the manuscript.
YL and JH provided critical manuscript revisions, as well as
administrative and technical support. YL supervised the study. All
authors read and approved the final manuscript. YL and XW checked
and confirmed the authenticity of the raw data.
Ethics approval and consent to
participate
The study protocol conformed to the tenets of
Declaration of Helsinki and was approved by the Human Ethics
Committee of Jinan Mingshui Eye Hospital (Jinan, China; approval
no. Ethics/2024/004). All of the adult study participants consented
to the use of the corneal stromal lenticules obtained during their
surgery for this study.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Jiang Y, Li Y, Liu XW and Xu J: A novel
tectonic keratoplasty with femtosecond laser intrastromal lenticule
for corneal ulcer and perforation. Chin Med J (Engl).
129:1817–1821. 2016.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Wu F, Jin X, Xu Y and Yang Y: Treatment of
corneal perforation with lenticules from small incision lenticule
extraction surgery: A preliminary study of 6 patients. Cornea.
34:658–663. 2015.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Ferrari G and Rama P: The keratoconus
enigma: A review with emphasis on pathogenesis. Ocul Surf.
18:363–373. 2020.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Wollensak G, Spoerl E and Seiler T:
Riboflavin/ultraviolet-a-induced collagen crosslinking for the
treatment of keratoconus. Am J Ophthalmol. 135:620–627.
2003.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Chen T, Wu CF and Yin YP: Corneal collagen
crosslinking for advanced keratoconus. Practical Blind Prevention
Techniques. 11:89–82. 2016.
|
|
6
|
Wollensak G, Spörl E, Reber F, Pillunat L
and Funk R: Corneal endothelial cytotoxicity of riboflavin/UVA
treatment in vitro. Ophthalmic Res. 35:324–328. 2003.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Zhao J, Shang J, Zhao Y, Fu D, Zhang X,
Zeng L, Xu H and Zhou X: Epikeratophakia using small-incision
lenticule extraction lenticule addition combined with corneal
crosslinking for keratoconus. J Cataract Refract Surg.
45:1191–1194. 2019.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Wang KN, Fu MJ, Zhao JJ, Wang YC, Wang JH,
Zhang HR and Wang R: Corneal surface mirror (stromal lens)
implantation combined with corneal collagen cross-linking for the
treatment of keratoconus: A case report. J Clin Ophthalmol.
30:552–553. 2022.
|
|
9
|
Sun X, Shen D, Cai J, Zhang CN and Wei W:
A case of keratoconus treated by femtosecond laser assisted
implantation of corneal allogenic matrix lens combined with corneal
collagen crosslinking. Chin J Optometry Ophthalmol Visual Sci.
24:472–474. 2022.
|
|
10
|
Li M, Yang D, Zhao F, Han T, Li M, Zhou X
and Ni K: Thirty-month results after the treatment of post-LASIK
ectasia with allogenic lenticule addition and corneal
cross-linking: A case report. BMC Ophthalmol.
18(294)2018.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Ganesh S and Brar S: Femtosecond
intrastromal lenticular implantation combined with accelerated
collagen Cross-Linking for the treatment of Keratoconus-initial
clinical result in 6 eyes. Cornea. 34:1331–1339. 2015.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Nubile M, Alio Del Barrio JL, Cerino L,
Salgari N, El Zarif M, Totta M, Lanzini M and Mastropasqua L: Ex
vivo lenticule customization for stromal lenticule addition
keratoplasty. Invest Ophthalmol Vis Sci. 65(9)2024.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Liu YC, Teo EPW, Ang HP, Seah XY, Lwin NC,
Yam GHF and Mehta JS: Biological corneal inlay for presbyopia
derived from small incision lenticule extraction (SMILE). Sci Rep.
8(1831)2018.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Lim CH, Riau AK, Lwin NC, Chaurasia SS,
Tan DT and Mehta JS: LASIK following small incision lenticule
extraction (SMILE) lenticule re-implantation: A feasibility study
of a novel method for treatment of presbyopia. PLoS One.
8(e83046)2013.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Jacob S, Kumar DA, Agarwal A, Agarwal A,
Aravind R and Saijimol AI: Preliminary evidence of successful near
vision enhancement with a new technique: PrEsbyopic allogenic
refractive lenticule (PEARL) corneal inlay using a SMILE lenticule.
J Refract Surg. 33:224–229. 2017.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Yuen LH, Chan WK, Koh J, Mehta JS and Tan
DT: SingLasik Research Group. A 10-year prospective audit of LASIK
outcomes for myopia in 37,932 eyes at a single institution in Asia.
Ophthalmology. 117:1236–1244.e1. 2010.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Luft N, Schumann RG, Dirisamer M, Kook D,
Siedlecki J, Wertheimer C, Priglinger SG and Mayer WJ: Wound
healing, inflammation, and corneal ultrastructure after smile and
femtosecond Laser-Assisted LASIK: A human ex vivo study. J Refract
Surg. 34:393–399. 2018.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Sugar A: Ultrafast (femtosecond) laser
refractive surgery. Curr Opin Ophthalmol. 13:246–249.
2002.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Kunert KS, Blum M, Duncker GI, Sietmann R
and Heichel J: Surface quality of human corneal lenticules after
femtosecond laser surgery for myopia comparing different laser
parameters. Graefes Arch Clin Exp Ophthalmol. 249:1417–1424.
2011.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Zhao Y, Li M, Sun L, Zhao J, Chen Y and
Zhou X: Lenticule quality after continuous curvilinear
lenticulerrhexis in SMILE evaluated with scanning electron
microscopy. J Refract Surg. 31:732–735. 2015.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Van Mellaert CE and Missotten L: On the
safety of 193-nanometer excimer laser refractive corneal surgery.
Refract Corneal Surg. 8:235–239. 1992.PubMed/NCBI
|
|
22
|
Yin Y, Hu T, Xiang A, Fu Y, Zhao Y, Wu X,
Wu X and Wen D: A microscopic study of the corneal stromal
lenticules extracted during femtosecond laser-assisted small
incision lenticule extraction. Exp Ther Med. 22(681)2021.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Sumioka T, Miyamoto T, Takatsuki R, Okada
Y, Yamanaka O and Saika S: Histological analysis of a cornea
following experimental femtosecond laser ablation. Cornea. 33
(Suppl 11):S19–S24. 2014.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Zhao J, Miao H, Han T, Shen Y, Zhao Y, Sun
L and Zhou X: A pilot study of SMILE for hyperopia: Corneal
morphology and surface characteristics of concave lenticules in
human donor eyes. J Refract Surg. 32:713–716. 2016.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Vossmerbaeumer U and Jonas JB: Structure
of intracorneal femtosecond laser pulse effects in conical incision
profiles. Graefes Arch Clin Exp Ophthalmol. 246:1017–1020.
2008.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Schaub F, Gerber F, Adler W, Enders P,
Schrittenlocher S, Heindl LM, Cursiefen C and Bachmann BO: Corneal
densitometry as a predictive diagnostic tool for visual acuity
results after descemet membrane endothelial keratoplasty. Am J
Ophthalmol. 198:124–129. 2019.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Patel SV, McLaren JW, Hodge DO and Bourne
WM: The effect of corneal light scatter on vision after penetrating
keratoplasty. Am J Ophthalmol. 146:913–919. 2008.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Agca A, Ozgurhan EB, Yildirim Y, Cankaya
KI, Guleryuz NB, Alkin Z, Ozkaya A, Demirok A and Yilmaz OF:
Corneal backscatter analysis by in vivo confocal microscopy: Fellow
eye comparison of small incision lenticule extraction and
femtosecond laser-assisted LASIK. J Ophthalmol.
2014(265012)2014.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Lazaridis A, Droutsas K, Sekundo W, Petrak
M and Schulze S: Corneal clarity and visual outcomes after
small-incision lenticule extraction and comparison to femtosecond
Laser-assisted in situ keratomileusis. J Ophthalmol.
2017(5646390)2017.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Han T, Zhao J, Shen Y, Chen Y, Tian M and
Zhou X: A Three-year observation of corneal backscatter after small
incision lenticule extraction (SMILE). J Refract Surg. 33:377–382.
2017.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Wei R, Li M, Yang W, Shen Y, Zhao Y, Fu D,
Shang J, Zhang J, Choi J and Zhou X: Corneal densitometry after
small incision lenticule extraction (SMILE) and femtosecond
Laser-assisted LASIK (FS-LASIK): 5-year prospective comparative
study. Front Med (Lausanne). 7(521078)2020.PubMed/NCBI View Article : Google Scholar
|