Introduction
Pulmonary large cell neuroendocrine (NE) carcinoma
(LCNEC) is a rare type of pulmonary tumor, accounting for 2–3% of
lung cancers in surgical series. Subsequent to the initial
description of LCNEC by Travis et al in 1991, increasing
evidence has indicated that LCNEC shares numerous morphological,
immunohistochemical and molecular characteristics with small cell
lung cancer (SCLC), as well as treatment strategies and a poor
prognosis (1). The optimal treatment
regime for patients with LCNEC has yet to be established. Recently,
the use of epidermal growth factor receptor-tyrosine kinase
inhibitors (EGFR-TKIs) has been demonstrated to be an effective
therapeutic strategy for patients with non-SCLC (NSCLC),
particularly for those with EGFR mutations (2,3). However,
EGFR mutations typically occur in patients with adenocarcinoma and
investigations of EGFR mutations in LCNEC are limited.
To date, only one case of LCNEC with an activating
EGFR gene mutation and a good response to EGFR-TKI has been
described in the literature (4). The
present study describes a case of LCNEC harboring an activating
EGFR mutation that was treated with icotinib and exhibited a marked
response. The current report highlights the possibility of
identifying EGFR mutations in LCNEC and the potential of EGFR-TKIs
in the treatment of patients with LCNEC harboring these EGFR gene
mutations. Written informed consent was obtained from the patient's
family.
Case report
In February 2013, an 84-year-old male with a smoking
history of 20 cigarettes a day for 40 years presented to the First
Affiliated Hospital of the College of Medicine, Zhejiang University
(Hangzhou, China) with a 1-month history of a non-productive cough
and right-sided back pain. The patient also complained of fatigue
and weight loss of 10 lb over the most recent month. The patient
exhibited a poor Eastern Cooperative Oncology Group performance
status of 3 (5), a left
supraclavicular lymph node was palpably enlarged upon initial
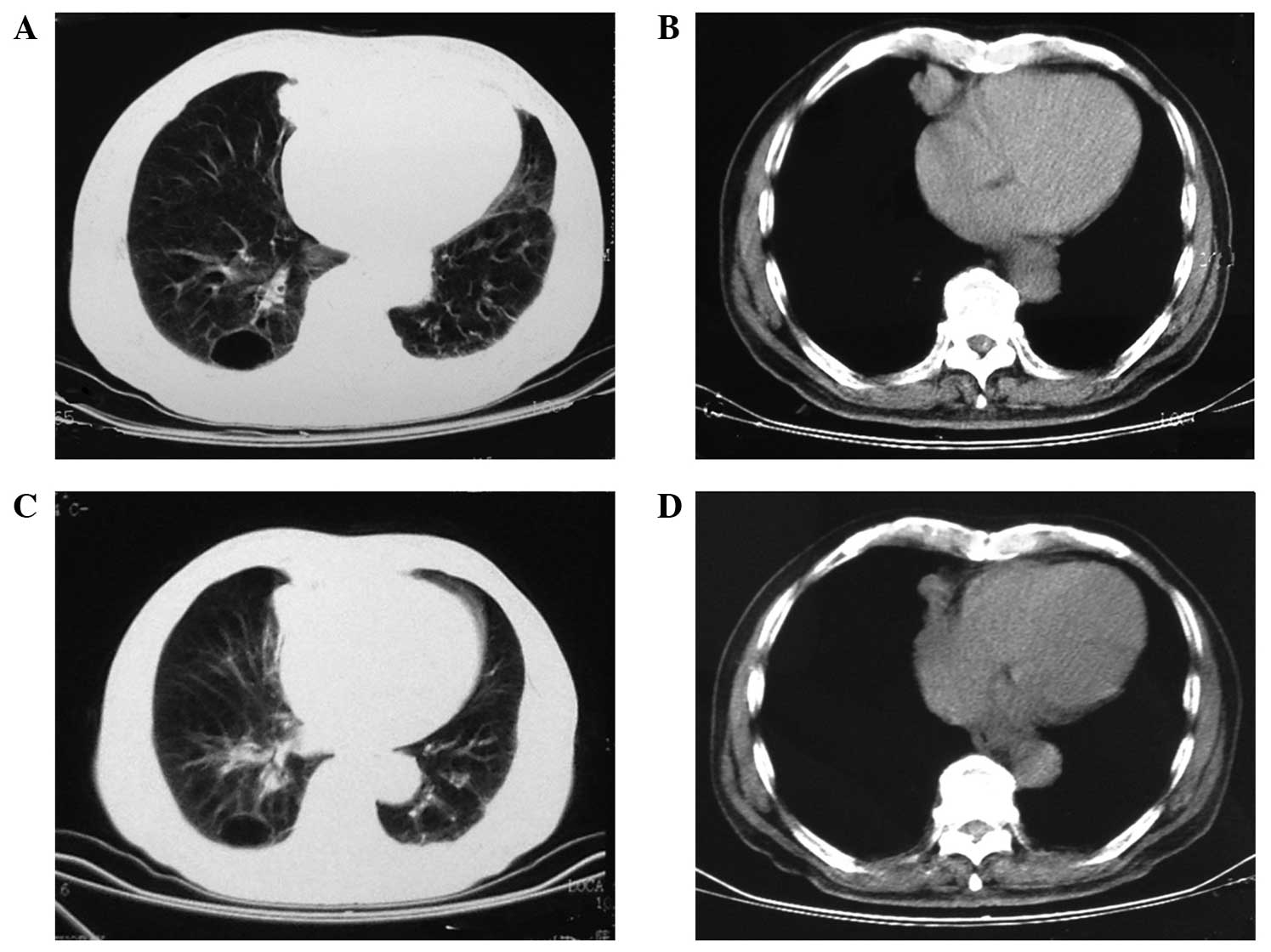
physical examination and chest computed tomography (CT) detected an
irregular mass in the middle lobe of the right lung (Fig. 1A and B). Initial blood tests revealed
an elevated carcinoembryonic antigen (CEA) concentration of 106.1
ng/ml (standard range, 0–5 ng/ml) and an elevated neuron specific
enolase (NSE) concentration of 82.1 ng/ml (standard range, 0–15
ng/ml). Furthermore, right middle lobe bronchial brushing during
fiberoptic bronchoscopy identified poorly-differentiated cancer
cells. A biopsy of the left supraclavicular lymph node was
histologically analyzed and the following NSCLC cytological
features were identified: Large cell size, low nuclear/cytoplasmic
ratio, NE morphology with organoid nesting and a high mitotic rate
of >10 mitoses per 2 mm2. These results were
consistent with a diagnosis of metastatic LCNEC (Fig. 2). In agreement with this diagnosis, an
NE phenotype was demonstrated by positive cytoplasmic
immunostaining for synaptophysin (Fig.
2C) and chromogranin A (Fig. 2D).
Additionally, formalin-fixed paraffin-embedded tissues with a
thickness of 5 µm were used to determine the presence of EGFR
mutations. Genomic DNA was isolated using the QIAamp® DNA Mini kit
(Qiagen, Hilden, Germany), according to the manufacturer's
instructions. Exon sequences for EGFR (exons 18, 19, 20 and 21)
were amplified with specific primers by polymerase chain reaction
and an activating EGFR mutation (exon 19 deletion) was
detected.
Following diagnosis, icotinib was orally
administered at a dose of 125 mg three times per day and continued
for 8 months. After 1 week of treatment, the patient reported a
significant reduction in coughing and right-sided back pain. Chest
CT scans performed 1 month after treatment with icotinib commenced
revealed partial remission (Fig. 1C and
D). Furthermore, CEA and NSE concentrations were markedly
reduced to 65.1 and 22.2 ng/ml, respectively, after 4 months of
icotinib treatment. This marked response to icotinib lasted for 8
months. However, after 8 months of treatment, the patient reported
the reappearance of cough and right-sided back pain, and decided to
discontinue self-administration of icotinib. The patient did not
return to the First Affiliated Hospital of the College of Medicine
for further examination or treatment.
Discussion
LCNEC is a subtype of large cell carcinoma (LCC).
Due to its NE differentiation, LCNEC is also classified as a
pulmonary NE tumor. According to the 1999 and 2004 World Health
Organization classifications (6,7), there are
four major categories of NE phenotype in LCCs: i) LCNEC (LCC with
NE features upon light microscopy, immunohistochemistry and/or
electron microscopy); ii) LCC with NE morphology (LCC with NE
morphology, but no NE differentiation upon electron microscopy or
immunohistochemistry); iii) LCC with NE differentiation (LCC with
no NE morphology, but with NE differentiation upon
immunohistochemistry or electron microscopy); and iv) classic LCC
(LCC that appears to lack NE morphology and NE
differentiation).
As the population of patients with LCNEC is small,
it has been difficult to conduct randomized controlled trials to
establish a consensus on the optimal management of LCNEC. LCNEC is
more similar to SCLC than NSCLC with respect to its clinical
characteristics, including a preponderance of men and smokers, as
well as the effectiveness of palliative chemotherapeutic regimens
(8). The majority of previous studies
have reported that patients with LCNEC exhibit poorer survival than
is expected for patients with stage-matched NSCLC, approaching the
unfavorable outcome of patients with SCLC. Overall, previous study
series have reported LCNEC 5-year survival rates of 13–57% in
surgically-treated patients (9,10). Certain
retrospective reviews of LCNEC patients undergoing surgery have
indicated that surgical resection tends to improve overall
survival. For such resec Table patients, it has been demonstrated
that perioperative adjuvant chemotherapy favors survival compared
with surgery alone (5,10–12). With
respect to chemotherapeutic agents, the cisplatin-VP-16 doublet
regime has been recommended, similar to the recommendation for
patients with SCLC. This treatment strategy demonstrated
satisfactory results in terms of overall survival and
recurrence-free survival (11). The
majority of previous studies focused on surgically-treated cases
due to the difficulty in obtaining a pre-operative pathological
diagnosis, therefore, only a small number of studies have evaluated
the treatment of advanced LCNEC thus far, including the efficacy of
systemic chemotherapy (8,13). The number of patients analyzed in
these studies, however, was too small to draw meaningful conclusion
from.
EGFR-TKI therapy has been the primary treatment
strategy for patients with EGFR-mutant NSCLC, particularly for
patients with lung adenocarcinoma, non-smokers and Asian patients
(2,3).
However, due to the rarity of patients with LCNEC, our
understanding of EGFR mutations in these patients is limited.
Although cases of LCNEC harboring EGFR gene mutations have been
sporadically reported since 2011, only one case of LCNEC case
treated with EGFR-TKI has been reported. De Pas et al
reported the case of a non-smoking, 66-year-old female with an exon
19 deletion in the EGFR gene who exhibited a long-lasting response
to gefitinib as first-line therapy (4). Similarly, the present study reports the
case of a heavy smoker with an activating EGFR exon 19 deletion
mutation who exhibited a marked long-lasting response to EGFR-TKI
therapy. These two cases of LCNEC with activating EGFR mutations
responded well to EGFR-TKI treatment, indicating that mutational
analysis should be encouraged to improve treatment selection for
patients with LCNEC patients. Whether EGFR mutation predominantly
occurs in non-smoking women or Asian patients with LCNEC, similar
to lung adenocarcinoma, remains unknown due to the rarity of such
cases.
The genomic alterations and mechanisms of LCNEC are
largely unknown. Yanagisawa et al (14) and Popat et al (15) reported two cases of refractory lung
adenocarcinoma with EGFR mutations that exhibited transformation
from adenocarcinoma to LCNEC following long-term gefitinib
treatment or erlotinib plus chemotherapy treatment, respectively.
This transformation to LCNEC retained the original EGFR mutation,
indicating that it may be a potential EGFR-TKI resistance
mechanism.
Identifying the potential molecular targets for
LCNEC therapy is imperative to improve the prognosis of patients
with LCNEC. A number of studies have analyzed the expression and
mutation of various genes in LCNEC patients. For example, Rossi
et al (16) investigated 83
patients with pure pulmonary LCNEC and revealed that LCNEC samples
strongly expressed the following receptor tyrosine kinases (RTKs):
KIT expression was identified in 62.7% of patients,
platelet-derived growth factor receptor (PDGFR)α in 60.2% of
patients, PDGFRβ in 81.9% of patients and Met in 47% of patients.
However, no mutations were detected in the exons encoding the
relevant juxtamembrane domains. Iyoda et al (17) analyzed c-KIT, human epidermal growth
factor receptor type 2 (HER2) and vascular endothelial growth
factor (VEGF) expression by immunohistochemical analysis. Gene
mutations in EGFR, HER-2 and c-KIT were identified in 13 resected
LCNEC samples and compared with the expression in lung
adenocarcinoma. LCNEC exhibited a higher rate of c-KIT, HER2 and
VEGF immunohistochemical expression. Only a single EGFR mutation
(exon 18) was found in the LCNEC group. These data indicate a
potential role for RTK-, VEGF-, c-KIT- and HER2-targeted agents in
LCNEC treatment.
In conclusion, the current case highlights the
possibility of identifying EGFR mutations in LCNEC cases and
indicates that EGFR-TKIs may be an alternative treatment strategy
for patients with LCNEC harboring activating EGFR mutations.
Understanding the potential molecular targets in LCNEC is critical
for investigating novel and effective treatment strategies for
LCNEC. Prospective clinical studies on larger series of patients
with LCNEC are required to confirm the significance of EGFR gene
mutations and the role of EGFR-TKI in the treatment of LCNEC with
these mutations.
References
|
1
|
Travis WD, Linnoila RI, Tsokos MG,
Hitchcock CL, Cutler GB Jr, Nieman L, Chrousos G, Pass H and
Doppman J: Neuroendocrine tumors of the lung with proposed criteria
for large-cell neuroendocrine carcinoma. An ultrastructural,
immunohistochemical, and flow cytometric study of 35 cases. Am J
Surg Pathol. 15:529–553. 1991. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Rosell R1, Carcereny E, Gervais R,
Vergnenegre A, Massuti B, Felip E, Palmero R, Garcia-Gomez R,
Pallares C, Sanchez JM, et al: Spanish Lung Cancer Group in
collaboration with Groupe Français de Pneumo-Cancérologie and
Associazione Italiana Oncologia Toracica: Erlotinib versus standard
chemotherapy as first-line treatment for European patients with
advanced EGFR mutation-positive non-small-cell lung cancer
(EURTAC): A multicentre, open-label, randomised phase 3 trial.
Lancet Oncol. 13:239–426. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Mok TS, Wu YL, Thongprasert S, Yang CH,
Chu DT, Saijo N, et al: Gefitinib or carboplatin-paclitaxel in
pulmonary adenocarcinoma. N Engl J Med. 361:947–957. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
De Pas TM, Giovannini M, Manzotti M,
Trifirò G, Toffalorio F, Catania C, Spaggiari L, Labianca R and
Barberis M: Large-cell neuroendocrine carcinoma of the lung
harboring EGFR mutation and responding to gefitinib. J Clin Oncol.
29:e819–e822. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Travis WD: Advances in neuroendocrine lung
tumors. Ann Oncol. 21:(Sul 7). vii65–vii71. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Travis WD, Colby TV, Corrin B, et al:
Histological Typing of Lung and Pleural Tumors. Springer-Verlag;
Berlin: 1999, View Article : Google Scholar
|
|
7
|
Travis WD, Brambilla E, Müller-Hermelink
HK, et al: Pathology and GeneticsTumours of the Lung, Pleura,
Thymus and Heart. IARC Press; Lyon: 2004
|
|
8
|
Sun JM, Ahn MJ, Ahn JS, Um SW, Kim H, Kim
HK, et al: Chemotherapy for pulmonary large cell neuroendocrine
carcinoma: Similar to that for small cell lung cancer or non-small
cell lung cancer? Lung Cancer. 77:365–370. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Takei H, Asamura H, Maeshima A, Suzuki K,
Kondo H, Niki T, Yamada T, Tsuchiya R and Matsuno Y: Large cell
neuroendocrine carcinoma of the lung: A clinicopathologic study of
eighty-seven cases. J Thorac Cardiovasc Surg. 124:285–292. 2002.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Fournel L, Falcoz PE, Alifano M,
Charpentier MC, Boudaya MS, Magdeleinat P, Damotte D and Régnard
JF: Surgical management of pulmonary large cell neuroendocrine
carcinomas: A 10-year experience. Eur J Cardiothorac Surg.
43:111–114. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Abedallaa N, Tremblay L, Baey C, Fabre D,
Planchard D, Pignon JP, Guigay J, Pechoux CL, Soria JC, de
Montpreville VT, et al: Effect of chemotherapy in patients with
resected small-cell or large cell neuroendocrine carcinoma. J
Thorac Oncol. 7:1179–1183. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Kozuki T, Fujimoto N, Ueoka H, Kiura K,
Fujiwara K, Shiomi K, Mizobuchi K, Tabata M, Hamazaki S and
Tanimoto M: Complexity in the treatment of pulmonary large cell
neuroendocrine carcinoma. J Cancer Res Clin Oncol. 131:147–151.
2005. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Igawa S, Watanabe R, Ito I, Murakami H,
Takahashi T, Nakamura Y, Tsuya A, Kaira K, Naito T, Endo M, et al:
Comparison of chemotherapy for unresectable pulmonary high-grade
non-small cell neuroendocrine carcinoma and small-cell lung cancer.
Lung Cancer. 68:438–445. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Yanagisawa S, Morikawa N, Kimura Y, Nagano
Y, Murakami K and Tabata T: Large-cell neuroendocrine carcinoma
with epidermal growth factor receptor mutation: Possible
transformation of lung adenocarcinoma. Respirology. 17:1275–1277.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Popat S, Wotherspoon A, Nutting CM,
Gonzalez D, Nicholson AG and O'Brien M: Transformation to ‘high
grade’ neuroendocrine carcinoma as an acquired drug resistance
mechanism in EGFR-mutant lung adenocarcinoma. Lung Cancer. 80:1–4.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Rossi G, Cavazza A, Marchioni A, Longo L,
Migaldi M, Sartori G, Bigiani N, Schirosi L, Casali C, Morandi U,
et al: Role of chemotherapy and the receptor tyrosine kinases KIT,
PDGFRalpha, PDGFRbeta, and Met in large-cell neuroendocrine
carcinoma of the lung. J Clin Oncol. 23:8774–8785. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Iyoda A, Travis WD, Sarkaria IS, Jiang SX,
Amano H, Sato Y, Saegusa M, Rusch VW and Satoh Y: Expression
profiling and identification of potential molecular targets for
therapy in pulmonary large-cell neuroendocrine carcinoma. Exp Ther
Med. 2:1041–1045. 2011.PubMed/NCBI
|