Introduction
Depression is a debilitating disorder with severe
health problems which pose a heavy economic burden to society
(1). At present, monoamine drugs
are the dominant therapeutic agent of choice for the treatment of
depression (2). However, currently
available antidepressant agents have severe drawbacks, such as low
rates of treatment response and delayed onset time (3,4). In
several studies, depression is considered as the disease that is
related to the high expression of proinflammatory cytokines, and
furthermore, attenuation of inflammation is suggested as one
possible mechanism explaining the action of antidepressant agents
(5–7). Collectively, the inflammatory
response system is likely to be implicated in the etiology and
treatment of depression.
Ketamine, an ionotropic glutamatergic
N-methyl-D-aspartic acid (NMDA) receptor antagonist, is widely used
in clinical anesthesia and pain treatment. Recent clinical studies
have provided evidence that sub-anesthetic doses of ketamine may
rapidly alleviate symptoms of depression, even for
treatment-resistant depression, with an identical therapeutic
effect (8,9). However, its underlying mechanisms
have yet to be fully elucidated.
A previous review summarized that ketamine has the
potential to modulate inflammation (10). It has been widely acknowledged that
ketamine has been recommended for use in the surgery of sepsis
patients due to its anti-inflammatory effects (11,12).
However, too little attention is presently focused on the
underlying mechanism with regard to whether inflammatory cytokines
are involved in the antidepressant effects of ketamine.
Thus, we propose a hypothesis that ketamine may
exert antidepressant effects via modulation of proinflammatory
cytokines. Based on this theory, we aimed to validate the
above-mentioned hypothesis. The present study was designed to
determine the levels of IL-1β and IL-6 in the rat prefrontal cortex
and hippocampus after ketamine administration during a forced
swimming test (FST).
Materials and methods
Animals and drugs
Twenty male Wistar rats weighing 180–300 g were
purchased from the Shanghai Animal Center (Shanghai, China). Five
rats were housed per cage with food and water available ad
libitum and maintained on a 12-h light/dark cycle (lights on at
07:00 am). Rats were randomly divided into 2 groups (each group,
n=10). Rats were intraperitoneally administered with saline or
ketamine at a dose of 10 mg/kg 30 min before the test session of
FST. Ketamine was obtained from the Gutian Pharmaceutical Company
(Fujian, China). The experimental procedures were approved by the
Institutional Animal Ethics Committee of Suzhou University (Suzhou,
China).
FST
FST was applied according to our previous study
(13) to evaluate the
antidepressant effects of ketamine. The test included two separate
sessions in a cylindrical tank (30-cm diameter, 60-cm height)
filled with water (22–23°C) to a 30-cm level in which rats were
unable to touch the bottom of the tank. The water was replaced
after each rat had completed one session. All procedures were
conducted between 9:00 am–15:00 pm. Rats first underwent a FST for
15 min (pre-test session). After 24 h, rats were placed in the
water again for 5 min (test session), and the immobility time was
recorded in seconds. Immobility was defined as the amount of time
that the rat remained floating in the water without struggling and
made only those movements necessary to keep its head above the
water.
Testing IL-1β levels
Following FST, rats were immediately sacrificed and
the prefrontal cortex and hippocampus were harvested for
determination. In brief, the prefrontal cortex and hippocampus were
separately washed with ice-cold phosphate-buffered solution (PBS)
and scraped in lysis buffer. The insoluble material was removed by
centrifugation at 12,000 rpm for 20 min. Protein content was
measured according to the bicinchoninic acid (BCA) method.
Non-specific binding was blocked for 1 h at 37°C in TBS containing
non-fat dried milk. The membrane was then incubated with primary
antibodies against IL-1β (1:1000) and β-actin served as the
control. Membranes were then incubated in the appropriate
HRP-conjugated secondary antibodies (1:20000).
Testing IL-6 levels
IL-6 levels in the prefrontal cortex and hippocampus
were measured by sandwich-ELISA of relevant primary antibodies
according to the manufacturer’s instructions (Chemicon, Temecula,
CA, USA). Briefly, rat prefrontal cortex and hippocampus were
homogenized in PBS with 1 mM phenylmethylsulfonyl fluoride (PMSF)
and 1 mM ethylene glycol tetraacetic acid (EGTA). Microtiter plates
(48-well flat-bottom) were coated for 24 h with the samples diluted
1:2 in sample diluent and standard curves ranged between 7.8 and
500 pg/ml. The plates were then washed four times with sample
diluent and a monoclonal rabbit antibody diluted 1:1000 in sample
diluent was added to each well. The plates were then incubated for
3 h at room temperature. After washing, a peroxidase-conjugated
anti-rabbit antibody (diluted 1:1000) was added to each well and
incubated at room temperature for 1 h. After addition of
streptavidin-enzyme, substrate and stop solution, the amount of
IL-6 was determined by absorbance at 450 nm. The standard curve
demonstrates a direct correlation between optical density (OD) and
the concentration of IL-6. Total protein was measured by Lowry’s
method using bovine serum albumin as a standard.
Statistical analysis
Data are presented as mean ± standard deviation
(SD). Statistical analyses were performed by one-way analysis of
variance (ANOVA). These statistical analyses were conducted by
Statistical Product for Social Sciences (SPSS version 17.0).
P<0.05 was considered to indicate a statistically significant
result.
Results
Effects of ketamine on the immobility
time of rats during FST
Compared with saline administration, the
administration of ketamine significantly decreased the immobility
time of rats during FST (P<0.05; Fig. 1).
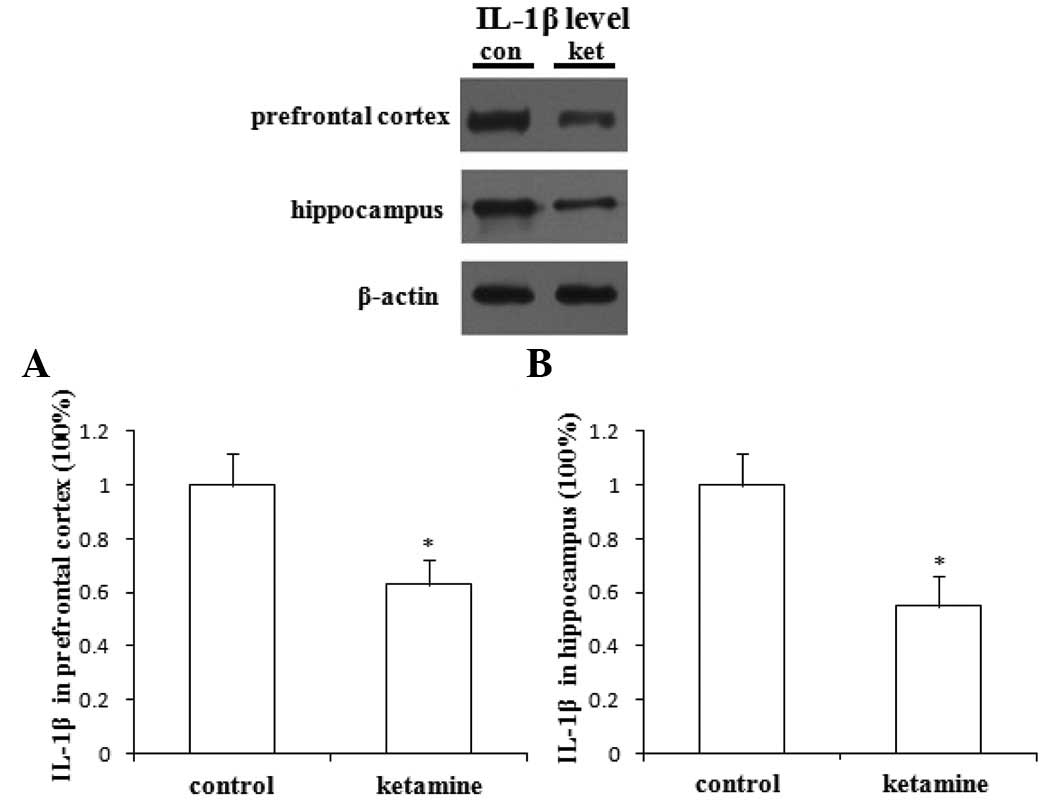
Effects of ketamine on the expression of
IL-1β in rat prefrontal cortex and hippocampus
Compared with saline administration, the
administration of ketamine significantly decreased the expression
of IL-1β in rat prefrontal cortex (Fig. 2A) and hippocampus (Fig. 2B; P<0.05).
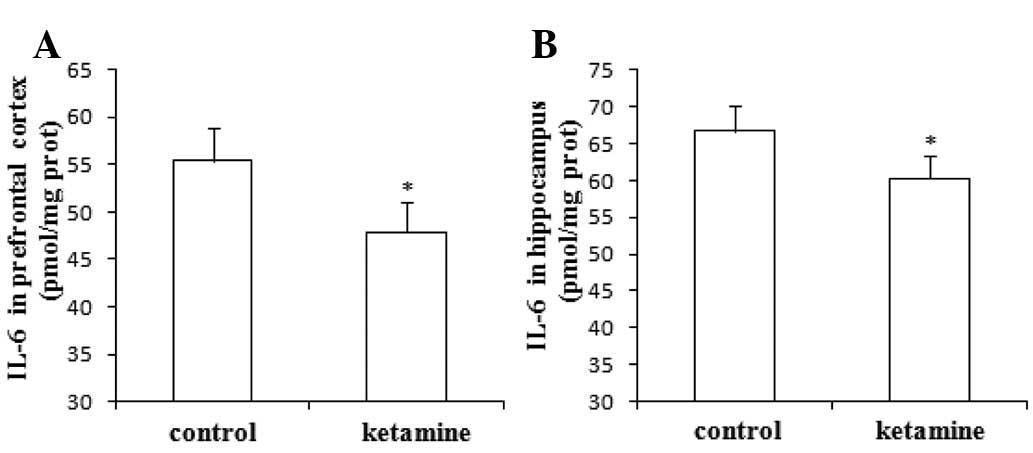
Effects of ketamine on the expression of
IL-6 in rat prefrontal cortex and hippocampus
Compared with saline administration, the
administration of ketamine significantly decreased the expression
of IL-6 in rat prefrontal cortex (Fig.
3A) and hippocampus (Fig. 3B;
P<0.05).
Discussion
In the present study, we demonstrated that ketamine
significantly decreased the immobility time of rats in FST, and
there was a significantly lower expression of IL-1β and IL-6 in rat
prefrontal cortex and hippocampus following ketamine
administration.
Recent animal and clinical studies have indicated
that the administration of ketamine at sub-anesthetic doses has
fast-acting and robust antidepressant effects (8,9), and
it has been shown that ketamine, widely used as an anesthetic
agent, demonstrates unique effects for the treatment of depression.
In the present study, the administration of ketamine at a dose of
10 mg/kg significantly decreased the immobility time of rats
receiving FST. This result is consistent with previous studies and
confirmed ketamine’s antidepressant effects.
It has previously been reported that ketamine is
recommended for use in the anesthesia of patients with sepsis due
to its effects of stimulating sympathetic nerves, maintaining
vasoconstriction and maintaining circulation stability (14,15).
Taniguchi and Yamamoto (16) have
indicated that ketamine may inhibit the sepsis-induced inflammatory
response in a rat model and attenuate the fall of blood pressure.
Furthermore, a previous study conducted by Sun et al
(17) has revealed that ketamine’s
anti-inflammatory effects may be associated with the changes in the
expression of nuclear factor-κB and tumor necrosis factor-α.
Collectively, these findings suggest that ketamine has significant
anti-inflammatory effects.
At present, the treatment of depression is mainly
dependent on conventional antidepressant agents. A large body of
evidence suggests that the peripheral serum proinflammatory
cytokine levels of patients with depression are significantly
higher than normal levels, and the increased levels are
proportional to the severity of depression (18,19).
In addition, it has been demonstrated that the proinflammatory
cytokine levels in the peripheral blood of patients with depression
gradually tend to become normal following treatment with
antidepressant agents (20,21).
In the preliminary study, we observed a lower expression of IL-1β
and IL-6 in rat prefrontal cortex and hippocampus after ketamine
administration, and the results validated our above-mentioned
hypothesis.
Mounting studies reveal that both IL-1β and IL-6 are
important in the etiology and pathophysiology of depression
(22,23). In clinical trials, elevated levels
of IL-1β and IL-6 have been observed in the peripheral blood of
depressed patients (23,24). Besides, in experimental animals,
administration of IL-1β has produced depressive-like symptoms which
were attenuated by treatment with antidepressants (25,26).
Therefore, we concluded that the onset of antidepressants may be
accompanied by the inhibition of IL-1β and IL-6. In the present
study, the results demonstrated that ketamine exerts an
antidepressant effect that is associated with the downregulation of
IL-1β and Il-6 levels, which was consistent with the
above-mentioned conclusion.
In conclusion, ketamine possesses properties that
exert antidepressant effects, which have been confirmed in the
present study, and its underlying mechanism is potentially
associated with the inhibition of IL-1β and IL-6 expression in rat
prefrontal cortex and hippocampus. However, a great limitation of
the present study is that we did not test the levels of
anti-inflammatory cytokines, which future studies are required to
investigate further.
Acknowledgements
This study was supported by grants
from the National Natural Science Foundation of China (Grant No.
30872424).
References
|
1
|
Kessler RC, Berglund P, Demler O, et al:
The epidemiology of major depressive disorder: results from the
National Comorbidity Survey Replication (NCS-R). JAMA.
289:3095–3105. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Berton O and Nestler EJ: New approaches to
antidepressant drug discovery: beyond monoamines. Nat Rev Neurosci.
7:137–151. 2006. View
Article : Google Scholar : PubMed/NCBI
|
|
3
|
Uppal A, Singh A, Gahtori P, Ghosh SK and
Ahmad MZ: Antidepressants: current strategies and future
opportunities. Curr Pharm Des. 16:4243–4253. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Mitchell AJ: Two-week delay in onset of
action of antidepressants: new evidence. Br J Psychiatry.
188:105–106. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Wright CE, Strike PC, Brydon L and Steptoe
A: Acute inflammation and negative mood: mediation by cytokine
activation. Brain Behav Immun. 19:345–350. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Dantzer R: Cytokine-induced sickness
behavior: mechanisms and implications. Ann NY Acad Sci.
933:222–234. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Pollak Y and Yirmiya R: Cytokine-induced
changes in mood and behaviour: implications for ‘depression due to
a general medical condition’, immunotherapy and antidepressive
treatment. Int J Neuropsychopharmacol. 5:389–399. 2002.
|
|
8
|
Skolnick P, Popik P and Trullas R:
Glutamate-based antidepressants: 20 years on. Trends Pharmacol Sci.
30:563–569. 2009.PubMed/NCBI
|
|
9
|
Machado-Vieira R, Salvadore G,
Diazgranados N and Zarate CA Jr: Ketamine and the next generation
of antidepressants with a rapid onset of action. Pharmacol Ther.
123:143–150. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Dale O, Somogyi AA, Li Y, Sullivan T and
Shavit Y: Does intra-operative ketamine attenuate inflammatory
reactivity following surgery? A systematic review and
meta-analysis. Anesth Analg. 115:934–943. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Ward JL, Harting MT, Cox CS Jr and Mercer
DW: Effects of ketamine on endotoxin and traumatic brain injury
induced cytokine production in the rat. J Trauma. 70:1471–1479.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Takahashi T, Kinoshita M, Shono S, et al:
The effect of ketamine anesthesia on the immune function of mice
with postoperative septicemia. Anesth Analg. 111:1051–1058.
2010.PubMed/NCBI
|
|
13
|
Yang C, Hu YM, Zhou ZQ, Zhang GF and Yang
JJ: Acute administration of ketamine in rats increases hippocampal
BDNF and mTOR levels during forced swimming test. Ups J Med Sci.
Sep 13–2012.(Epub ahead of print).
|
|
14
|
Busch CJ, Spöhr FA, Motsch J, Gebhard MM,
Martin EO and Weimann J: Effects of ketamine on hypoxic pulmonary
vasoconstriction in the isolated perfused lungs of endotoxaemic
mice. Eur J Anaesthesiol. 27:61–66. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Nakayama M and Murray PA: Ketamine
preserves and propofol potentiates hypoxic pulmonary
vasoconstriction compared with the conscious state in chronically
instrumented dogs. Anesthesiology. 91:760–771. 1999. View Article : Google Scholar
|
|
16
|
Taniguchi T and Yamamoto K:
Anti-inflammatory effects of intravenous anesthetics on
endotoxemia. Mini Rev Med Chem. 5:241–245. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Sun J, Zhou ZQ, Lv R, Li WY and Xu JG:
Ketamine inhibits LPS-induced calcium elevation and NF-kappa B
activation in monocytes. Inflamm Res. 53:304–308. 2004.PubMed/NCBI
|
|
18
|
Raedler TJ: Inflammatory mechanisms in
major depressive disorder. Curr Opin Psychiatry. 24:519–525.
2011.PubMed/NCBI
|
|
19
|
Hannestad J, DellaGioia N and Bloch M: The
effect of antidepressant medication treatment on serum levels of
inflammatory cytokines: a meta-analysis. Neuropsychopharmacology.
36:2452–2459. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Catena-Dell’Osso M, Bellantuono C, Consoli
G, Baroni S, Rotella F and Marazziti D: Inflammatory and
neurodegenerative pathways in depression: a new avenue for
antidepressant development? Curr Med Chem. 18:245–255.
2011.PubMed/NCBI
|
|
21
|
Song C and Wang H: Cytokines mediated
inflammation and decreased neurogenesis in animal models of
depression. Prog Neuropsychopharmacol Biol Psychiatry. 35:760–768.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Owen BM, Eccleston D, Ferrier IN and Young
AH: Raised levels of plasma interleukin-1beta in major and
postviral depression. Acta Psychiatr Scand. 103:226–228. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Piletz JE, Halaris A, Iqbal O, et al:
Pro-inflammatory biomakers in depression: treatment with
venlafaxine. World J Biol Psychiatry. 10:313–323. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Brambilla F, Monteleone P and Maj M:
Interleukin-1beta and tumor necrosis factor-alpha in children with
major depressive disorder or dysthymia. J Affect Disord.
78:273–277. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Castanon N, Bluthe RM and Dantzer R:
Chronic treatment with the atypical antidepressant tianeptine
attenuates sickness behavior induced by peripheral but not central
lipopolysaccharide and interleukin-1beta in the rat.
Psychopharmacology (Berl). 154:50–60. 2001. View Article : Google Scholar
|
|
26
|
Merali Z, Brennan K, Brau P and Anisman H:
Dissociating anorexia and anhedonia elicited by interleukin-1beta:
anti-depressant and gender effects on responding for ‘free chow’
and ‘earned’ sucrose intake. Psychopharmacology (Berl).
165:413–418. 2003.PubMed/NCBI
|