Introduction
Atrial fibrillation (AF) is a highly prevalent
disease encountered in clinical practice, which results in
cardiovascular morbidity and mortality (1), and is difficult to treat (2). AF patients are treated using certain
therapeutic strategies, such as electrical cardioversion, tissue
ablation and pharmacological therapy. However, electrical
cardioversion and tissue ablation require anesthesia, which may be
associated with periprocedural complications. Pharmacological
therapy is considered to be the most important treatment of AF,
particularly in elderly populations. However, currently available
pharmacological therapeutic modalities for terminating AF or
maintaining sinus rhythm are only moderately effective.
Furthermore, these drugs may induce ventricular pro-arrhythmia
(3). Therefore, the development of
effective and safe therapeutic strategies to treat AF is important.
An improved understanding of the anti-arrhythmic mechanisms of the
effective drugs may facilitate the improvement of therapeutic
strategies. Drugs are conventionally grouped according to their
anti-arrhythmic mechanism of action, such as: i) Na+
channel blockade, ii) β-adrenoceptor antagonism, iii) action
potential prolonging, and iv) Ca2+ channel blockade.
Certain drugs have various classes that act to inhibit AF, such as
amiodarone, a class III drug, has multiple actions for blocking
numerous ion currents (INa, INa/Ca,
ICaL, ICaT, Ito, IKur,
IKr, IKS, IK1 and
IKACh) and adrenergic/cholinergic receptors. The current
therapeutic strategies for the management of AF recommend the
administration of specified drugs for rate control depending on the
patient's state (4). Amiodarone is
recommended for treating recent onset or persistent AF and
preventing AF recurrence. When other methods are unsuccessful for
rate control, amiodarone is an alternative approach. However,
amiodarone has serious side effects, and may adversely affect
numerous organs and tissues (5,6). The other
class III drug, ibutilide, is recommended for treatment of AF or
atrial flutter, although there is a risk of ventricular
pro-arrhythmia, most likely due to inhibition of IKr,
which induced QT prolongation (4).
Amiodarone and ibutilide are two of the most effective class III
antiarrhythmic drugs for cardioversion of acute onset AF; however,
their efficacy in persistent AF of long duration is limited
(7–9).
Thus, the aim of the current study was to
investigate whether the combination of amiodarone and ibutilide
with different treatment processes improves the treatment success
rates in persistent AF. In the present study, the efficacy and
safety of treatment with amiodarone plus ibutilide, vs. ibutilide
alone, on cardioversion of persistent AF and maintenance time of
sinus rhythm was compared.
Materials and methods
Patients
The study recruited 79 patients (48 males and 31
females; mean age, 64.6±11.2 years; range, 40–80 years) with
non-valvular chronic AF lasting >7 days (range, 7–97 days) who
had been referred to The First Affiliated Hospital of Harbin
Medical University (Harbin, China) for cardioversion of persistent
AF between June 2013 and April 2014. Exclusion criteria for the
study were as follows: Patients with i) acute coronary syndrome;
ii) severe structural heart disease; iii) ventricular arrhythmia;
iv) ventricular rate <50 times per min; v) left ventricular
ejection fraction (LVEF) <35%. Written informed consent was
obtained from all patients for the present study, which involved
internal atrial defibrillation, electrophysiology studies, and
intravenous administration of amiodarone and/or ibutilide. The
study was approved by the Clinical Research Committee of The First
Affiliated Hospital of Harbin Medical University.
Study protocol
Treatment with antiarrhythmic drugs (excluding
Digitalis, β-blockers and calcium channel antagonists) was
discontinued at least 5 half-lives prior to the study. Patients
that had already been treated with amiodarone were not included in
the current study. A placebo was administered to 39 patients, and
amiodarone (Sanofi Winthrop Industrie, Floirac, France) was
administered intravenously (dose, 300 mg) to 40 patients, then 30
min later ibutilide (Feng Yuan Pharmaceutical Co., Ltd., Maanshan,
China) was administered (dose, 1 mg) to all patients, resulting in
an ibutilide treatment group (ibutilide alone; n=39) and an
amiodarone + ibutilide co-treatment group (amiodarone + ibutilide;
n=40). The administered quantities were based on typical clinical
doses.
Electrocardiography recordings were obtained prior
to administration of the drugs and subsequently at 30, 60, 75, 95,
105 and 120 min. The electrocardiography (ECG) recording speed was
25 mm/sec and the voltage was 1 mV/cm. Noise was minimized using a
digital filter. Analyses of the ECG waves were performed to
calculate heart rate (HR; bpm), QRS duration (msec), QT interval
(msec) and PR interval (msec). Corrected QT for HR was established
using Bazett's formula: [QTc=QT/(square root of RR interval)]. For
each data point, measurements were obtained at three
non-consecutive, randomly selected points in every 5-min recording.
The results are presented as the mean of three randomly selected
segments.
Follow-up
At baseline and at the follow-up visits, patients
underwent physical examination, transthoracic echocardiography,
resting electrocardiogram, blood pressure measurement, and
assessment of quality of life and symptoms. For those who were not
followed up at The First Affiliated Hospital of Harbin Medical
University, attempts were made to contact the patients or their
relatives. In addition, hospital records were reviewed and all
cardiac events were confirmed by a review of hospital records.
Statistical analysis
Values are expressed as means ± standard deviation.
The clinical characteristics of the patients were analyzed using
the Mann-Whitney U test. Differences between pre- and
post-treatment HR, effective refractory period and QTc within each
group were analyzed using the Wilcoxon signed-rank test. P<0.05
was considered to indicate a statistically significant difference.
All statistical analyses were performed using SPSS 13.0 software
(SPSS, Inc., Chicago, IL, USA).
Results
Clinical characteristics of the
patients
The current study included 79 patients (48 males and
31 females), which were divided into two groups, the ibutilide
treatment group (ibutilide alone; n=39) and the amiodarone +
ibutilide co-treatment group (amiodarone + ibutilide; n=40). No
significant differences were identified between the two groups with
regard to clinical characteristics and basic diseases (Table I).
 | Table I.Baseline characteristics of the two
groups. |
Table I.
Baseline characteristics of the two
groups.
| Variable | Ibutilide (n=39) | Amiodarone +
ibutilide (n=40) | P-value |
|---|
| Age (years) | 65.64±8.59 | 61.73±12.34 | 0.147 |
| Male/female | 22/17 | 26/14 | 0.558 |
| Atrial fibrillation
duration (days) | 26.31±24.38 | 29.97±28.67 | 0.641 |
| Coronary artery
disease (%) | 51.31 | 47.11 | 0.861 |
| Hypertension (%) | 56.41 | 61.12 | 1.002 |
| Diabetes (%) | 5.11 | 6.24 | 0.580 |
| Heart failure
(%) | 29.71 | 28.35 | 1.030 |
| Potassium ion
(mM) | 4.52±0.37 | 4.43±0.31 | 0.993 |
| Magnesium ion
(mM) | 0.81±0.09 | 0.91±0.11 | 0.755 |
| Left atrial size
(mm) | 40.86±4.12 | 40.97±4.24 | 0.963 |
| LV end-diastolic
dimension (mm) | 50.23±6.31 | 51.17±7.31 | 0.981 |
| LV ejection fraction
(%) | 57.34±9.73 | 56.66±9.19 | 0.187 |
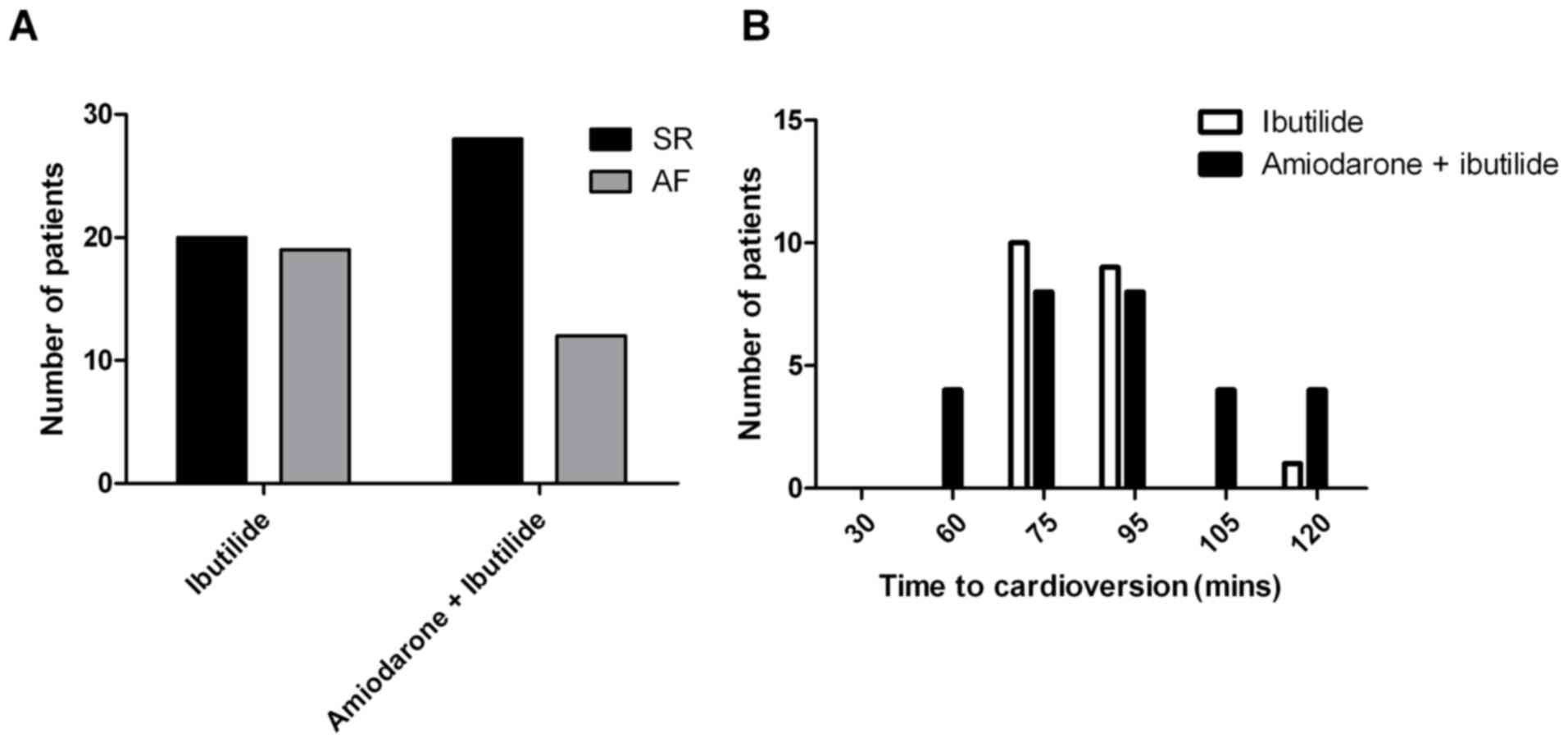
Cardioversion rate
A total of 48 patients were successfully converted
to sinus rhythm, there were 20 patients from the control group
(ibutilide treatment alone; rate of cardioversion, 51.3%) and 28
from the study group (co-treatment of amiodarone + ibutilide; rate
of cardioversion, 71.8%). A significant difference in the number of
patients successfully converted to SR was identified between the
two groups (P<0.05; Fig. 1A). There
were 10, 9 and 1 patients successfully converted to sinus rhythm in
75, 95 and 120 min, respectively, in the ibutilide treatment group.
There were 4, 8, 8, 4 and 4 patients successfully converted to
sinus rhythm in 60, 75, 95, 105 and 120 min, respectively in the
amiodarone and ibutilide co-treatment group (Fig. 1B). The timing of conversion to sinus
rhythm in the two groups displayed two distinct peaks at 75 and 95
min after the onset of drug administration (Fig. 1B). Furthermore, no significant
differences in demographic and clinical characteristics were
identified between the patients who successfully converted to sinus
rhythm and those who continued to exhibit AF.
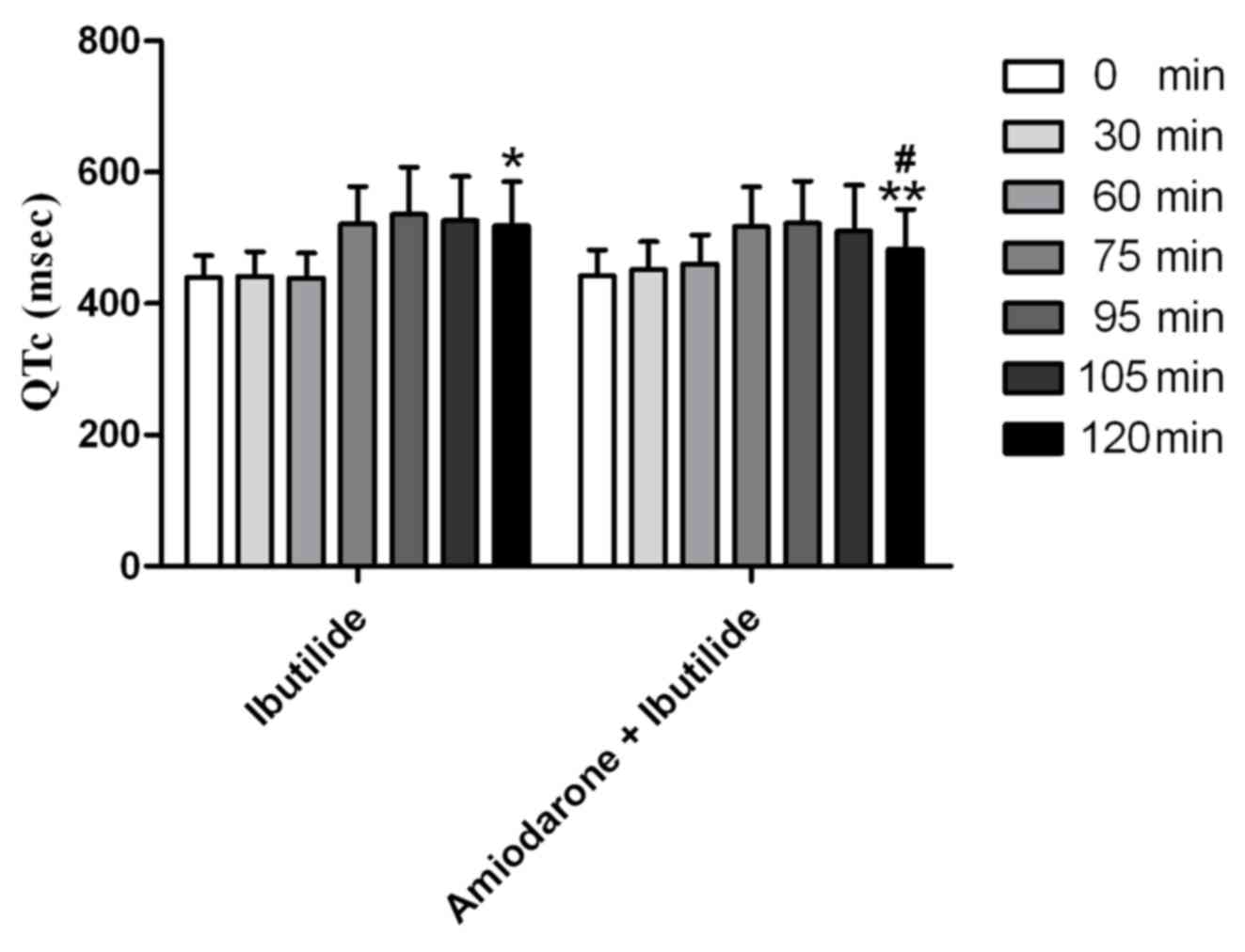
QTc interval prolongation
The QTc interval was significantly prolonged in the
two groups, from 440.7±38.1 to 520.6±69.3 msec (P<0.05) in the
ibutilide group and from 447.7±39.4 to 484.8±61.4 msec (P<0.05)
in the amiodarone + ibutilide group. As shown in Fig. 2, although the QTc interval of the two
groups was prolonged following the application of the drug, the
extent of the prolongation was similar, and the QTc of each group
demonstrated no significant difference between the time points that
were close together. Furthermore, the QTc interval of the
amiodarone + ibutilide co-treatment group was identified to be
shorter than the QTc of the ibutilide alone group at 120 min
(P<0.05).
Complications and safety profile
There were no patients exhibiting frequent premature
ventricular contractions, non-sustained ventricular tachycardia,
sustained ventricular tachycardia or ventricular fibrillation in
the amiodarone + ibutilide co-treatment group. There were 13
patients exhibiting frequent premature ventricular contractions, 7
patients with non-sustained ventricular tachycardia and 3 patients
with sustained ventricular tachycardia and ventricular fibrillation
(the 3 patients underwent emergency electrical defibrillation
therapy for conversion of sinus rhythm) in the ibutilide alone
group. It was observed that the co-administration of amiodarone +
ibutilide was safer than the ibutilide alone with regard to the
risk of ventricular arrhythmia. In addition, 9 patients exhibited
sinus bradycardia in the amiodarone + ibutilide group and 5
patients exhibiting sinus bradycardia in the ibutilide group.
Long-term outcome
The patients of successful cardioversion were
personally contacted for an updated follow-up. After a median
follow-up period of 19.84±8.50 months, the result demonstrated that
the mean sinus rhythm maintenance time of the amiodarone +
ibutilide group was 4.36±2.44 months. Furthermore, the mean sinus
rhythm maintenance time of the ibutilide group was 2.34±1.75
months. The mean sinus rhythm maintenance time of the amiodarone +
ibutilide group was significantly higher than that of the ibutilide
group (P<0.01).
Discussion
For the refractory treatment of AF, AF patients are
managed with electrical vs. chemical cardioversion. At present, the
majority of patients with persistent AF of long duration are
treated with electrical direct current cardioversion, which is
associated with high success rates and reduced monitoring times.
However, electrical conversion requires general anesthesia and may
be associated with periprocedural complications. Thus, the
development of effective and safe therapeutic strategies to treat
AF is important (10,11). In the current study, the
pharmacological effects of a combination of amiodarone and
ibutilide on cardioversion of persistent AF were determined.
Ibutilide is administered for the acute
cardioversion of AF and atrial flutter. It is used as a first-line
drug in the treatment of recent-onset AF and atrial flutter. In
rapid onset (3–48 h), the cardioversion rate of atrial flutter with
ibutilide was 87%, and the cardioversion rate of AF with ibutilide
was 77% (12). However, the efficacy
of treatment of ibutilide in the cardioversion of persistent AF is
not as effective as the curative effect for acute AF. A previous
study indicated that the conversion rate of persistent AF
(duration, >30 days) with ibutilide was 48% (13). Furthermore, ibutilide may induce QT
interval prolongation and increase the risk of torsade de pointes,
as a result of prolonging the action potential duration (APD) by
increasing the slow inward sodium current and blocking the delayed
rectifier potassium current (14–16).
Amiodarone has a complex electrophysiological characteristic
(12,17). With long-term administration,
amiodarone markedly prolongs the ventricular action potential and
the QT interval (13); however, the
incidence of torsade de pointes is low (18,19).
Long-term amiodarone therapy is commonly used for the maintenance
of sinus rhythm for patients with recent-onset AF. Thus, the
conventional antiarrhythmic drugs, used for persistent AF of long
duration, have shown limited efficacy. In the current study, the
electrophysiological effects of amiodarone and ibutilide on the
atrium in patients with persistent AF were evaluated. A total of 48
patients were successfully converted to sinus rhythm; with 20
patients from the ibutilide treatment group (rate of cardioversion,
51.3%), and 28 patients from the ibutilide and amiodarone
co-treatment group (rate of cardioversion, 71.8%). The rate of
cardioversion was significantly different between the two groups
(P<0.05; Fig. 1).
The most serious proarrhythmic side effect of class
III agents is torsade de pointes. Class IA and class III
antiarrhythmic agents induced prolongation of APD and the QTc
interval, which are associated with an increased risk of torsade de
pointes. As shown in Fig. 2, the QTc
interval was significantly prolonged in the two groups, from
440.7±38.1 to 520.6±69.3 msec (P<0.05) in the ibutilide
treatment group and from 447.7±39.4 to 484.8±61.4 msec (P<0.05)
in the amiodarone + ibutilide co-treatment group. However, the QTc
interval of the co-treatment group was identified to be shorter
than the QTc of the ibutilide group at 120 min. In the current
study, there were 13 patients with frequent premature ventricular
contractions, 7 patients with non-sustained ventricular
tachycardia, and 3 patients with sustained ventricular tachycardia
and ventricular fibrillation in the ibutilide treatment group. The
incidence of sustained torsade de pointes was 10.1% (3/31
patients). This result was relatively consistent with previous
ibutilide studies. In a study of 180 patients who received
ibutilide treatment for cardioversion, the incidence of torsade de
pointes was reported to be up to 8.3% (20). There were no patients with frequent
premature ventricular contractions, non-sustained ventricular
tachycardia, or sustained ventricular tachycardia and ventricular
fibrillation in the amiodarone + ibutilide co-treatment group in
the present study. The low incidence of ventricular fibrillation
with amiodarone + ibutilide therapy may be multifactorial. Previous
studies indicate that the dispersion of repolarization was a
critical factor in the maintenance of torsade de pointes (13,18). The
ventricular myocardium normally displays heterogeneity of
refractoriness, with the M (or middle) cells displaying the longest
APD of the ventricular subtypes. Amiodarone prolongs the APD of all
ventricular cell subtype; however, it does not prolong the M-cell
APD. Thus, amiodarone may reduce the transmural dispersion of
repolarization (7,8). This may, in part, explain why
co-treatment with amiodarone + ibutilide is safer than treatment
with ibutilide alone in the risk of ventricular arrhythmia.
In conclusion co-treatment with amiodarone and
ibutilide for AF therapy was evaluated in detail during the present
study. A significantly increased efficacy and safety of combination
therapy was observed when compared with treatment of ibutilide
alone. Therefore, combination pharmacological therapy with
amiodarone + ibutilide may present as a useful adjunct to current
cardioversion protocols for AF, particularly in cases of persistent
AF.
Acknowledgements
The present study was supported by Science and
Technology Department of Heilongjiang Province (grant no.
GC12C305-6), Health and Family Planning Commission of the
Heilongjiang Province (grant no. 2016-002).
References
|
1
|
Waktare JE and Camm AJ: Atrial
fibrillation begets trouble. Heart. 77:393–394. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Sasaki N, Watanabe I, Kogawa R, Sonoda K,
Takahashi K, Okumura Y, Ohkubo K, Nakai T and Hirayama A: Effects
of intravenous amiodarone and ibutilide on action potential
duration and atrial conduction kinetics in patients with persistent
atrial fibrillation. Int Heart J. 55:244–248. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
European Heart Rhythm Association;
European Association for Cardio-Thoracic Surgery, ; Camm AJ,
Kirchof P, Lip GY, Schotten U, Savelieva I, Ernst S, van Gelder IC,
Al-Attar N, et al: Guidelines for the management of atrial
fibrillation: The task force for the management of atrial
fibrillation of the European society of cardiology (ESC). Eur Heart
J. 31:2369–2429. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Workman AJ, Smith GL and Rankin AC:
Mechanisms of termination and prevention of atrial fibrillation by
drug therapy. Pharmacol Ther. 131:221–241. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Vasić NR, Milenković BA, Pešut DP, Stević
RS and Jovanović DM: Drug induced lung disease-amiodarone in focus.
Med Pregl. 67:334–337. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Fadahunsi O and Krol R: Acute amiodarone
pulmonary toxicity following lung resection. Int J Biomed Sci.
10:217–220. 2014.PubMed/NCBI
|
|
7
|
Lafuente-Lafuente C, Mouly S,
Longás-Tejero MA, Mahé I and Bergmann JF: Antiarrhythmic drugs for
maintaining sinus rhythm after cardioversion of atrial
fibrillation: A systematic review of randomized controlled trials.
Arch Intern Med. 166:719–728. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Freemantle N, Lafuente-Lafuente C,
Mitchell S, Eckert L and Reynolds M: Mixed treatment comparison of
dronedarone, amiodarone, sotalol, flecainide, and propafenone, for
the management of atrial fibrillation. Europace. 13:329–345. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Camm J: Antiarrhythmic drugs for the
maintenance of sinus rhythm: Risks and benefits. Int J Cardiol.
155:362–371. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
de Paola AA, Figueiredo E, Sesso R, Veloso
HH and Nascimento LO: SOCES Investigators: Effectiveness and costs
of chemical versus electrical cardioversion of atrial fibrillation.
Int J Cardiol. 88:157–166. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Korantzopoulos P, Kolettis TM,
Papathanasiou A, Naka KK, Kolios P, Leontaridis I, Draganigos A,
Katsouras CS and Goudevenos JA: Propafenone added to ibutilide
increases conversion rates of persistent atrial fibrillation.
Heart. 92:631–634. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Kafkas NV, Patsilinakos SP, Mertzanos GA,
Papageorgiou KI, Chaveles JI, Dagadaki OK and Kelesidis KM:
Conversion efficacy of intravenous ibutilide compared with
intravenous amiodarone in patients with recent-onset atrial
fibrillation and atrial flutter. Int J Cardiol. 118:321–325. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Vos MA, Golitsyn SR, Stangl K, Ruda MY,
van Wijk LV, Harry JD, Perry KT, Touboul P, Steinbeck G and Wellens
HJ: Superiority of ibutilide (a new class III agent) over
DL-sotalol in converting atrial flutter and atrial fibrillation.
The Ibutilide/Sotalol Comparator Study Group. Heart. 79:568–575.
1998. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Fragakis N, Bikias A, Delithanasis I,
Konstantinidou M, Liakopoulos N, Kozirakis M and Katsaris G: Acute
beta-adrenoceptor blockade improves efficacy of ibutilide in
conversion of atrial fibrillation with a rapid ventricular rate.
Europace. 11:70–74. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Stambler BS, Wood MA, Ellenbogen KA, Perry
KT, Wakefield LK and VanderLugt JT: Efficacy and safety of repeated
intravenous doses of ibutilide for rapid conversion of atrial
flutter or fibrillation. Ibutilide Repeat Dose Study Investigators.
Circulation. 94:1613–1621. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Yang T, Snyders DJ and Roden DM:
Ibutilide, a methanesulfonanilide antiarrhythmic, is a potent
blocker of the rapidly activating delayed rectifier K+
current (IKr) in AT-1 cells. Concentration-, time-, voltage-, and
use-dependent effects. Circulation. 91:1799–1806. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Stambler BS, Beckman KJ, Kadish AH, Camm
JA, Ellenbogen KA, Perry KT and VanderLugt JT: Acute hemodynamic
effects of intravenous ibutilide in patients with or without
reduced left ventricular function. Am J Cardiol. 80:458–463. 1997.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Gill J, Heel RC and Fitton A: Amiodarone:
An overview of its pharmacological properties and review of its
therapeutic use in cardiac arrhythmias. Drugs. 43:69–110. 1992.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Mitchell LB, Wyse DG, Gillis AM and Duff
HJ: Electropharmacology of amiodarone therapy initiation. Time
courses of onset of electrophysiologic and antiarrhythmic effects.
Circulation. 80:34–42. 1989. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Stambler BS, Wood MA and Ellenbogen KA:
Antiarrhythmic actions of intravenous ibutilide compared with
procainamide during human atrial flutter and fibrillation:
Electrophysiological determinants of enhanced conversion efficacy.
Circulation. 96:4298–4306. 1997. View Article : Google Scholar : PubMed/NCBI
|