Introduction
Pancreatic cancer is a major cause of cancer-related
mortality worldwide, the 5-year survival rate being 2–6% (1,2). Indeed,
even in patients who undergo resection, the 5-year survival rate is
poor at between 7 and 24%, whereas the median survival time is
about 1 year in the majority of series (3). Certainly, the prognosis of unresectable
or recurrent patients is even worse. Recently, the advent of
nab-paclitaxel (nab-PTX) plus gemcitabine (GEM) therapy and 5-FU,
leucovorin, irinotecan and oxaliplatin (FOLFIRINOX) therapy offered
a ray of hope for treatment of unresectable pancreatic cancer
(4,5). Prior to appearance of these powerful
regimens, no third-line chemotherapy was recommended after 5-FU and
GEM-based regimens. In addition, such a powerful treatment can no
longer be used gradually in the terminal stage. Palliative
chemotherapy superior to best supportive care (BSC) is required at
such time.
Paclitaxel (PTX) is an anticancer agent used for
various malignant diseases previously (6) that stabilizes polymerized microtubules
and enhances microtubule assembly, which arrests the cell cycle in
G0/G1 and G2/M phases, and leads to cell death (7,8).
Low-dose PTX ameliorates tissue fibrosis by inhibiting the activity
of transforming growth factor (TGF)-β/Smad activity (9,10).
Therefore, we reasoned that paclitaxel might be useful for treating
patients with pancreatic and biliary tract cancer (BTC) associated
with tissue fibrosis.
We found that low-dose PTX inhibits the epithelial
mesenchymal transition (EMT) of cholangiocarcinoma cells treated
with TGF-β (11). Furthermore, we
studied the responses of patients with BTC treated with low-dose
PTX as palliative chemotherapy following GEM and S-1 (oral prodrug
of 5-FU) (12,13). Thereafter, we planned a Phase I
clinical trial to determine the optimal dose of weekly low-dose PTX
therapy as third-line palliative chemotherapy for patients with
pancreatic cancers after failure of S-1 and GEM.
Patients and methods
Patient selection
Patients with unresectable or recurrent pancreatic
cancers after excision who had been treated with GEM and S-1 were
eligible for this study. Other inclusion criteria were as follows:
age 20–80 years, Eastern Cooperative Oncology Group (ECOG)
performance status ≤1 (ambulatory and capable of self-care),
adequate renal function (normal serum creatinine and blood urea
nitrogen concentrations), adequate liver function (total bilirubin,
<2.5-times the upper normal limit [UNL] or <triple the UNL
after biliary drainage in patients with jaundice and serum
transaminase [GOT, GPT] concentrations <2.5-times the UNL or
<triple the UNL after biliary drainage in patients with
jaundice), adequate bone marrow reserve (white blood cell count,
4.0–12.0×109/l; neutrophil count, >2.0×109/l; platelet count,
>100×109/l; and hemoglobin >95 g/l), and adequate pulmonary
function (PaO2, >70 mmHg). Patients with a history of
treatment for pancreatic cancer must have discontinued such
treatment (tumor resection, chemotherapy, immunotherapy, or
radiotherapy) ≥2 weeks before enrolment.
Exclusion criteria were as follows: pulmonary
fibrosis or interstitial pneumonia, marked pleural or pericardial
effusion, marked peripheral edema, severe heart disease,
difficult-to-control diabetes mellitus, active infection, pregnancy
or lactation, women of childbearing age not using effective
contraception, severe drug hypersensitivity, severe neurological
impairment, severe mental disorder, active concomitant malignancy,
previous history of PTX administration, complications of another
malignancy, and other serious medical conditions.
Written informed consent was obtained from each
patient before enrolment, and the Institutional Review Board of
Kanazawa University Hospital approved this study (UMIN ID:
000008148).
Study design
This was an open-label, single-center,
non-randomized, dose-escalation Phase I study. Laboratory tests to
assess eligibility were completed within 7 days before commencing
treatment. PTX was administered as a 60-min intravenous infusion on
Days 1, 8, 15, and 22 of each cycle. A second cycle was then
administered at the specified higher dose level beginning on Day
28. The doses of PTX were planned as follows: Level 1, 40
mg/m2; Level 2, 50 mg/m2. If the treatment
was found to be effective after two cycles, it was continued weekly
or biweekly for as long as possible.
Definition of dose-limiting toxicity
(DLT) and maximum tolerated dose (MTD)
DLT was determined during each treatment cycle and
defined according to the National Cancer Institute's Common
Toxicity Criteria scale (version 4.0) (http://ctep.cancer.gov/protocolDevelopment/electronic_applications/ctc.htm
#ctc_40) as one or more of the effects attributable to the study
drug as follows: i) Grade 3/4 neutropenia complicated by fever; ii)
Grade 4 neutropenia >4 days; iii) Grade 4 thrombocytopenia; iv)
any other Grade 3/4 nonhematologic toxicity except anorexia,
nausea, and vomiting in the absence of an appropriate antiemetic;
and v) delay of recovery from treatment-related toxicity for more
than 2 weeks. At least three patients received each dose level. If
DLT was observed after the first cycle in more than two patients,
treatment at that dose was discontinued. If DLT was observed after
the first cycle in one patient, three additional patients were
administered that dose level. If only one of six patients
experienced DLT, dose escalation was continued. The MTD of the
combination was defined as the dose that produced DLT in more than
two of six patients or in the initial three patients. The
recommended dose (RD) was defined as the dose that was one level
below the MTD. Because the aim was palliation, if Level 2 was less
than the MTD, no further dose escalation was implemented and Level
2 became the RD.
Assessment of efficacy
Tumor responses were evaluated according to the
Response Evaluation Criteria in Solid Tumors (14). Complete response (CR) was defined as
disappearance of clinical evidence of the tumor. Partial response
(PR) was defined as a ≥30% reduction in the sum of the products of
two orthogonal diameters of all measurable lesions compared with
baseline values with no evidence of new lesions. Stable disease
(SD) was defined as <30% reduction or <20% increase in the
sum of the products of two orthogonal diameters of all measurable
lesions compared with baseline values with no evidence of new
lesions. Progressive disease (PD) was defined as ≥20% increase in
the sum of the products of two orthogonal diameters of all
measurable lesions compared with baseline values, appearance of a
new lesion, or deterioration in clinical status consistent with
disease progression. Patients were evaluated for objective evidence
of response after two cycles of chemotherapy. Additionally,
concentrations of the tumor markers carcinoembryonic antigen (CEA),
cancer antigen (CA)19-9 and Duke pancreatic monoclonal antigen type
2 (DUPAN-2) were measured before and after two treatment
cycles.
Statistical analysis
The median survival time (MST) and OS were
calculated from the start of treatment until death and were
determined using the Kaplan-Meier method. The significance of
differences CEA and CA19-9 concentrations were evaluated using
Student's paired t-test after logarithmic transformation of the
values and p<0.05 was considered to indicate statistical
significance. A SPSS statistical package (version 19; SPSS,
Chicago, IL, USA) was used to perform the analyses.
Results
From May 2012 to January 2014, 10 patients (three
men and seven women) diagnosed as having recurrent or unresectable
pancreatic cancers after failure of GEM and oral S-1 were enrolled
in this study. The patients' characteristics and the effects of
treatment are listed in Table I.
Treatment was administered at Level 1 (40 mg/m2) to six
patients and Level 2 (50 mg/m2) to four patients. The
following responses were documented: PR, none of 10 patients
(0.0%); SD, four (40.0%); and PD, six (60.0%); thus, the disease
control rate (PR+SD) was 40.0%. During the two courses of therapy,
Grade 1 or 2 adverse events occurred in all patients, dose-limiting
adverse events (Grade 3 or 4) occurring in three patients receiving
Level 2. However, eight patients completed two courses of
treatment, the remaining two discontinuing treatment because of
disease progression. Adverse events were as follows: epilation
(100.0%), anemia (100.0%), neutropenia (Grade 1 or 2: 20.0%, Grade
3 or 4: 30.0%), thrombocytopenia (10.0%), general malaise (40.0%),
and liver dysfunction (20.0%). No significant neuropathy or
anorexia were observed during the two treatment cycles (Table II). Dose-limiting adverse events
(Grade 3 or 4) occurred in three of four patients receiving Level 2
(neutropenia). Thus, dose escalation was aborted at Level 2 and
Level 1 was defined as MTD and RD.
 | Table I.Patient's characteristics and
treatment effects. |
Table I.
Patient's characteristics and
treatment effects.
| No. | Age, years | Sex | Tumor location | Dose
(mg/m2) | Operation | Treatment effect | TTF (months) |
|---|
| 1 | 65 | F | BT | 40 | + | PD | 0 |
| 2 | 61 | F | BT | 40 | + | PD | 0 |
| 3 | 65 | F | BT | 40 | − | PD | 0 |
| 4 | 62 | F | H | 40 | + | SD | 9 |
| 5 | 65 | F | BT | 40 | − | PD | 0 |
| 6 | 74 | F | BT | 40 | + | SD | 4 |
| 7 | 69 | M | BT | 50 | − | PD | 0 |
| 8 | 45 | M | BT | 50 | − | PD | 0 |
| 9 | 62 | F | BT | 50 | + | SD | 4 |
| 10 | 71 | M | H | 50 | + | SD | 5 |
 | Table II.Adverse events. |
Table II.
Adverse events.
|
| Grade 1, 2 | Grade 3, 4 |
|---|
| Neutropenia | 2 (20.0%) | 3 (30.0%) |
| Anemia | 10 (100%) | 0 |
|
Thrombocytopenia | 1 (10.0%) | 0 |
| Anorexia | 0 | 0 |
| General
malaise | 4 (40.0%) | 0 |
| Liver
dysfunction | 3 (30.0%) | 0 |
| Neuropathy | 0 | 0 |
| Epilation | 10 (100%) | − |
Before treatment, CEA concentrations were high
(>5 ng/ml) in six of 10 patients, CA-19-9 concentrations (>37
U/ml) in nine of 10 patients, and DUPAN-2 concentrations (>150
U/ml) in seven of 10 patients. CEA and DUPAN-2 concentrations each
decreased in only one patient, whereas CA19-9 concentrations
decreased in four patients; however, the decreases in these tumor
marker concentration were not significant (data not shown).
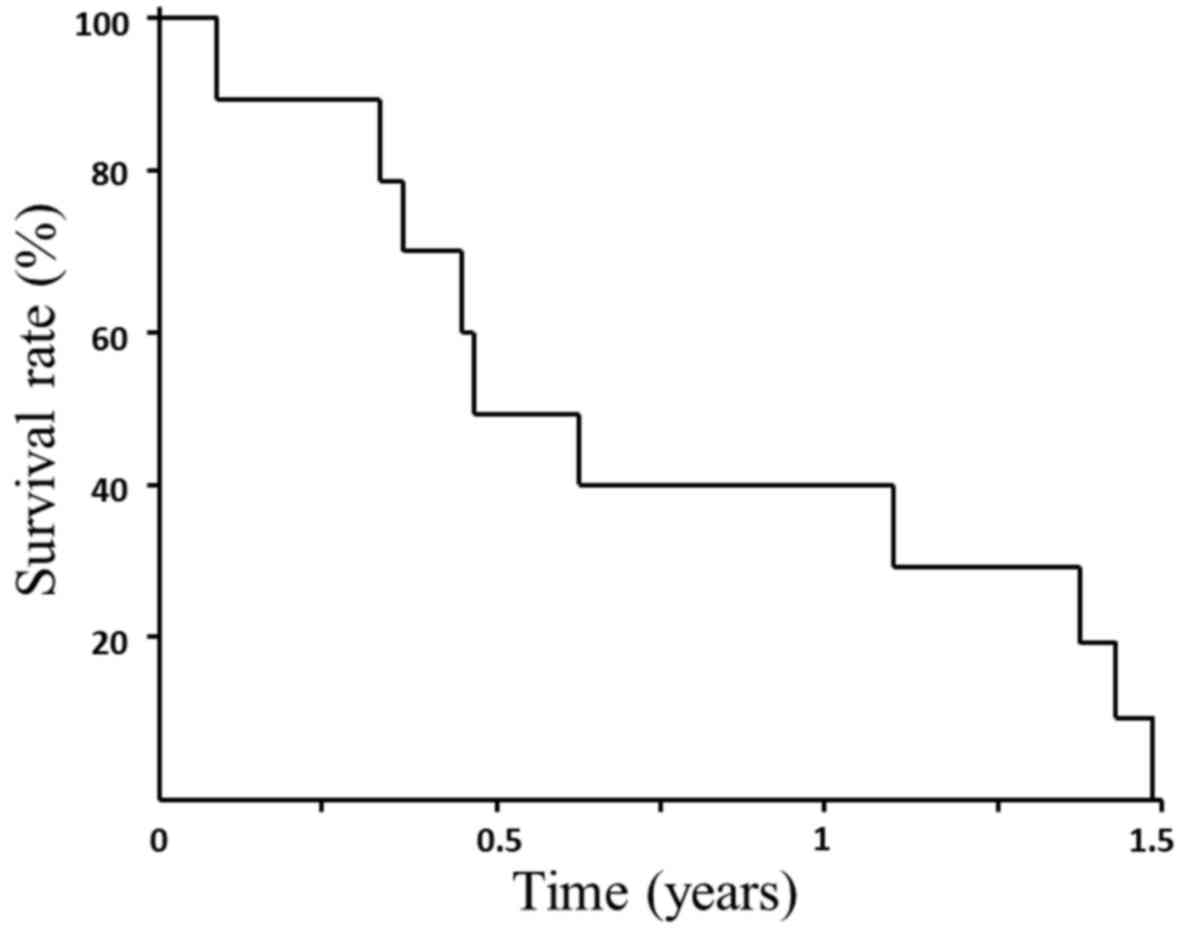
OS from the start of treatment until death and MST
were 0.77 months (range: 0.45–1.09) and 0.47 months, respectively
(Fig. 1).
Discussion
Before development of nab-PTX+GEM and FOLFIRINOX
therapies, the key drugs for treating pancreatic cancer were 5-FU
and GEM. 5-FU was the major drug used to treat
hepatobiliary-pancreatic cancers; however, Phase II studies of
combinations based primarily on 5-FU regimens show little or no
benefit in survival or quality of life (11,12). In
a Phase III GEST trial, S-1, an oral prodrug of 5-FU that is widely
used in Japan, achieved favorable responses and was not inferior to
GEM for increasing the OS of patients with unresectable pancreatic
cancer (15). Moreover, the JASPAC
01 trial found that S-1 prior to GEM is effective adjuvant
chemotherapy for resected pancreatic cancer (16). However, there was no recommended
third-line chemotherapy following GEM and 5-FU for treating
patients with pancreatic cancer.
PTX is isolated from the Western Yew, Taxus
brevifolia (4). Similar to vinca
alkaloids, it binds microtubules. However, whereas vinca alkaloids
promote microtubule dissociation and disruption of the mitotic
spindle, PTX promotes microtubule formation and stabilization. Both
retrospective studies and Phase I and II studies of PTX and
docetaxel (taxanes) on treating patients with pancreatic cancer
(17–20) have reported disease control rates of
33–57% when this regimen is used as first or second line
chemotherapy.
PTX is currently receiving attention for its effects
on pathologies other than cancers. For example, PTX is incorporated
into drug-eluting stents placed in coronary arteries (21). Moreover, PTX ameliorates fibrosis in
hepatic stellate cells and renal fibrosis through inhibition of
TGF-β/Smad activity (9,10). Further, paclitaxel inhibits paracrine
TGF-β1 signaling between gallbladder epithelial cells and
myofibroblasts (22).
PTX decreases interstitial fluid pressure and
improves oxygenation of breast cancer tissues of patients treated
with neoadjuvant chemotherapy (23).
Thus, taxanes may be effective for treating fibrous hypoxic tumors
such as pancreatic cancer. For example, nab-PTX + GEM therapy
increases the treatment options for patients with pancreatic cancer
(24); this therapy disrupts stroma
in these patients (25).
Taxanes are used to treat patients with
GEM-refractory pancreatic cancer (26,27).
Anticancer drugs, irradiation, hypoxia, malnutrition, and heat
induce EMT of cancer cells and activation of fibroblasts, which is
involved in the invasive potential of cancer cells and cancer
associated fibroblasts (28). The
inhibitory effect of PTX on TGF-β/Smad activity contributes to
suppression of the EMT (9).
We have previously reported that PTX is more
effective, as assessed by time to treatment failure, than GEM and
S-1 for treating patients with unresectable gallbladder cancer
(10). Thus, a Phase I study of
low-dose PTX, which has fewer adverse effects, is warranted for
palliative chemotherapy in patients with BTCs (13). Of note, PTX is an established
palliative chemotherapy agent for treating patients with breast
cancer (29). In the present Phase I
study, we demonstrated the efficacy and safety of weekly low-dose
PTX as third-line chemotherapy for patients with pancreatic cancer.
Moreover, 40 mg/m2 of PTX was the MTD after 8 weeks of
weekly administration, and thus defined as RD. A past study to
determine the appropriate dose of PTX in patients with BTCs was
terminated at 50 mg/m2 (13). Moreover, low dose PTX as third line
palliative chemotherapy was found to be more effective in patients
with BTC than in those with pancreatic cancer. These results
suggest that the general condition of patients with pancreatic
cancer may be poorer than that of patients with BTC considering
third line chemotherapy. However, this study is just a phase I;
comparison with placebo or BSC group is necessary in phase II study
in the future.
In conclusion, after failure of therapy with GEM and
5-FU, palliative chemotherapy with low-dose PTX is well-tolerated
and safe in patients with unresectable or recurrent pancreatic
cancer, the RD being 40 mg/m2. In the future, it is
considered that Phase II trial and Phase III trial compared with
BSC are necessary.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
The authors, MO, TY, YO, KOk, SN, ST, SS, JK and IM,
conducted chemotherapy on patients, KN, HH, KOy, MI and TM
contributed to the clinical data analysis, HTaj, HTak, IN and SF
contributed the clinical trial operation. TO conducted the clinical
study. All authors read and approved the final manuscript.
Ethics approval and consent to
participate
Written informed consent was obtained from each
patient prior to enrolment, and the present study was approved by
the Institutional Review Board of Kanazawa University Hospital
(Takaramaci, Japan).
Competing interests
The authors declare that they have no competing
interests
References
|
1
|
Von Hoff DD, Ervin T, Arena FP, Chiorean
EG, Infante J, Moore M, Seay T, Tjulandin SA, Ma WW, Saleh MN, et
al: Increased survival in pancreatic cancer with nab-paclitaxel
plus gemcitabine. N Engl J Med. 369:1691–1703. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Suker M, Beumer BR, Sadot E, Marthey L,
Faris JE, Mellon EA, El-Rayes BF, Wang-Gillam A, Lacy J, Hosein PJ,
et al: FOLFIRINOX for locally advanced pancreatic cancer: A
systematic review and patient-level meta-analysis. Lancet Oncol.
17:801–810. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Evans DB, Abbruzzese JL and Willett CG:
Cancer of the pancreasCancer: Principles and Practice of Oncology.
6th. DeVita VT Jr, Hellman S and Rosenberg SA: Lippincott Williams
and Wilkins; Philadelphia: pp. 1126–1161. 2001
|
|
4
|
Von Hoff DD, Ramanathan RK, Borad MJ,
Laheru DA, Smith LS, Wood TE, Korn RL, Desai N, Trieu V, Iglesias
JL, et al: Gemcitabine plus nab-paclitaxel is an active regimen in
patients with advanced pancreatic cancer: A phase I/II trial. J
Clin Oncol. 29:4548–4554. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Conroy T, Desseigne F, Ychou M, Bouché O,
Guimbaud R, Bécouarn Y, Adenis A, Raoul JL, Gourgou-Bourgade S, de
la Fouchardière C, et al Groupe Tumeurs Digestives of Unicancer, ;
PRODIGE Intergroup, : FOLFIRINOX versus gemcitabine for metastatic
pancreatic cancer. N Engl J Med. 364:1817–1825. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Gelmon K: The taxoids: Paclitaxel and
docetaxel. Lancet. 344:1267–1272. 1994. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Donaldson KL, Goolsby GL, Kiener PA and
Wahl AF: Activation of p34cdc2 coincident with taxol-induced
apoptosis. Cell Growth Differ. 5:1041–1050. 1994.PubMed/NCBI
|
|
8
|
Schiff PB, Fant J and Horwitz SB:
Promotion of microtubule assembly in vitro by taxol. Nature.
277:665–667. 1979. View
Article : Google Scholar : PubMed/NCBI
|
|
9
|
Zhang D, Sun L, Xian W, Liu F, Ling G,
Xiao L, Liu Y, Peng Y, Haruna Y and Kanwar YS: Low-dose paclitaxel
ameliorates renal fibrosis in rat UUO model by inhibition of
TGF-beta/Smad activity. Lab Invest. 90:436–447. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhou J, Zhong DW, Wang QW, Miao XY and Xu
XD: Paclitaxel ameliorates fibrosis in hepatic stellate cells via
inhibition of TGF-β/Smad activity. World J Gastroenterol.
16:3330–3334. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Hirose A, Tajima H, Ohta T, Tsukada T,
Okamoto K, Nakanuma S, Sakai S, Kinoshita J, Makino I, Furukawa H,
et al: Low-dose paclitaxel inhibits the induction of
epidermal-mesenchymal transition in the human cholangiocarcinoma
CCKS-1 cell line. Oncol Lett. 6:915–920. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Tajima H, Ohta T, Shinbashi H, Hirose A,
Tsukada T, Okamoto K, Nakanuma S, Sakai S, Furukawa H, Makino I, et
al: Successful treatment of unresectable gallbladder cancer with
low-dose paclitaxel as palliative chemotherapy after failure of
gemcitabine and oral S-1: A case report. Oncol Lett. 4:1281–1284.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Tajima H, Ohta T, Shinbashi H, Hirose A,
Okazaki M, Yamaguchi T, Ohbatake Y, Okamoto K, Nakanuma S, Sakai S,
et al: Phase I study of weekly palliative chemotherapy with
low-dose third-line paclitaxel for biliary tract cancer. Mol Clin
Oncol. 6:753–757. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Eisenhauer EA, Therasse P, Bogaerts J,
Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S,
Mooney M, et al: New response evaluation criteria in solid tumours:
Revised RECIST guideline (version 1.1). Eur J Cancer. 45:228–247.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Ueno H, Ioka T, Ikeda M, Ohkawa S,
Yanagimoto H, Boku N, Fukutomi A, Sugimori K, Baba H, Yamao K, et
al: Randomized phase III study of gemcitabine plus S-1, S-1 alone,
or gemcitabine alone in patients with locally advanced and
metastatic pancreatic cancer in Japan and Taiwan: GEST study. J
Clin Oncol. 31:1640–1648. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Uesaka K, Boku N, Fukutomi A, Okamura Y,
Konishi M, Matsumoto I, Kaneoka Y, Shimizu Y, Nakamori S, Sakamoto
H, et al JASPAC 01 Study Group, : Adjuvant chemotherapy of S-1
versus gemcitabine for resected pancreatic cancer: A phase 3,
open-label, randomised, non-inferiority trial (JASPAC 01). Lancet.
388:248–257. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Okada S, Sakata Y, Matsuno S, Kurihara M,
Sasaki Y, Ohashi Y and Taguchi T; Cooperative Group of Docetaxel
for Pancreatic Cancer in Japan, : Phase II study of docetaxel in
patients with metastatic pancreatic cancer: A Japanese cooperative
study. Br J Cancer. 80:438–443. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Ryan DP, Kulke MH, Fuchs CS, Grossbard ML,
Grossman SR, Morgan JA, Earle CC, Shivdasani R, Kim H, Mayer RJ, et
al: A Phase II study of gemcitabine and docetaxel in patients with
metastatic pancreatic carcinoma. Cancer. 94:97–103. 2002.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Jones DV Jr, Lozano R, Hoque A, Markowitz
A, Patt YZ and Phase II: Phase II study of paclitaxel therapy for
unresectable biliary tree carcinomas. J Clin Oncol. 14:2306–2310.
1996. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Maeda S, Motoi F, Onogawa T, Morikawa T,
Shigeru O, Sakata N, Takadate T, Naitoh T, Rikiyama T, Katayose Y,
et al: Paclitaxel as second-line chemotherapy in patients with
gemcitabine-refractory pancreatic cancer: A retrospective study.
Int J Clin Oncol. 16:539–545. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Baek I, Bai CZ, Hwang J, Nam HY, Park JS
and Kim DJ: Paclitaxel coating of the luminal surface of
hemodialysis grafts with effective suppression of neointimal
hyperplasia. J Vasc Surg. 55:806–814.e1. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Choi HS, Savard CE, Choi JW, Kuver R and
Lee SP: Paclitaxel interrupts TGF-beta1 signaling between
gallbladder epithelial cells and myofibroblasts. J Surg Res.
141:183–191. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Taghian AG, Abi-Raad R, Assaad SI, Casty
A, Ancukiewicz M, Yeh E, Molokhia P, Attia K, Sullivan T, Kuter I,
et al: Paclitaxel decreases the interstitial fluid pressure and
improves oxygenation in breast cancers in patients treated with
neoadjuvant chemotherapy: Clinical implications. J Clin Oncol.
23:1951–1961. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Von Hoff DD, Ramanathan RK, Borad MJ,
Laheru DA, Smith LS, Wood TE, Korn RL, Desai N, Trieu V, Iglesias
JL, et al: Gemcitabine plus nab-paclitaxel is an active regimen in
patients with advanced pancreatic cancer: A phase I/II trial. J
Clin Oncol. 29:4548–4554. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Alvarez R, Musteanu M, Garcia-Garcia E,
Lopez-Casas PP, Megias D, Guerra C, Muñoz M, Quijano Y, Cubillo A,
Rodriguez-Pascual J, et al: Stromal disrupting effects of
nab-paclitaxel in pancreatic cancer. Br J Cancer. 109:926–933.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Shukuya T, Yasui H, Boku N, Onozawa Y,
Fukutomi A, Yamazaki K, Taku K, Kojima T and Machida N: Weekly
Paclitaxel after failure of gemcitabine in pancreatic cancer
patients with malignant ascites: A retrospective study. Jpn J Clin
Oncol. 40:1135–1138. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Cereda S and Reni M: Weekly docetaxel as
salvage therapy in patients with gemcitabine-refractory metastatic
pancreatic cancer. J Chemother. 20:509–512. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Tajima H, Ohta T, Shoji Y, Watanabe T,
Makino I, Hayashi H, Nakagawara H, Onishi I, Takamura H, Ninomiya
I, et al: Expression of epithelial-mesenchymal transition markers
in locally recurrent hepatocellular carcinoma after radio frequency
ablation. Exp Ther Med. 1:347–350. 2010. View Article : Google Scholar
|
|
29
|
Schrama JG, de Boer MM, Baars JW,
Schornagel JH and Rodenhuis S: Palliative chemotherapy after
failure of high-dose chemotherapy in breast cancer-toxicity and
efficacy. Anticancer Res. 23(3C): 1–2800. 2003.PubMed/NCBI
|