Introduction
Quality improvement (QI) is a critical aspect of advancing patient care, enhancing outcomes and ensuring the highest standards of safety and efficiency in surgical practices (1-4). Neurosurgery, with its inherent complexities and high risks, demands attention to detail and a persistent pursuit of excellence. Severe perioperative complications in neurosurgical patients can lead to considerable harm, morbidity, permanent disability, or even mortality. The recovery period following such procedures is frequently complex, requiring extended rehabilitation and the use of expensive specialized resources (2-5). The field has seen notable advancements over the years, driven by innovative surgical techniques, cutting-edge technology and a deeper understanding of neurological conditions (3). However, the complexity and risks associated with neurosurgical procedures require a robust framework for continuous QI. This involves systematically identifying areas for enhancement, implementing evidence-based interventions, and rigorously evaluating outcomes to ensure sustained improvements (5). In this context, QI initiatives aim to reduce complications, optimize patient recovery, and enhance overall surgical success rates, thereby elevating the standard of care for patients (6).
Despite the presence of numerous systematic reviews on various types of surgeries, such as otolaryngology-head and neck surgeries, cleft palate surgeries and laparoscopic surgeries (7-9), current systematic reviews for QI dedicated to neurosurgery have not been established, at least to the best of our knowledge. The present systematic review thus aimed to explore existing evidence, gaps in current practices and standardized QI measures utilized in neurosurgery.
Data and methods
For the present systematic review, articles were selected based on a set of predetermined key words, including ‘Quality’, ‘Control’, ‘Improvement’, ‘Neurosurgical’ and ‘Neurosurgery’. These key words were strategically selected to ensure a comprehensive search and capture all relevant studies within the scope of neurosurgical quality control and improvement. In order to gather the scientific publications, the key words were applied across six major internet search databases: PubMed, Google Scholar, Scopus, Wiley, ScienceDirect and Microsoft Academic. These databases were selected due to their extensive repositories and relevance to the field. Initially, a total of 391 scientific publications were retrieved from these databases. During the initial review, 31 articles were found to be duplicates and were subsequently removed, leaving a total of 360 unique papers for further screening (Fig. 1). The screening process was meticulous and involved a detailed examination of the relevance of each article to the inclusion and exclusion criteria set by the research team. In order to maintain the meticulousness of the screening process at a high level, all reviews and studies that tended to provide information on new interventions to improve the quality of services in neurosurgery were included; articles that discussed non-neurosurgical interventions and were not related to QI were excluded.
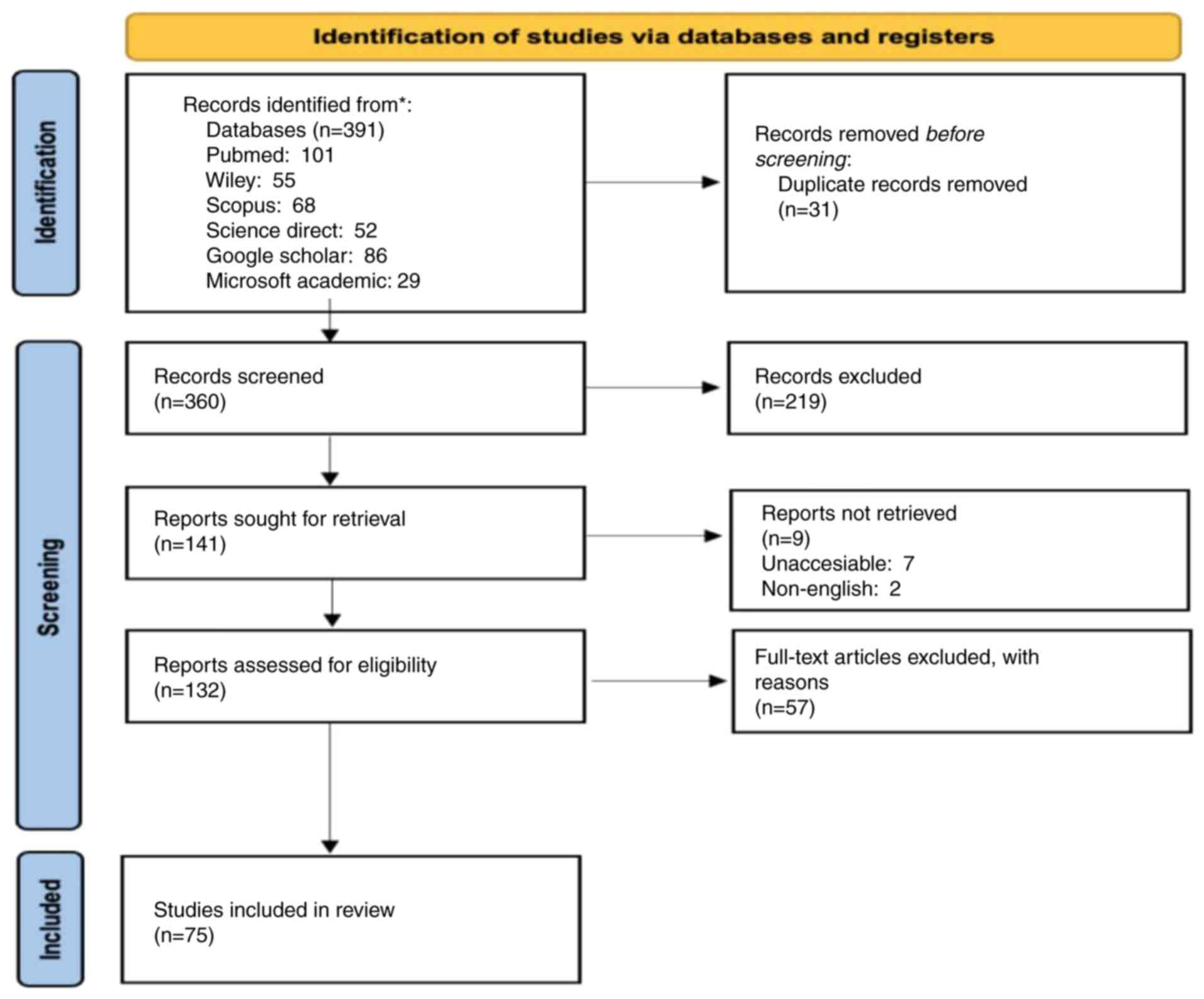 |
Figure 1
PRISMA flow diagram illustrating the process of article inclusion and exclusion for the present systematic review.
|
This process narrowed the selection down to 75 publications deemed most pertinent for inclusion in the systematic review. The selected scientific articles were found to fall between 2004 and 2023. Although there was no time frame restriction, there were no further articles located prior to that time frame. This 19-year period provided a comprehensive overview of the developments and trends in neurosurgical quality control and improvement. During the screening stage, only articles written in the English language were considered, resulting in the exclusion of two non-English publications. This decision was made to maintain consistency and ensure that all reviewed articles were accessible to the research team.
Results
The 75 publications (listed in Table I) (2,4,5,10-81) revealed an uneven distribution across four main fields of neurosurgery. Adult neurosurgery encompassed the largest proportion of 70.5%, accounting for 53 articles (2,4,5,13,14,16-23,26-29,31-33,35-40,45,48,50-55,57-65,67-70,72-77). This was followed by spine surgery with 17 articles (22.5%) (10-12,24,30,41-44,46,47,56,71,78-81), pediatric neurosurgery with three articles (4%) (15,25,34) and neuro-oncology exclusive studies with the lowest proportion of 3%, representing two articles (49,66) (Table I and Fig. 2). There was also a marked disparity in the distribution of targeted patients (n=621,293) across the different fields of neurosurgery. QI studies focusing on spinal-only cases comprised the vast majority of patients at 87.07% (n=540,955) (10-12,24,30,41-44,46,47,56,71,78-81), while cranial-only studies and combined cranial and spinal studies accounted for 0.21% of the total patients collectively (n=1,309) (2,4,5,13,14,16-23,26-29,31-33,35-40,45,48,50-55,57-65,67-70,72-77). Additionally, the unspecified category accounted for 12.72% (73,29) of patients (15,25,34,49,66) (Table II).
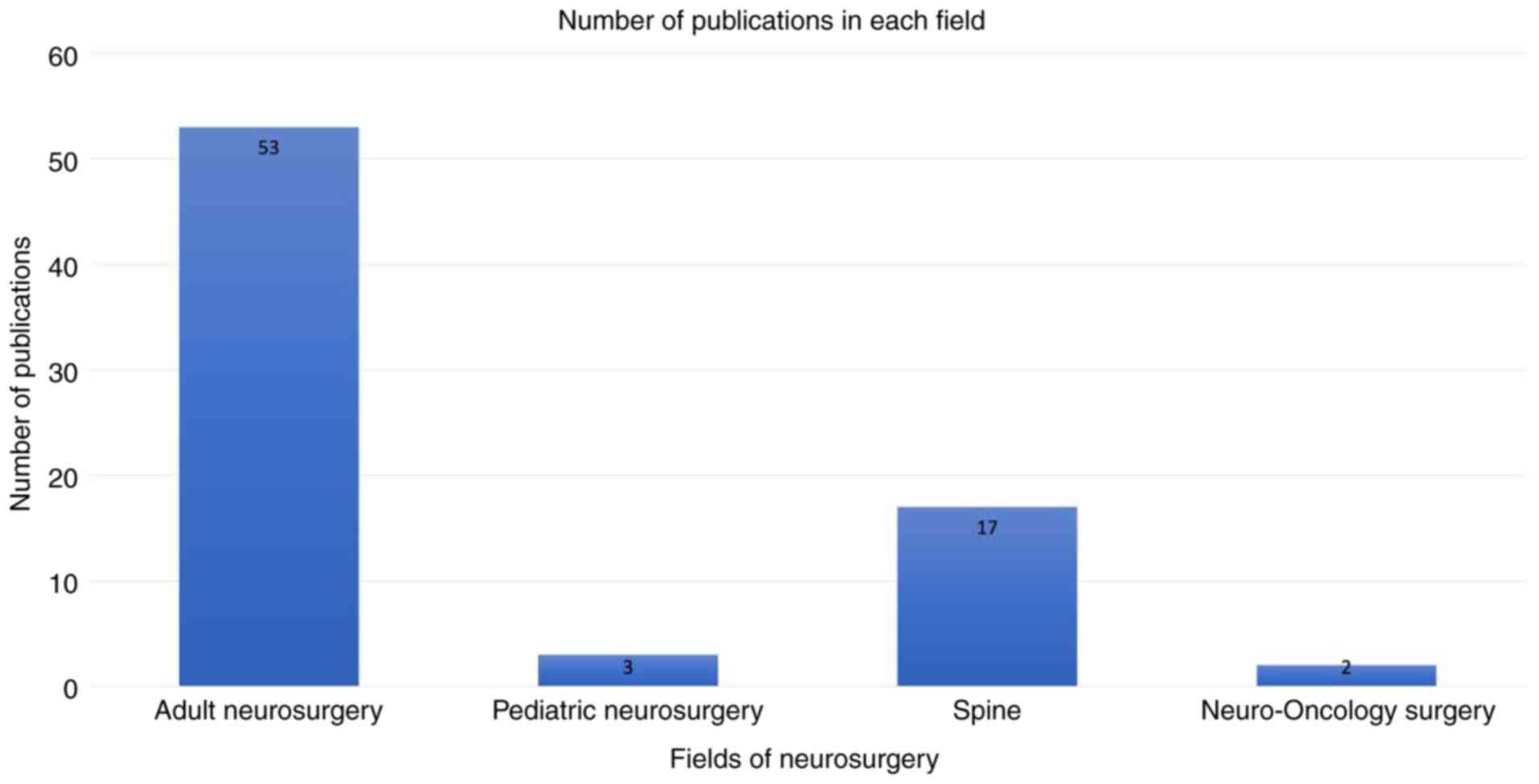 |
Figure 2
Bar chart depicting the number of quality improvement publications in four main fields in neurosurgery.
|
 |
Table I
Summary of all relevant findings in the included quality improvement studies.
|
Table I
Summary of all relevant findings in the included quality improvement studies.
| Article no. |
First author |
Year of publication |
Country |
Field of neurosurgery |
Targeted patients |
No. of patients |
QI intervention |
Research design |
(Refs.) |
| 1 |
Ziewacz |
2015 |
USA |
Spine surgery |
All patients undergoing neurosurgery |
Unspecified |
Education |
Correlational study |
(10) |
| 2 |
Anderson |
2016 |
USA |
Spine surgery |
Patients underwent spine surgery |
Data on HAI from over 1545 hospital facilities with unspecified number of patients |
Infection prevention and sterilization |
Systematic review |
(11) |
| 3 |
Lindbäck |
2017 |
Sweden |
Spine surgery |
Patients with degenerative lumbar spine disorder |
197 |
Protocol and audit |
Randomized clinical trial |
(12) |
| 4 |
McLaughlin |
2015 |
USA |
Adult neurosurgery |
All neurosurgical procedures performed in the main operating room or the outpatient surgery center at the Ronald Reagan UCLA Medical Center and UCLA Santa Monica Medical Center from July 2008 to December 2012 were considered for this study except interventional radiology and stereotactic radiosurgery procedures |
6,912 |
Incidence reporting |
Systematic review |
(13) |
| 5 |
Robertson |
2018 |
USA |
Adult neurosurgery |
Patients undergoing elective cranial or spinal neurosurgery |
416 |
Patient compliance and safety |
Randomized clinical trial |
(14) |
| 6 |
Pendola |
2022 |
USA |
Pediatric neurosurgery |
Pediatric neurosurgery |
129 |
Data analysis and review |
Cross-sectional study |
(15) |
| 7 |
Ashraf |
2021 |
Pakistan |
Adult neurosurgery |
Elective cases of both cranial and spinal neurosurgical diseases. |
100 |
Protocol and audit |
Audit study |
(16) |
| 8 |
Isaacs |
2022 |
Canada |
Adult neurosurgery |
Adult patients (aged ≥18 years) undergoing VP shunt surgery |
244 |
Infection prevention and sterilization |
Audit study |
(17) |
| 9 |
Bekelis |
2015 |
USA |
Adult neurosurgery |
Unspecified |
Unspecified |
Data analysis and review |
Prospective cohort study |
(18) |
| 10 |
Zuckerman |
2012 |
USA |
Adult neurosurgery |
All patients undergoing neurosurgical procedures. |
Unspecified |
Checklist |
Systematic review |
(19) |
| 11 |
Ali |
2021 |
USA |
Adult neurosurgery |
neurosurgical patients at an urban, level I trauma, academic teaching hospital. |
Unspecified |
Education |
Prospective cohort study |
(20) |
| 12 |
Asher |
2015 |
USA |
Adult neurosurgery |
Unspecified |
Unspecified |
Data analysis and review |
Prospective cohort study |
(21) |
| 13 |
Kerezoudis |
2021 |
USA |
Adult neurosurgery |
National Surgical Quality Improvement Program abstracted neurosurgical cases |
317 |
Infection prevention and sterilization |
Systematic review |
(22) |
| 14 |
Sisler |
2017 |
USA |
Adult neurosurgery |
Patients 18 years of age or older who indicated current tobacco use (that is, in the 30 days prior to admission) were admitted to the inpatient neurosurgical service |
526: 189 from the period between July 1, 2014, and December 31, 2014 taken as control and 337 from period between January 1, 2015 to December 31, 2015 taken as the intervention group |
Protocol and audit |
Randomized clinical trial |
(23) |
| 15 |
Deyo |
2009 |
USA |
Spine surgery |
Patients underwent spine surgery |
Unspecified |
Data analysis and review |
Prospective cohort studies |
(24) |
| 16 |
Ruiz Colón |
2023 |
USA |
Pediatric neurosurgery |
Pediatric patients |
Unspecified |
Data analysis and review |
Systematic review |
(25) |
| 17 |
Yang |
2015 |
USA |
Adult neurosurgery |
Unspecified |
Unspecified |
Data analysis and review |
Prospective cohort studies |
(26) |
| 18 |
Stumpo |
2021 |
USA |
Adult neurosurgery-cranial |
Unspecified |
Unspecified |
ERAS |
Systematic review |
(27) |
| 19 |
Wang |
2020 |
USA |
Adult neurosurgery |
Unspecified |
Unspecified |
Data analysis and review |
Case report |
(28) |
| 20 |
Meyrat |
2021 |
USA |
Adult neurosurgery |
Ambulatory and hospital cases of neurosurgery |
2,646: 2,270 were ambulatory dataset and 376 were a hospital dataset |
Patient compliance and safety |
Correlational study |
(29) |
| 21 |
Tanenbaum |
2016 |
USA |
Spine surgery |
All adult patients aged 18 years and older included in the nation-wide inpatient sample (NIS) that underwent lumbar fusion from 1998-2011 |
53,9172 |
Patient compliance and safety |
Prospective cohort study |
(30) |
| 22 |
Groman |
2015 |
USA |
Adult neurosurgery |
Unspecified |
Unspecified |
Data analysis and review |
Prospective cohort studies |
(31) |
| 23 |
Hall |
2019 |
UK |
Adult neurosurgery |
Patients returning from the operating department to the neuro-surgical ward |
100 |
Checklist |
Randomized clinical trial |
(32) |
| 24 |
McLaughlin |
2014 |
USA |
Adult neurosurgery |
All patients undergoing neurosurgery |
Unspecified |
Protocol and audit |
Systematic review |
(33) |
| 25 |
Shi |
2023 |
USA |
Pediatric neurosurgery |
Children undergoing spinal surgery |
Unspecified |
Data analysis and review |
Randomized clinical trial |
(34) |
| 26 |
Oszvald |
2012 |
Germany |
Adult neurosurgery |
All patients undergoing neurosurgery |
12,390 |
Checklist |
Randomized clinical trial |
(35) |
| 27 |
Sarnthein |
2016 |
Switzerland |
Adult neurosurgery-cranial |
All patients undergoing neurosurgery |
2,880 |
Protocol and audit |
Correlational study |
(36) |
| 28 |
Zuckerman |
2015 |
North America |
Adult neurosurgery |
All patients undergoing neurosurgery |
Unspecified |
Checklist |
Systematic review |
(37) |
| 29 |
Ber |
2021 |
USA |
Adult neurosurgery |
All patients undergoing neurosurgery |
1,530 |
Technology |
Randomized clinical trial |
(38) |
| 30 |
Liu |
2022 |
China |
Adult neurosurgery |
Patients >65 years of age undergoing neurosurgeries |
Unspecified |
ERAS |
Systematic review |
(39) |
| 31 |
Benjamin |
2022 |
USA |
Adult neurosurgery |
Patients undergoing endoscopic endonasal resection of pituitary adenomas |
171 |
Protocol and audit |
Case-control study |
(40) |
| 32 |
Norris |
2023 |
USA |
Spine surgery |
Patients ≥18 years of age meeting one of the following high-risk criteria: 8 + levels fused, osteoporosis with 4 + levels fused, three column osteotomy, anterior revision of the same lumbar level, or planned significant correction for severe myelopathy, scoliosis (>75˚), or kyphosis (>75˚) |
263 |
Data analysis and review |
Prospective cohort study |
(41) |
| 33 |
Debono |
2021 |
|
Spine surgery |
Patients undergoing lumbar spinal fusion |
Unspecified |
ERAS |
Systematic review |
(42) |
| 34 |
Elsarrag |
2019 |
USA |
Spine surgery |
Pediatric patients with spinal deformities |
132 |
ERAS |
Systematic review |
(43) |
| 35 |
Dietz |
2019 |
India |
Spine surgery |
Patients with brain tumors |
500 |
ERAS |
Systematic review |
(44) |
| 36 |
Elayat |
2021 |
India |
Adult neurosurgery |
Adult patients scheduled for elective supratentorial intracranial tumor excision |
70 |
ERAS |
Randomized clinical trial |
(45) |
| 37 |
Koucheki |
2021 |
Canada |
Spine surgery |
Individuals with adolescent idiopathic scoliosis |
2,456 |
ERAS |
Systematic review |
(46) |
| 38 |
Kerolus |
2021 |
USA |
Spine surgery |
Patients undergoing an elective single-level MIS TLIF for degenerative changes at a single institution |
299 |
ERAS |
Randomized clinical trial |
(47) |
| 39 |
Wang |
2022 |
China |
Adult neurosurgery |
Patients who underwent elective craniotomy between January 2019 and June 2020. |
151 |
ERAS |
Randomized clinical trial |
(48) |
| 40 |
Greisman |
2022 |
USA |
Neuro-oncology |
Patients undergoing cranial tumor resection. |
Unspecified |
ERAS |
Systematic review |
(49) |
| 41 |
Suresh |
2021 |
India |
Adult neurosurgery |
Undergoing elective neurosurgical procedures, specifically 131 cases of craniotomy and 69 cases of spine surgery |
200 |
Checklist |
Cross-sectional study |
(50) |
| 42 |
Westman |
2020 |
Finland |
Adult neurosurgery |
Patients undergoing neurosurgical procedures. |
Unspecified |
Checklist |
Systematic review |
(2) |
| 43 |
Lepänluoma |
2014 |
Finland |
Adult neurosurgery |
Neurosurgical patients |
150 |
Checklist |
Cross-sectional study |
(51) |
| 44 |
Soriano Sánchez |
2019 |
Mexico |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Checklist |
Systematic review |
(52) |
| 45 |
Lau. |
2012 |
USA |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Checklist |
Prospective cohort study |
(53) |
| 46 |
Enchev |
2015 |
Bulgaria |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Checklist |
Systematic review |
(54) |
| 47 |
Silva-Freitas |
2012 |
Spain |
Adult neurosurgery |
Neurosurgical patients |
400 |
Checklist |
Pre/post-intervention study |
(55) |
| 48 |
Schaffzin |
2015 |
USA |
Spine surgery |
Pediatric patients undergoing cardio-thoracic, neurosurgical shunt, and spinal fusion surgeries |
Unspecified |
Infection prevention and sterilization |
Cross-sectional study |
(56) |
| 49 |
Pauli |
2017 |
Brazil |
Adult neurosurgery |
Patients with mesial temporal lobe epilepsy undergoing anterior temporal lobectomy |
50 |
ERAS |
Systematic review |
(57) |
| 50 |
Tian |
2022 |
China |
Adult neurosurgery |
Neurosurgical patients |
24,137 |
Infection prevention and sterilization |
Systematic review |
(58) |
| 51 |
Wang |
2020 |
China |
Adult neurosurgery |
Patients admitted to the neurosurgery intensive care unit between January 2017 and February 2018, in Capital Medical University, Beijing, China |
310 |
Prediction model |
Systematic review |
(59) |
| 52 |
Annette |
2005 |
Sweden |
Adult neurosurgery |
Neurosurgical intensive care unit patients |
Unspecified |
Education |
Cross-sectional study |
(60) |
| 53 |
Krushelnytskyy |
2022 |
USA |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Protocol and audit |
Audit study |
(61) |
| 54 |
Kassicieh |
2022 |
USA |
Adult neurosurgery-cranial |
Patients with inter-hospital transfer status |
47,736 |
NA |
Prospective cohort study |
(62) |
| 55 |
Witiw |
2015 |
USA |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Infection prevention and sterilization |
Randomized clinical trial |
(5) |
| 56 |
Neal |
2021 |
USA |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Framework |
Audit study |
(4) |
| 57 |
Rotter |
2022 |
USA |
Adult neurosurgery |
Patients requiring external ventricular drain (EVD) or intracranial pressure (ICP) monitor placement |
Unspecified |
Protocol and audit |
Audit study |
(63) |
| 58 |
Schipmann |
2016 |
Germany |
Adult neurosurgery-cranial |
Patients undergoing cranial neurosurgery |
70 cases with surgical site infections and 185 matched controls |
Infection prevention and sterilization |
Case-control studies |
(64) |
| 59 |
Rubiano |
2012 |
USA |
Adult neurosurgery-cranial |
Neurotrauma patients in low- and middle-income countries |
Unspecified |
Data analysis and review |
Systematic review |
(65) |
| 60 |
Fischer |
2015 |
USA |
Neuro-oncology |
Pediatric patients with brain tumors |
Unspecified |
Data analysis and review |
Systematic review |
(66) |
| 61 |
Bernstein |
2004 |
Canada |
Adult neurosurgery |
Patients undergoing novel neurosurgical procedures |
Unspecified |
Framework |
Systematic review |
(67) |
| 62 |
Leming-Lee |
2019 |
USA |
Adult neurosurgery |
Neurosurgical patients undergoing craniotomy procedures |
Unspecified |
Infection prevention and sterilization |
Pre/post-intervention studies |
(68) |
| 63 |
Hover |
2013 |
USA |
Adult neurosurgery |
Patients undergoing elective neurosurgical procedures |
Unspecified |
Infection prevention and sterilization |
Pre/post-intervention studies |
(69) |
| 64 |
Mathews |
2015 |
USA |
Adult neurosurgery |
Elective neurosurgical patients |
2,328 |
Protocol and audit |
Case report |
(70) |
| 65 |
Rupich |
2018 |
USA |
Spine surgery |
Postoperative neuro-surgical spine patients |
Unspecified |
ERAS |
Case-control study |
(71) |
| 66 |
Rozman |
2020 |
USA |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Protocol and audit |
Pre/post-intervention study |
(72) |
| 67 |
Farrokhi |
2013 |
USA |
Adult neurosurgery |
Patients undergoing minimally invasive spine surgery |
Unspecified |
Protocol and audit |
Audit study |
(73) |
| 68 |
Xu |
2013 |
China |
Adult neurosurgery |
Critically ill patients in a neurosurgical intensive care unit |
Unspecified |
Protocol and audit |
Audit study |
(74) |
| 69 |
Chang |
2021 |
USA |
Adult neurosurgery-cranial |
Patients requiring external ventricular drain (EVD) placement in the emergency department |
38 (20 during protocol initia tion and 18 pre-protocol) |
Patient compliance and safety |
Pre/post-intervention study |
(75) |
| 70 |
Ezeamuzie |
2019 |
USA |
Adult neurosurgery |
Patients undergoing complex surgical procedures with increased operative time) |
212 |
Protocol and audit |
Prospective case-control study |
(76) |
| 71 |
Kantelhardt |
2011 |
Germany |
Adult neurosurgery |
Neurosurgical patients |
Unspecified |
Incidence reporting |
Pre/post-intervention studies |
(77) |
| 72 |
Ryan |
2014 |
USA |
Spine surgery |
Pediatric patients undergoing complex spine surgery |
267 |
Infection prevention and sterilization |
Pre/post-intervention study |
(78) |
| 73 |
Kantelhardt |
2016 |
Germany |
Spine surgery |
Patients undergoing spinal surgery |
149 |
Checklist |
Pre/post-intervention study |
(79) |
| 74 |
Licina |
2021 |
Australia |
Spine surgery |
Patients undergoing spinal surgery |
Unspecified |
ERAS |
Systematic review |
(80) |
| 75 |
Young |
2020 |
USA |
Spine surgery |
Patients undergoing elective spine procedures |
1,000 |
Protocol and audit |
Pre/post-intervention study |
(81) |
 |
Table II
Quality improvement in neurosurgeries and sub-subspecialties.
|
Table II
Quality improvement in neurosurgeries and sub-subspecialties.
| Targeted patients |
No. of patients |
Percentage |
(Refs.) |
| Spinal only |
540,955 |
87.07 |
(10-12,24,30,41-44,46,47,56,71,78-81) |
| Unspecified |
79,029 |
12.72 |
(15,25,34,49,66) |
| Cranial + spinal |
673 |
0.11 |
(13,14,16-23,25,26,28,29,31-33,35,37-40,45,48,50-55,57-4,5,61,63,67-70,72-74,76,77) |
| Cranial only |
636 |
0.1 |
(27,36,62,64,65,75) |
Different interventions were used to improve QI and enhance care in neurosurgery. Implementing new protocols and audits was the most common intervention with 14 articles (18.67%) (12,16,23,33,36,40,61,63,70,72-74,76,81). This was followed by enhanced recovery after surgery (ERAS) with 13 articles (17.33%) (27,39,42,49,57,71,80), data analysis of databases, registries, and literature with 12 articles (16%) (15,18,21,24-26,28,31,34,41,65,66), new or modified checklists implementation with 11 articles (14.67%) (2,19,32,35,37,50-52,54,55,79), and utilizing new sterilization devices or protocols with 10 articles (13.3%) (5,11,17,22,56,58,64,68,69,78). Less frequently addressed interventions were utilizing new technology, using a prediction model, improving incident reporting, increasing patient compliance, and educating the neurosurgical staff (10,13,14,20,29,30,38,53,59,60,75,77) (Fig. 3).
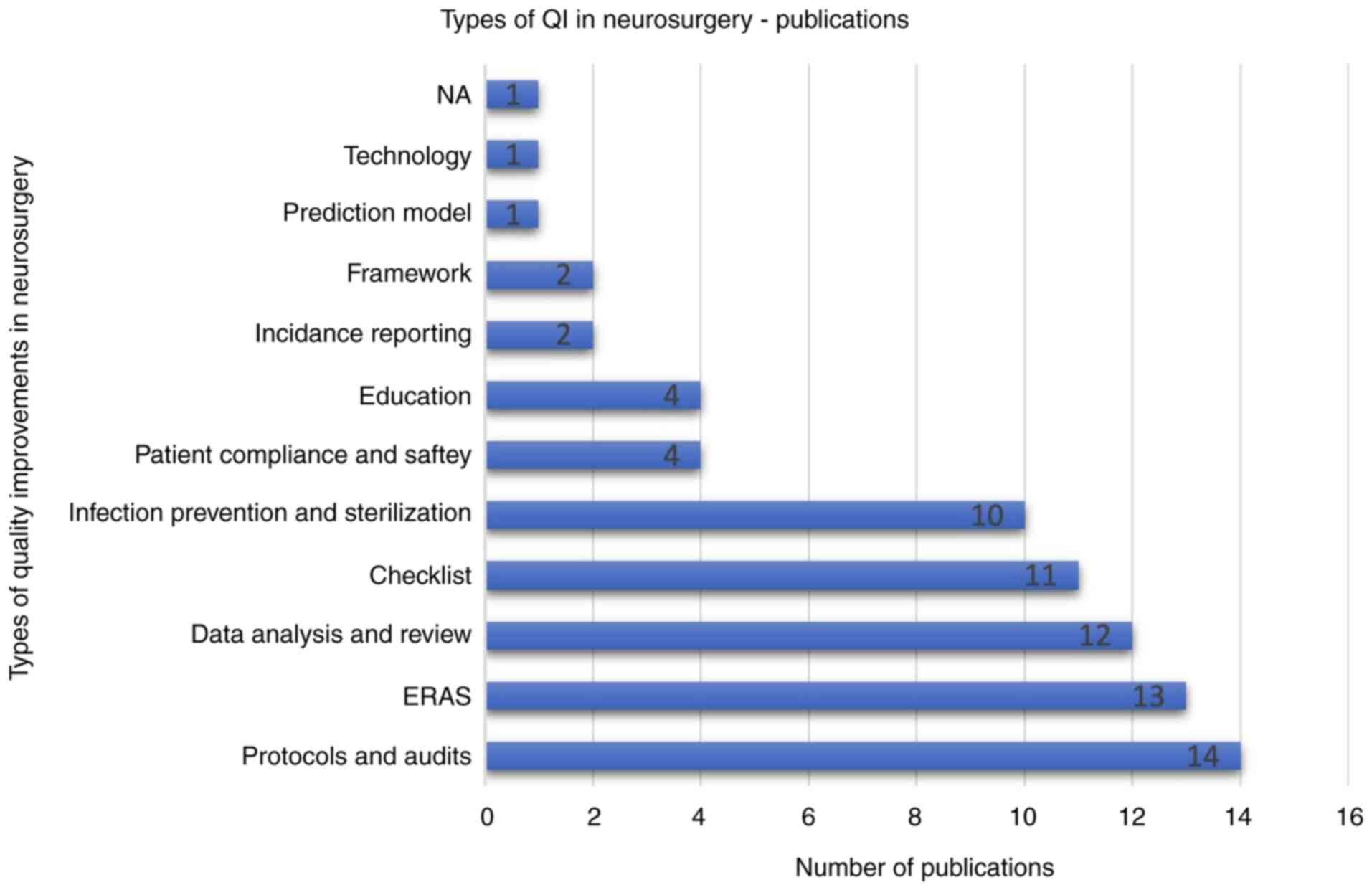 |
Figure 3
Bar chart depicting the different interventions used to provide quality improvement in neurosurgical care.
|
The study design varied within the 75 publications and covered the whole research design pyramid from systematic reviews, the most authentic and strongest research design, to case studies, the least authentic and weakest research design. The predominant design was systematic review studies with 24 articles (32%) (2,11,13,19,22,25,27,33,37,39,42,43,44,46,49,52,54,57-59,65-67,80), followed by randomized clinical trials with 11 articles (14.67%) (5,12,14,23,32,34,35,38,45,47,48), and prospective cohort studies with 10 articles (13.33%) (18,20,21,24,26,30,31,41,53,62). The least research designs used were prospective case-control studies with only one article (1.33%) (77), case reports with two articles (2.67%) (28,37), and correlation (10,29,36) and retrospective (40,64,71) studies with three articles (4%) each. Other types of studies, such as audit studies (4,16,17,61,63,73,74) and cross-sectional studies (15,50,51,56,60) were in between (Table III).
 |
Table III
Research design of the selected studies.
|
Table III
Research design of the selected studies.
| Types of studies |
No. of studies |
Percentage |
(Refs.) |
| Systematic review studies |
24 |
32.00 |
(2,11,13,19,22,25,27,33,37,39,42,43,44,46,49,52,54,57-59,65,69,67,80) |
| Randomized clinical trials |
11 |
14.67 |
(12,14,23,32,34,35,38,45,47,48,63) |
| Prospective cohort studies |
10 |
13.33 |
(18,20,21,24,26,30,31,41,53,62) |
| Pre/post-intervention studies |
9 |
12.00 |
(55,68,69,72,75,77,78,79,81) |
| Audit studies |
7 |
9.33 |
(4,16,17,61,63,73,74) |
| Cross-sectional studies |
5 |
6.67 |
(15,50,52,56,60) |
| Case-control studies |
3 |
4.00 |
(40,64,71) |
| Correlation studies |
3 |
4.00 |
(10,29,36) |
| Case reports |
2 |
2.67 |
(28,37) |
| Prospective case-control studies |
1 |
1.33 |
(76) |
The articles spanned through a period of 20 years from 2004 to 2023, with gaps of no publications in 2006-2008 and 2010. Notably, 81% of the publications were from 2012 to 2023 (2,4,5,10-23,25-59,61-66,68,81). The year 2021 had the highest number of publications with 14 articles (18.66%) (4,16,20,22,27,29,38,42,45-47,50,75,80), followed by 2015 with 12 articles (16%) (5,10,13,18,21,26,31,37,54,56,66,70), and 2022 with 10 articles (13.3%) (15,17,39,40,48,49,58,61-63). Conversely, 2004, 2005, 2009 and 2011 had the fewest publications, with only one article each (24,60,67,77), followed by 2018 with two articles each (14,71). The average number of articles per year between 2004 and 2023 was 3.75 (Fig. 4). Geographically, the distribution of publications was also uneven. The majority originated from the USA (46 articles) (4,5,10,11,13-15,18-31,33,34,38,40,41,43,47,49,53,56,61-63,65,66,68-73,75,76,78,81), and Germany and China with four and five articles, respectively (35,39,48,58,59,64,74,77,79). Contributions from other countries were fewer (Fig. 5).
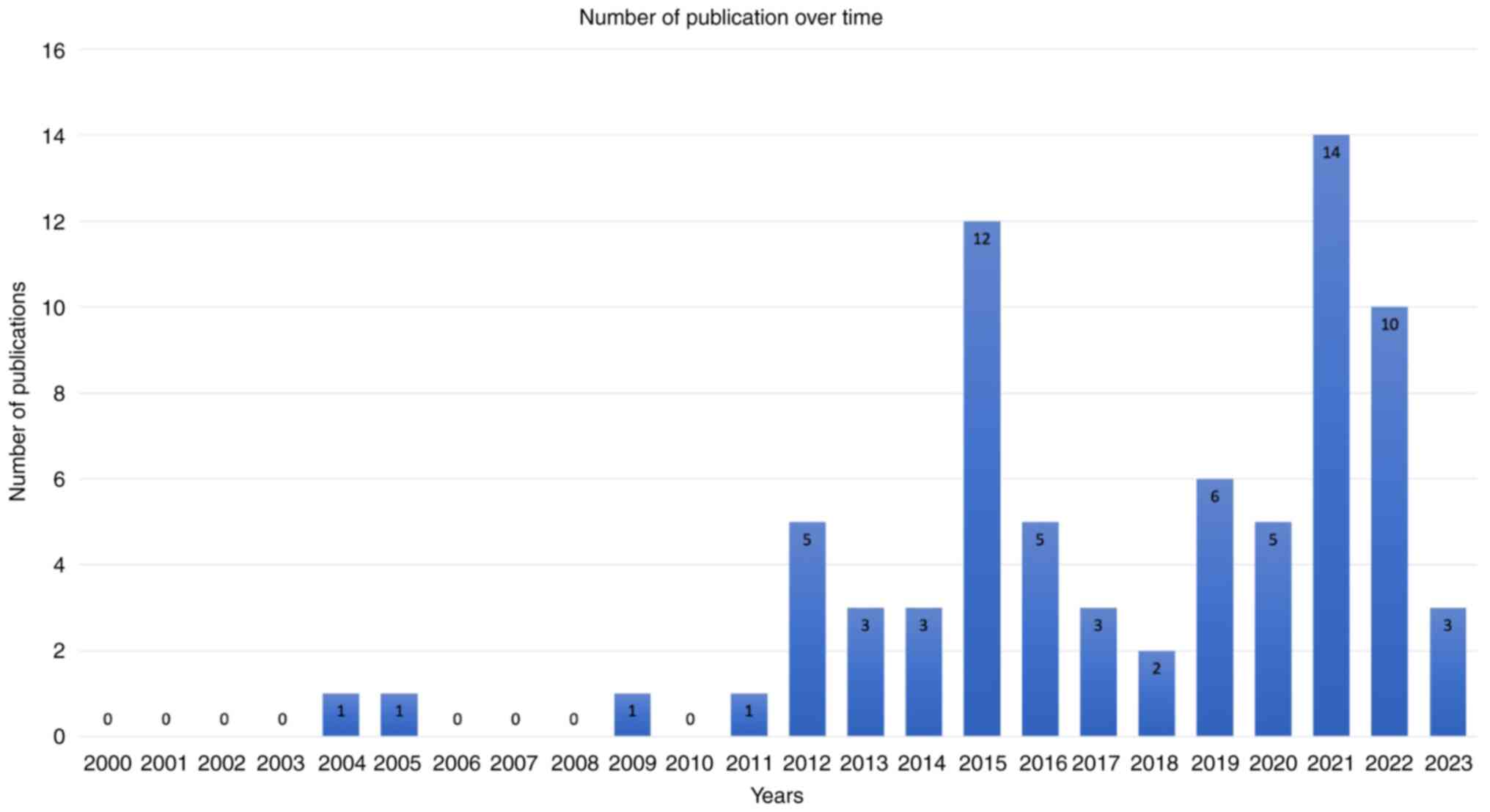 |
Figure 4
Bar chart depicting the number of publications in each year from 2000 to 2023.
|
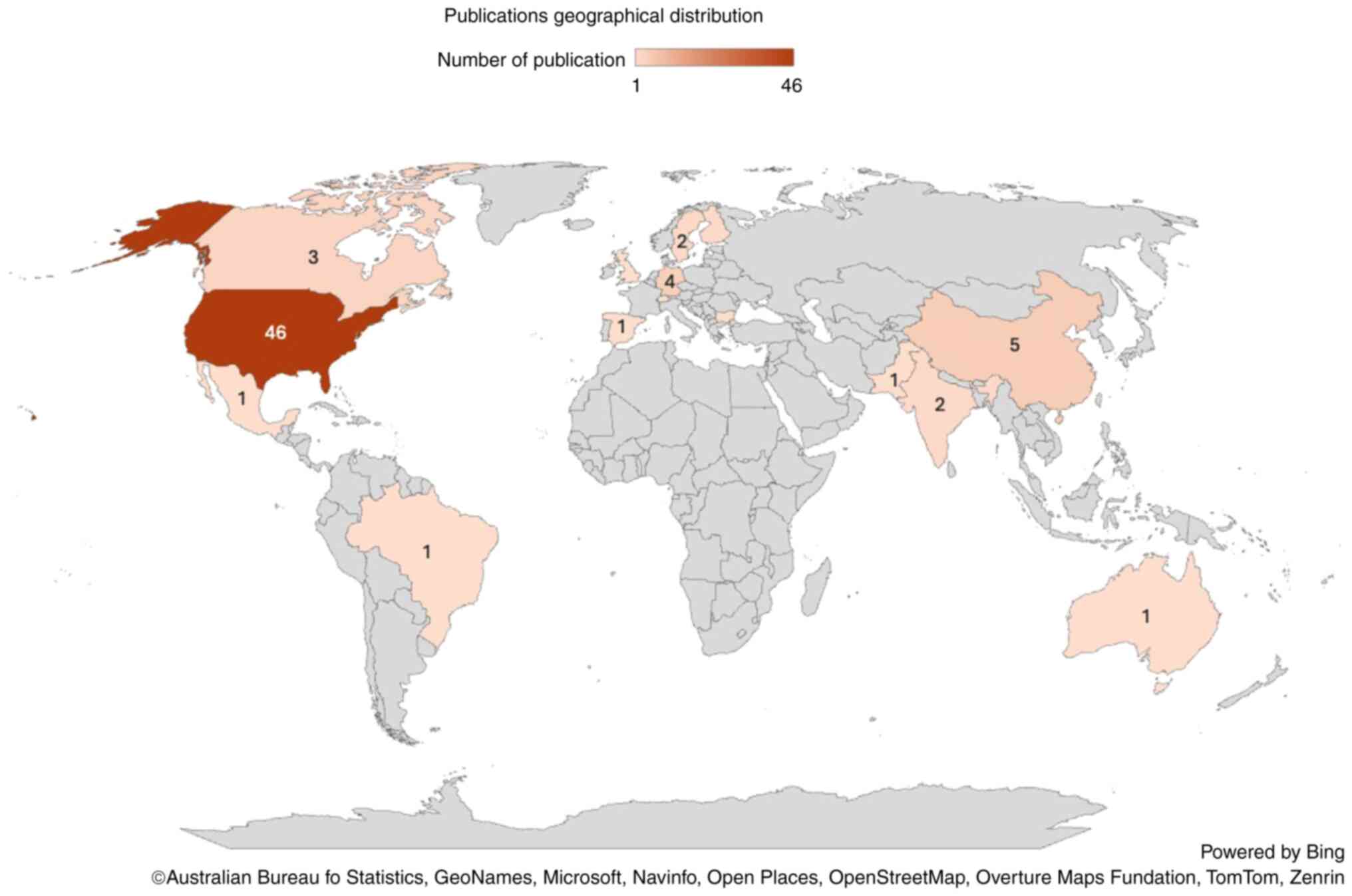 |
Figure 5
World map depicting the countries where quality improvement studies were published and their numbers.
|
Discussion
QI in healthcare is crucial for various reasons: For enhancing the outcomes of patients, professional development, understanding healthcare challenges at local and national levels, and improving overall system performance. Given the inherent complexities and critical nature of neurosurgery, QI is exceptionally essential, rendering research in this area fundamental (26).
The results of the present study provide key insight into the QI initiatives within the field of neurosurgery. There is an uneven distribution of publications across the main subspecialties of neurosurgery: Adults, pediatrics, spine, cranial and neuro-oncology. This is similar to the findings of other studies and is due to the higher volume of procedures in one field more than the other and/or higher incidence of complications. The findings of the present study, similar to those of other research, also demonstrated a marked disparity in the distribution of targeted patients across the different fields of neurosurgery being more focused on spinal-only (82). The reason for this may be due to low morbidity rates and high efficacy in sustaining therapeutic outcomes of spinal surgery. As a result, this leads to an unintentional bias in the effort of QI research aimed to improve these outcomes and reduce post-operative complications (82). However, the limited attention given to other subspecialties, such as cranial procedures, is concerning. This imbalance is troubling as it may lead to disparities in the quality of care and patient outcomes across different neurosurgical fields. Future QI initiatives should aim to achieve a more equitable distribution of focus across all subspecialties to ensure comprehensive improvements in neurosurgical care (83).
The most common QI interventions are implementing new protocols, audits, ERAS, and data analysis from databases and registries. As was expected, it was found that these QI interventions reflected marked effectiveness in reducing operative complications and improving outcomes (84). However, other implementations may have a crucial impact on neurosurgical care and outcomes that have less QI research focus. For example, improving incident reporting, prediction models and new technologies. It may be beneficial for future studies to explore the impact of the less common interventions and to determine their impact across neurosurgical settings (6).
The findings presented herein highlight several key areas for future research and development in QI for neurosurgery specifically and healthcare in general. There is a need for more balanced attention across all neurosurgical fields particularly in areas, such as pediatrics and neuro-oncology. Expanding the diversity in QI interventions and exploring the efficacy of less common approaches will be crucial for developing comprehensive strategies, techniques and protocols that address the challenges of neurosurgical care.
The present study had some limitations, which should be mentioned. One of the notable limitations encountered during the study was the inability to access several articles due to paywalls. Despite efforts to obtain these publications, seven articles could not be accessed and were therefore excluded from the review. This limitation highlights a common challenge in academic research where financial barriers restrict access to potentially valuable information. Additionally, the scarcity of articles directly addressing the specific aims of this study posed another limitation. The targeted nature of the key words and the niche focus on neurosurgical quality control and improvement meant that there were relatively few articles available that fit the criteria precisely. As a result, it is possible that some relevant articles were not detected during the search process, potentially leading to an incomplete collection of data. This limitation underscores the importance of continued research and publication in this specialized area to build a more robust body of literature for future reviews.
In conclusion, QI studies enhanced care delivery for patients admitted to neurosurgery departments. The findings of the present study demonstrated that these studies were mainly focused on adult neurosurgery and primarily targeted patients who required spinal surgery. Furthermore, the most commonly employed methods to improve the quality of care include the implementation of new protocols, ERAS pathways, data analysis and new or modified checklists. Further research is required to bridge the gap by addressing QI initiatives in cranial surgery and evaluating the effectiveness of less-used modalities, such as new technologies and predictive models.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The data generated in the present study may be requested from the corresponding author.
Authors' contributions
TAS and MMM were involved in the drafting of the manuscript or revising it critically for important intellectual content. TAS, MMM, AMA, NMA, and MA made substantial contributions to the conception or design of the study. MMM, AMA, NMA and MA were involved in the writing of the manuscript and in the literature review. All authors have read and approved the final version of the manuscript.
Ethics approval and consent to participate
Not Applicable.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
References
|
1
|
Backhouse A and Ogunlayi F: Quality improvement into practice. BMJ. 368(m865)2020.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Westman M, Takala R, Rahi M and Ikonen TS: The need for surgical safety checklists in neurosurgery now and in the future-A systematic review. World Neurosurg. 134:614–628.e3. 2020.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Shirley E: Advancements in neurosurgery and exploring innovations techniques. Perspective. 14(451)2024.
|
|
4
|
Neal MT, Richards AE, Curley KL and Lyons MK: Launching a quality improvement project in neurosurgery: How to get started. Interdiscip Neurosurg. 25(101206)2021.
|
|
5
|
Witiw CD, Nathan V and Bernstein M: Economics, innovation, and quality improvement in neurosurgery. Neurosurg Clin N Am. 26:197–205. 2015.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Hughes RG: Tools and strategies for quality improvement and patient safety. Patient Safety and Quality, 2008.
|
|
7
|
Gettelfinger JD, Paulk PB and Schmalbach CE: Patient safety and quality improvement in otolaryngology-head and neck surgery: A systematic review. Laryngoscope. 131:33–40. 2021.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Grue B, McGuire C, Hong P and Bezuhly M: Patient safety and quality improvement Initiatives in cleft lip and palate Surgery: A systematic review. J Craniofac Surg. 34:979–986. 2023.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Buia A, Stockhausen F and Hanisch E: Laparoscopic surgery: A qualified systematic review. World J Methodol. 5:238–254. 2015.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Ziewacz JE, McGirt MJ and Chewning SJ Jr: Adverse events in neurosurgery and their relationship to quality improvement. Neurosurg Clin N Am. 26:157–165.vii. 2015.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Anderson PA, Savage JW, Vaccaro AR, Radcliff K, Arnold PM, Lawrence BD and Shamji MF: Prevention of surgical site infection in spine surgery. Neurosurgery. 80(3S):S114–S123. 2017.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Lindbäck Y, Tropp H, Enthoven P, Abbott A and Öberg B: PREPARE: Presurgery physiotherapy for patients with degenerative lumbar spine disorder: A randomized controlled trial. Spine J. 18:1347–1355. 2018.PubMed/NCBI View Article : Google Scholar
|
|
13
|
McLaughlin N, Jin P and Martin NA: Assessing early unplanned reoperations in neurosurgery: Opportunities for quality improvement. J Neurosurg. 123:198–205. 2015.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Robertson FC, Logsdon JL, Dasenbrock HH, Yan SC, Raftery SM, Smith TR and Gormley WB: Transitional care services: A quality and safety process improvement program in neurosurgery. J Neurosurg. 128:1570–1577. 2018.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Pendola G, Koutsouras GW, Piatt J, Kaufman BA, Sandoval-Garcia C and Drapeau AI: Current state and future direction of quality improvement in pediatric neurosurgery: A survey of pediatric neurosurgeons. J Neurosurg Pediatr. 31:186–191. 2022.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Ashraf M, Hussain SS, Kamboh UA, Mehboob M, Shahid S and Ashraf N: Improvement in the quality of patient notes: A report of a closed loop audit quality improvement project at a neurosurgical department in Pakistan. J Pak Med Assoc. 71:1515–1520. 2021.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Isaacs AM, Ball CG, Sader N, Muram S, Ben-Israel D, Urbaneja G, Dronyk J, Holubkov R and Hamilton MG: Reducing the risks of proximal and distal shunt failure in adult hydrocephalus: A shunt outcomes quality improvement study. J Neurosurg. 136:877–886. 2021.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Bekelis K, McGirt MJ, Parker SL, Holland CM, Davies J, Devin CJ, Atkins T, Knightly J, Groman R, Zyung I and Asher AL: The present and future of quality measures and public reporting in neurosurgery. Neurosurg Focus. 39(E3)2015.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Zuckerman SL, Green CS, Carr KR, Dewan MC, Morone PJ and Mocco J: Neurosurgical checklists: A review. Neurosurg Focus. 33(E2)2012.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Ali R, Syed S, Sastry RA, Abdulrazeq H, Shao B, Roye GD, Doberstein CE, Oyelese A, Niu T, Gokaslan ZL and Telfeian A: Toward more accurate documentation in neurosurgical care. Neurosurg Focus. 51(E11)2021.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Asher AL, Parker SL, Rolston JD, Selden NR and McGirt MJ: Using clinical registries to improve the quality of neurosurgical care. Neurosurg Clin N Am. 26:253–263.ix-x. 2015.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Kerezoudis P, Kelley PC, Watts CR, Heiderscheit CJ and Roskos MC: Using a data-driven improvement methodology to decrease surgical site infections in a community neurosurgery practice: Optimizing preoperative screening and perioperative antibiotics. World Neurosurg. 149:e989–e1000. 2021.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Sisler L, Omofoye O, Paci K, Hadar E, Goldstein AO and Ripley-Moffitt C: Using lean quality improvement tools to increase delivery of evidence-based tobacco use treatment in hospitalized neurosurgical patients. Jt Comm J Qual Patient Saf. 43:633–641. 2017.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Deyo RA and Mirza SK: The case for restraint in spinal surgery: Does quality management have a role to play? Eur Spine J 18 Suppl. 3 (Suppl 3):S331–S337. 2009.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Ruiz Colón GD, Wu A, Ratliff JK and Prolo LM: Quality and patient safety research in pediatric neurosurgery: A review. Childs Nerv Syst. 39:1147–1158. 2023.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Yang I, Ung N, Nagasawa DT, Pelargos P, Choy W, Chung LK, Thill K, Martin NA, Afsar-Manesh N and Voth B: Recent advances in the patient safety and quality initiatives movement: Implications for neurosurgery. Neurosurg Clin N Am. 26:301–315.xi. 2015.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Stumpo V, Staartjes VE, Quddusi A, Corniola MV, Tessitore E, Schröder ML, Anderer EG, Stienen MN, Serra C and Regli L: Enhanced recovery after surgery strategies for elective craniotomy: A systematic review. J Neurosurg. 135:1857–1881. 2021.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Wang MC, Boop FA, Kondziolka D, Resnick DK, Kalkanis SN, Koehnen E, Selden NR, Heilman CB, Valadka AB, Cockroft KM, et al: Continuous improvement in patient safety and quality in neurological surgery: The American board of neurological surgery in the past, present, and future. J Neurosurg. 135:637–643. 2020.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Meyrat R, Vivian E, Shah J, Sridhar A, Hurst BB, Shoup C, Graham RB, Katzen S, Mitchell B, Oh M and Patel NH: Investigating the relationship between ambulatory and hospital patient experience scores in a neurosurgery practice. Healthcare (Basel). 9(1153)2021.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Tanenbaum JE, Alentado VJ, Miller JA, Lubelski D, Benzel EC and Mroz TE: Association between insurance status and patient safety in the lumbar spine fusion population. Spine J. 17:338–345. 2016.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Groman R: The relationship between national health care policies and quality improvement in neurosurgery. Neurosurg Clin N Am. 26:167–175.vii-viii. 2015.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Hall AJ, Toner NS and Bhatt PM: The introduction of a neurosurgical postoperative checklist improved quality of care and patient safety. Br J Neurosurg. 33:495–499. 2019.PubMed/NCBI View Article : Google Scholar
|
|
33
|
McLaughlin N, Rodstein J, Burke MA and Martin NA: Demystifying process mapping: A key step in neurosurgical quality improvement initiatives. Neurosurgery. 75:99–109. 2014.PubMed/NCBI View Article : Google Scholar
|
|
34
|
Shi HH, Chen S, Propester L, Valenzuela J, Gernsback J, Desai VR, Balsara K, Zieles K and Jea A: Influence of the living Pareto chart and data transparency on patient outcomes in neurosurgery. J Neurosurg Pediatr. 31:380–387. 2023.PubMed/NCBI View Article : Google Scholar
|
|
35
|
Oszvald Á, Vatter H, Byhahn C, Seifert V and Güresir E: ‘Team time-out’ and surgical safety-experiences in 12,390 neurosurgical patients. Neurosurg Focus. 33(E6)2012.PubMed/NCBI View Article : Google Scholar
|
|
36
|
Sarnthein J, Stieglitz L, Clavien PA and Regli L: A patient registry to improve patient safety: Recording general neurosurgery complications. PLoS One. 11(e0163154)2016.PubMed/NCBI View Article : Google Scholar
|
|
37
|
Zuckerman SL, Fargen KM and Mocco J: Neurosurgical checklists: A growing need. Neurosurg Clin N Am. 26:219–229. 2015.PubMed/NCBI View Article : Google Scholar
|
|
38
|
Ber R, London D, Senan S, Youssefi Y, Harter DH, Golfinos JG and Pacione D: Perioperative team communication through a mobile app for improving coordination and education in neurosurgery cases. J Neurosurg. 136:1157–1163. 2021.PubMed/NCBI View Article : Google Scholar
|
|
39
|
Liu B, Liu S, Zheng T, Lu D, Chen L, Ma T, Wang Y, Gao G and He S: Neurosurgical enhanced recovery after surgery ERAS for geriatric patients undergoing elective craniotomy: A review. Medicine (Baltimore). 101(e30043)2022.PubMed/NCBI View Article : Google Scholar
|
|
40
|
Benjamin CG, Dastagirzada Y, Bevilacqua J, Kurland DB, Fujita K, Sen C, Golfinos JG, Placantonakis DG, Jafar JJ, Lieberman S, et al: The cost effectiveness of implementation of a postoperative endocrinopathy management protocol after resection of pituitary adenomas. J Neurol Surg B Skull Base. 83:618–625. 2022.PubMed/NCBI View Article : Google Scholar
|
|
41
|
Norris ZA, Zabat MA, Patel H, Mottole NA, Ashayeri K, Balouch E, Maglaras C, Protopsaltis TS, Buckland AJ and Fischer CR: Multidisciplinary conference for complex surgery leads to improved quality and safety. Spine Deform. 11:1001–1008. 2023.PubMed/NCBI View Article : Google Scholar
|
|
42
|
Debono B, Wainwright TW, Wang MY, Sigmundsson FG, Yang MMH, Smid-Nanninga H, Bonnal A, Le Huec JL, Fawcett WJ, Ljungqvist O, et al: Consensus statement for perioperative care in lumbar spinal fusion: Enhanced Recovery After Surgery (ERAS®) Society recommendations. Spine J. 21:729–752. 2021.PubMed/NCBI View Article : Google Scholar
|
|
43
|
Elsarrag M, Soldozy S, Patel P, Norat P, Sokolowski JD, Park MS, Tvrdik P and Kalani MYS: Enhanced recovery after spine surgery: A systematic review. Neurosurg Focus. 46(E3)2019.PubMed/NCBI View Article : Google Scholar
|
|
44
|
Dietz N, Sharma M, Adams S, Alhourani A, Ugiliweneza B, Wang D, Nuño M, Drazin D and Boakye M: Enhanced recovery after surgery (ERAS) for spine surgery: A systematic review. World Neurosurg. 130:415–426. 2019.PubMed/NCBI View Article : Google Scholar
|
|
45
|
Elayat A, Jena SS, Nayak S, Sahu RN and Tripathy S: ‘Enhanced recovery after surgery-ERAS in elective craniotomies-a non-randomized controlled trial’ BMC. Neurol. 21(127)2021.PubMed/NCBI View Article : Google Scholar
|
|
46
|
Koucheki R, Koyle M, Ibrahim GM, Nallet J and Lebel DE: Comparison of interventions and outcomes of enhanced recovery after surgery: A systematic review and meta-analysis of 2456 adolescent idiopathic scoliosis cases. Eur Spine J. 30:3457–3472. 2021.PubMed/NCBI View Article : Google Scholar
|
|
47
|
Kerolus MG, Yerneni K, Witiw CD, Shelton A, Canar WJ, Daily D, Fontes RBV, Deutsch H, Fessler RG, Buvanendran A and O'Toole JE: Enhanced recovery after surgery pathway for single-level minimally invasive transforaminal lumbar interbody fusion decreases length of stay and opioid consumption. Neurosurgery. 88:648–657. 2021.PubMed/NCBI View Article : Google Scholar
|
|
48
|
Wang L, Cai H, Wang Y, Liu J, Chen T, Liu J, Huang J, Guo Q and Zou W: Enhanced recovery after elective craniotomy: A randomized controlled trial. J Clin Anesth. 76(110575)2022.PubMed/NCBI View Article : Google Scholar
|
|
49
|
Greisman JD, Olmsted ZT, Crorkin PJ, Dallimore CA, Zhigin V, Shlifer A, Bedi AD, Kim JK, Nelson P, Sy HL, et al: Enhanced recovery after surgery (ERAS) for cranial tumor resection: A review. World Neurosurg. 163:104–122.e2. 2022.PubMed/NCBI View Article : Google Scholar
|
|
50
|
Suresh V, Ushakumari PR, Pillai CM, Kutty RK, Prabhakar RB and Peethambaran A: Implementation and adherence to a speciality-specific checklist for neurosurgery and its influence on patient safety. Indian J Anaesth. 65:108–114. 2021.PubMed/NCBI View Article : Google Scholar
|
|
51
|
Lepänluoma M, Takala R, Kotkansalo A, Rahi M and Ikonen TS: Surgical safety checklist is associated with improved operating room safety culture, reduced wound complications, and unplanned readmissions in a pilot study in neurosurgery. Scand J Surg. 103:66–72. 2014.PubMed/NCBI View Article : Google Scholar
|
|
52
|
Soriano Sánchez JA, Soriano Solís S and Romero Rangel JAI: Role of the checklist in neurosurgery, a realistic perspective to ‘The need for surgical safety checklists in neurosurgery now and in the future-a systematic review’. World Neurosurg. 134:121–122. 2020.PubMed/NCBI View Article : Google Scholar
|
|
53
|
Lau CY, Greysen SR, Mistry RI, Han SJ, Mummaneni PV and Berger MS: Creating a culture of safety within operative neurosurgery: The design and implementation of a perioperative safety video. Neurosurg Focus. 33(E3)2012.PubMed/NCBI View Article : Google Scholar
|
|
54
|
Enchev Y: Checklists in neurosurgery to decrease preventable medical errors: A review. Balkan Med J. 32:337–346. 2015.PubMed/NCBI View Article : Google Scholar
|
|
55
|
Da Silva-Freitas R, Martín-Laez R, Madrazo-Leal CB, Villena-Martin M, Valduvieco-Juaristi I, Martínez-Agüeros JÁ and Vázquez Barquero A: Establishment of a modified surgical safety checklist for the neurosurgical patient: Initial experience in 400 cases. Neurocirugia (Spain). 23:60–69. 2012.PubMed/NCBI View Article : Google Scholar : (In Spanish).
|
|
56
|
Schaffzin JK, Harte L, Marquette S, Zieker K, Wooton S, Walsh K and Newland JG: Surgical site infection reduction by the solutions for patient safety hospital engagement network. Pediatrics. 136:e1353–e1360. 2015.PubMed/NCBI View Article : Google Scholar
|
|
57
|
Pauli C, Schwarzbold ML, Diaz AP, De Oliveira Thais MER, Kondageski C, Linhares MN, Guarnieri R, De Lemos Zingano B, Ben J, Nunes JC, et al: Predictors of meaningful improvement in quality of life after temporal lobe epilepsy surgery: A prospective study. Epilepsia. 58:755–763. 2017.PubMed/NCBI View Article : Google Scholar
|
|
58
|
Tian B, He Y, Han Z, Liu T and Zhang X: Effect of powdered vancomycin on stopping surgical site wound infections in neurosurgery: A meta-analysis. Int Wound J. 20:1139–1150. 2022.PubMed/NCBI View Article : Google Scholar
|
|
59
|
Wang J, Ji Y, Wang N, Chen W, Bao Y, Qin Q, Ma C, Xiao Q and Li S: Establishment and validation of a delirium prediction model for neurosurgery patients in intensive care. Int J Nurs Pract. 26(e12818)2020.PubMed/NCBI View Article : Google Scholar
|
|
60
|
Annette H and Wenström Y: Implementing clinical guidelines for nutrition in a neurosurgical intensive care unit. Nurs Health Sci. 7:266–272. 2005.PubMed/NCBI View Article : Google Scholar
|
|
61
|
Krushelnytskyy MD, Youngblood MW, Lesniak MS, Kemeny HR, Fernandez LG, Burdett KLB, Zhang H, Alden TD and Dahdaleh NS: Optimizing the patient handoff and progress note documentation efficiency in the EPIC EMR system within a neurosurgery residency: A quality improvement initiative. J Clin Neurosci. 105:86–90. 2022.PubMed/NCBI View Article : Google Scholar
|
|
62
|
Kassicieh AJ, Varela S, Rumalla K, Kazim SF, Cole KL, Ghatalia DV, Schmidt MH and Bowers CA: Worse cranial neurosurgical outcomes predicted by increasing frailty in patients with interhospital transfer status: Analysis of 47,736 patients from the National Surgical Quality Improvement Program (NSQIP) 2015-2019. Clin Neurol Neurosurg. 221(107383)2022.PubMed/NCBI View Article : Google Scholar
|
|
63
|
Rotter J, Carlstrom LP, Graffeo CS, Nesvick CL, Gunnels M, Hellickson JD, Marcellino C and Atkinson JLD: Streamlining the external ventricular drain and intracranial pressure monitor procedural setup: A quality improvement initiative. World Neurosurg. 166:e475–e483. 2022.PubMed/NCBI View Article : Google Scholar
|
|
64
|
Schipmann S, Akalin E, Doods J, Ewelt C, Stummer W and Suero Molina E: When the infection hits the wound: Matched case-control study in a neurosurgical patient collective including systematic literature review and risk factors analysis. World Neurosurg. 95:178–189. 2016.PubMed/NCBI View Article : Google Scholar
|
|
65
|
Rubiano AM, Puyana JC, Mock CN, Bullock MR and Adelson PD: Strengthening neurotrauma care systems in low and middle income countries. Brain Inj. 27:262–272. 2013.PubMed/NCBI View Article : Google Scholar
|
|
66
|
Fischer C, Petriccione M, Donzelli M and Pottenger E: Improving care in pediatric neuro-oncology patients: An overview of the unique needs of children with brain tumors. J Child Neurol. 31:488–505. 2016.PubMed/NCBI View Article : Google Scholar
|
|
67
|
Bernstein M and Bampoe J: Surgical innovation or surgical evolution: An ethical and practical guide to handling novel neurosurgical procedures. J Neurosurg. 100:2–7. 2004.PubMed/NCBI View Article : Google Scholar
|
|
68
|
Leming-Lee T, Polancich S and Pilon B: The application of the toyota production system LEAN 5S methodology in the operating room setting. Nurs Clin North Am. 54:53–79. 2019.PubMed/NCBI View Article : Google Scholar
|
|
69
|
Hover AR, Sistrunk WW, Cavagnol RM, Scarrow A, Finley PJ, Kroencke AD and Walker JL: Effectiveness and cost of failure mode and effects analysis methodology to reduce neurosurgical site infections. Am J Med Qual. 29:517–521. 2014.PubMed/NCBI View Article : Google Scholar
|
|
70
|
Mathews L, Kla KM, Marolen KN, Sandberg WS and Ehrenfeld JM: Measuring and improving first case on-time starts and analysis of factors predicting delay in neurosurgical operating rooms. J Neurosurg Anesthesiol. 27:203–208. 2015.PubMed/NCBI View Article : Google Scholar
|
|
71
|
Rupich K, Missimer E, O'Brien D, Shafer G, Wilensky EM, Pierce JT, Kerr M, Kallan MJ, Dolce D and Welch WC: The benefits of implementing an early mobility protocol in postoperative neurosurgical spine patients. Am J Nurs. 118:46–53. 2018.PubMed/NCBI View Article : Google Scholar
|
|
72
|
Rozman PA, Kurland DB, Golub D, Trang M, Rothstein A, Lewis A and Pacione D: Venous duplex ultrasound surveillance in the neurosurgical population: A single-center quality improvement initiative. World Neurosurg. 144:e80–e86. 2020.PubMed/NCBI View Article : Google Scholar
|
|
73
|
Farrokhi FR, Gunther M, Williams B and Blackmore CC: Application of lean methodology for improved quality and efficiency in operating room instrument availability. J Healthc Qual. 37:277–286. 2015.PubMed/NCBI View Article : Google Scholar
|
|
74
|
Xu Y, Ren X, Shi W and Jiang H: Implementation of the best practice in nasogastric tube feeding of critically ill patients in a neurosurgical intensive care unit. Int J Evid Based Healthc. 11:128–133. 2013.PubMed/NCBI View Article : Google Scholar
|
|
75
|
Chang H, Silva MA, Giner A, Ancheta S, Romano JG, Komotar R and Cajigas I: Effects of an external ventricular drain alert protocol on venticulostomy placement time in the emergency department. Neurosurg Focus. 51(E4)2021.PubMed/NCBI View Article : Google Scholar
|
|
76
|
Joseph J, McLaughlin D, Darian V and Ezeamuzie N: Intraoperative use of low-profile alternating pressure mattress for prevention of hospital-acquired pressure injury. Perioper Care and Oper Room Manage. 17(100080)2019.
|
|
77
|
Kantelhardt P, Müller M, Giese A, Rohde V and Kantelhardt SR: Implementation of a critical incident reporting system in a neurosurgical department. Cent Eur Neurosurg. 72:15–21. 2011.PubMed/NCBI View Article : Google Scholar
|
|
78
|
Ryan SL, Sen A, Staggers K, Luerssen TG and Jea A: Texas Children's Hospital Spine Study Group. A standardized protocol to reduce pediatric spine surgery infection: A quality improvement initiative. J Neurosurg Pediatr. 14:259–265. 2014.PubMed/NCBI View Article : Google Scholar
|
|
79
|
Kantelhardt P, Giese A and Kantelhardt SR: Medication reconciliation for patients undergoing spinal surgery. Eur Spine J. 25:740–747. 2016.PubMed/NCBI View Article : Google Scholar
|
|
80
|
Licina A, Silvers A, Laughlin H, Russell J and Wan C: Pathway for enhanced recovery after spinal surgery-a systematic review of evidence for use of individual components. BMC Anesthesiol. 21(74)2021.PubMed/NCBI View Article : Google Scholar
|
|
81
|
Young R, Cottrill E, Pennington Z, Ehresman J, Ahmed AK, Kim T, Jiang B, Lubelski D, Zhu AM, Wright KS, et al: Experience with an Enhanced Recovery After Spine Surgery protocol at an academic community hospital. J Neurosurg Spine. 34:680–687. 2020.PubMed/NCBI View Article : Google Scholar
|
|
82
|
Kamil M, Muttaqin Z, Hanaya R, Arita K and Yoshimoto K: Bibliometric analysis of the neurosurgery publication productivity of Southeast Asia in 2011-2020. World Neurosurg. 172:e490–e498. 2023.PubMed/NCBI View Article : Google Scholar
|
|
83
|
Hines K, Mouchtouris N, Knightly JJ and Harrop J: A brief history of quality improvement in health care and spinal surgery. Global Spine J. 10 (1_suppl):5S–9S. 2020.PubMed/NCBI View Article : Google Scholar
|
|
84
|
Rock AK, Opalak CF, Workman KG and Broaddus WC: Safety Outcomes Following Spine and Cranial Neurosurgery: Evidence From the National Surgical Quality Improvement Program. J Neurosurg Anesthesiol. 30:328–336. 2018.PubMed/NCBI View Article : Google Scholar
|



















