Introduction
Cancers of the esophagus are placed among the most
common malignancies worldwide, being the eighth leading cause of
cancer related deaths (1). Esophageal
squamous cell cancer (ESCC) is a dominant histological type of
esophageal malignancies (1,2). Previously, there has been growing
interest in investigating the host inflammatory response to tumors,
and systemic inflammatory responses reflect the stimulation of
angiogenesis, DNA damage and tumor invasion caused by the
overproduction of cytokines (3–5). Thus, the
prognostic value of inflammation-based prognostic scores, such as
the Glasgow Prognostic Score (GPS) and the platelet-to-lymphocyte
ratio (6,7), has been studied. In addition, increasing
evidence has indicated that the neutrophil-to-lymphocyte ratio
(NLR) may be an effective prognostic indicator in various types of
malignant diseases (8–18).
ESCC is characterized by profound immune dysfunction
thought to be caused by cytokine production originating from tumor
cells and host immune competent cells (19–21). In
cancer patients, lymphopenia is the surrogate of impaired
cell-mediated immunity, whereas neutrophilia is a response to
systemic inflammation. NLR is considered to be a marker of general
immune responses to various stress stimuli. It correlates with the
severity of clinical progress in severely ill patients in the
intensive care unit and emerging evidence suggests that it may have
prognostic value in patients with solid tumors (22–24).
Because >60% of newly diagnosed ESCC patients
present either locally advanced or metastatic disease, surgical
resection is not applied in these patients. For these patients, a
chemoradiation therapy (CRT)-based multidisciplinary treatment may
be the only approach to achieve cure instead of an esophagectomy
(1,2,25). Surgical
resection has constituted the primary treatment option in the
treatment of esophageal cancer. Despite advances in surgical
methodologies, long-term survival following surgery alone for
advanced esophageal cancer has remained poor. The implementation of
perioperative chemotherapy has improved survival rates. The most
commonly applied regimen for CRT and neoadjuvant chemotherapy is
the combination of cisplatin and 5-fluorouracil (FP) (25–27).
Currently, it is widely accepted that inflammatory
cells, which are present in the tumor microenvironment, and the
tumor immune response, which is activated by ionizing radiation,
significantly affect tumor development (28–31). This
tumor-generated inflammatory response may result in an increased
propensity for apoptosis, angiogenesis and DNA damage by
upregulating cytokines and inflammatory mediators.
Cancer-induced cachexia, a complex metabolic
syndrome associated with underlying illness, is another significant
problem in cancer treatment and care as it is associated with poor
responses to chemotherapy, nutritional impairment and immune
suppression (32,33). The authors previously reported that
malnutrition or hypoalbuminemia correlates well with immune
suppression, systemic inflammation and suppression of cell-mediated
immunity (34–38). Systemic inflammation may underlie these
conditions, which are prominent in patients with advanced cancer.
Thus, the relationship between the NLR and nutritional status or
immune function was also assessed in the current study.
Materials and methods
Study population
The authors enrolled 260 patients with locally
advanced and metastatic ESCC including 110 patients treated with
CRT and 150 with FP, were treated between May 2013 and May 2016 at
Saitama Medical University International Medical Center (Hidaka,
China). In patients with disturbance of oral nutrition, CRT was
mainly applied. Patient characteristics are listed in Table I. The study was approved by the
Institutional Review Board of Saitama Medical University
International Medical Center (Hidaka, China). All of the patients
provided written informed consent. Patient age ranged from 41 to 79
years (median, 65.3 years) in the CRT group and 40 to 78 years
(median, 63.6 years) in the FP group, and Eastern Cooperative Study
Group PS was 0 or 1. Peripheral blood were obtained before any
treatments, and NLR was defined as follows: Percentage of
neutrophils in white blood cells (WBCs)/percentage of lymphocytes
in WBCs or peripheral neutrophil count/peripheral lymphocyte count.
To assess the cell-mediated response, phytohemagglutinin was used
to stimulate lymphocyte proliferation, followed by a lymphocyte
proliferation assay in which proliferation was measured by
3H-thymidine incorporation; the proliferative response was
expressed as the stimulation index (SI). The serum concentrations
of prealbumin (PA) and retinol-binding protein (RBP), rapid
turnover proteins, were measured as nutritional parameters by
immunoturbidimetry and latex flocculation turbidimetry,
respectively, and serum levels of C-reactive protein (CRP) were
measured by latex flocculation turbidimetry as an indicator of
inflammation. The patients of CRT group and FP group were divided
into two groups with 3.0 of NLR. CRT patients included 57 with a
high NLR and 53 with a low NLR and FP patients did 61 with a high
NLR and 89 with a low NLR (Table
I).
 | Table I.Patient characteristics. |
Table I.
Patient characteristics.
| Characteristics | CRT | FP |
|---|
| Patients (n) | 110 | 150 |
| Age | 65.3 (41–79) | 63.6 (40–78) |
| NLR>3 | 57 | 61 |
| NLR≤3 | 53 | 89 |
Chemotherapy regimen
For CRT treatment, all radiation treatments were
delivered as either 3D-CRT or intensity-modulated radiation therapy
with standard fractionation (i.e., 1.8/2.0 Gy fractions once daily
for 5 days/week). Radiation was delivered by high-energy (6 or 15
MV) linear accelerators. Patients were treated with a total dose of
50–64 Gy administered over 25–32 fractions. Chemotherapy began on
day 1 concurrent with the initial radiation treatments, and the
regimens included two cycles of 5-fluorouracil and cisplatin.
5-fluorouracil (700 mg/m2) was administered
intravenously (i.v.) on days 1–3, and cisplatin (25
mg/m2) was administered by i.v. infusion in 500 ml
either normal saline or dextrose on days 1–3. For FP treatment, two
cycles of cisplatin and 5-fluorouracil (5-FU), which consisted of
80 mg/m2 cisplatin administered on days 1 and 29 and 800
mg/m2/24 h 5-FU administered on days 1–3 and days 29–31.
The responses were evaluated according to the Response Evaluation
Criteria in Solid Tumors (RECIST) version 1.0 (39) following two cycles of treatment. The
patients who responded to therapy received surgical resection and
the same chemotherapy regimen again, and those who did not respond
to treatment received docetaxel as second-line treatment.
Statistical analysis
The significance among parameters including NLR was
analyzed by the χ2 test and Student's t-test. The
strength and significance of correlations were assessed by
Spearman's rank correlation coefficient. Among the patients entered
in the study, 104 patients with CRT and 145 patients with FP were
available for the analysis of survival. The survival curves of
patients who received CRT or FP were estimated using the
Kaplan-Meier method, and the log-rank test were used to compare the
survival curves. P<0.05 was considered to indicate a
statistically significant difference. The patients were divided
into two groups according to their NLR: High NLR (NLR >3.0) and
low NLR (NLR ≤3.0). Survival and response to chemotherapy were
compared between groups. OS was defined as the time from the start
of chemotherapy until death.
Results
All of the enrolled patients were divided according
to their NLR, and the correlation of NLR with nutritional markers,
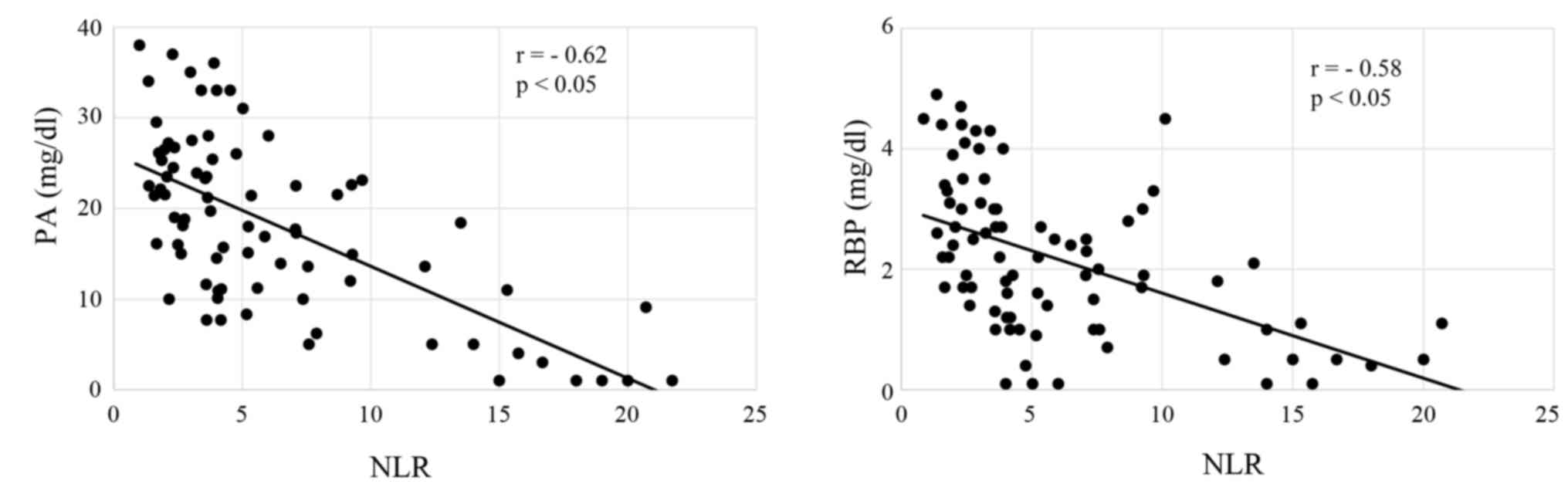
including PA, RBP, CRP and SI, was analyzed. Serum levels of PA and
RBP were both significantly inversely correlated with NLR in
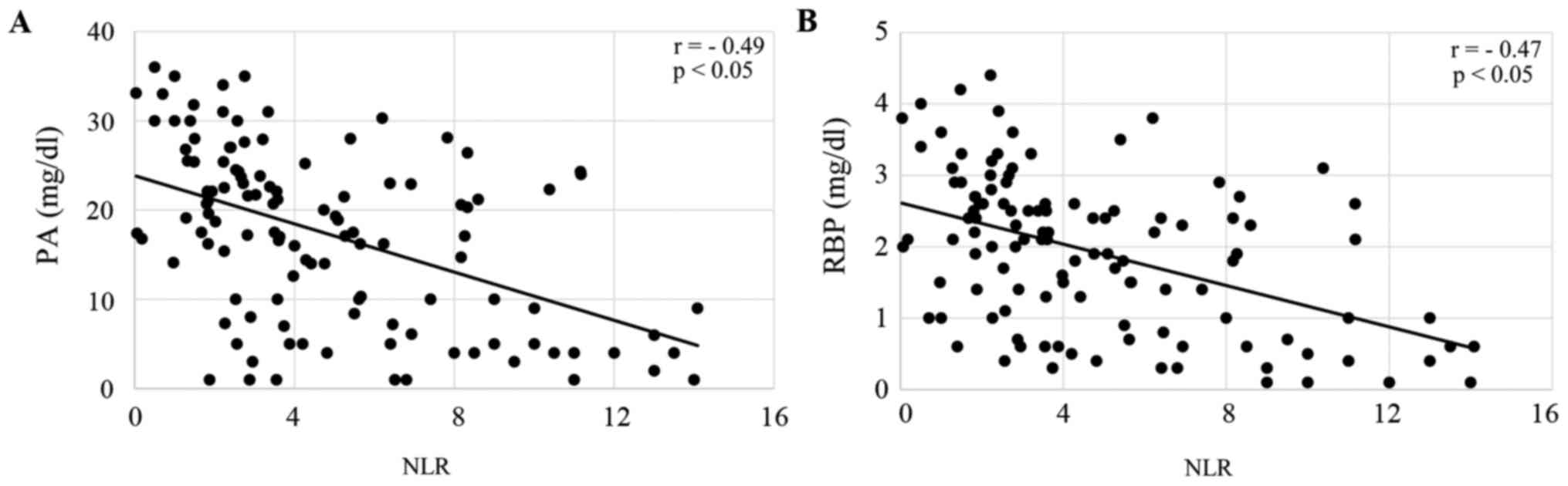
patients treated with CRT (both P<0.05; Fig. 1A and B), and patients treated with FP
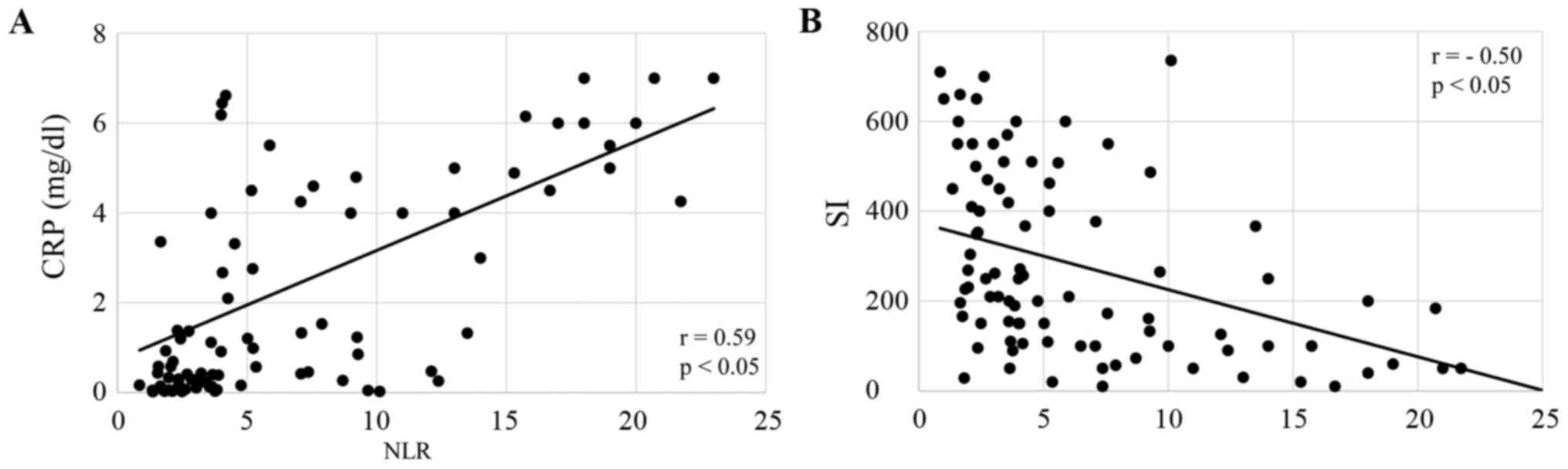
(both P<0.05; Fig. 2A and B). CRP
levels were significantly correlated, and SI was inversely
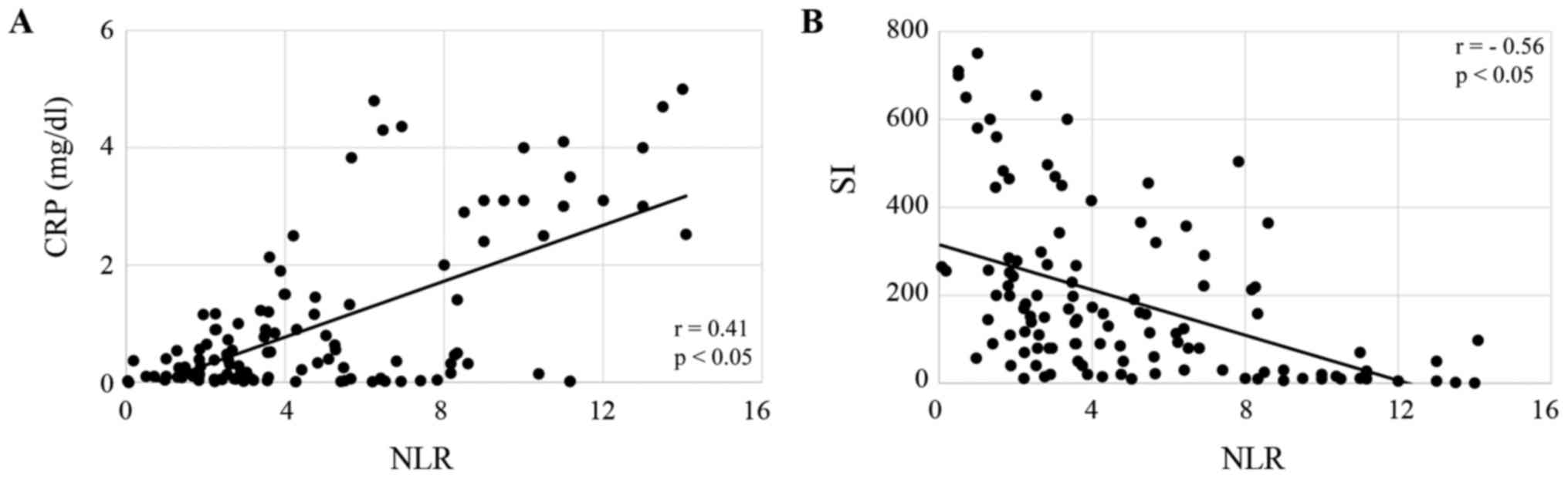
correlated with NLR in CRT patients (both P<0.05; Fig. 3A and B) and FP patients (both
P<0.05; Fig. 4A and B). The
responses to CRT and FP according to RECIST criteria are presented
in Table II. In patients treated with
CRT, a partial response was significantly higher in patients with a
low NLR (19.3% vs. 54.7%; P<0.05; Table II) and with progressive disease
compared to those with a high NLR (49.1% vs. 15.1%; P<0.05;
Table II). In patients treated with
FP, a partial response was also significantly higher in patients
with a low NLR (13.1% vs. 39.7%; P<0.05; Table II) and with progressive disease
compared to those with a high NLR (47.6% vs. 19.1%; P<0.05;
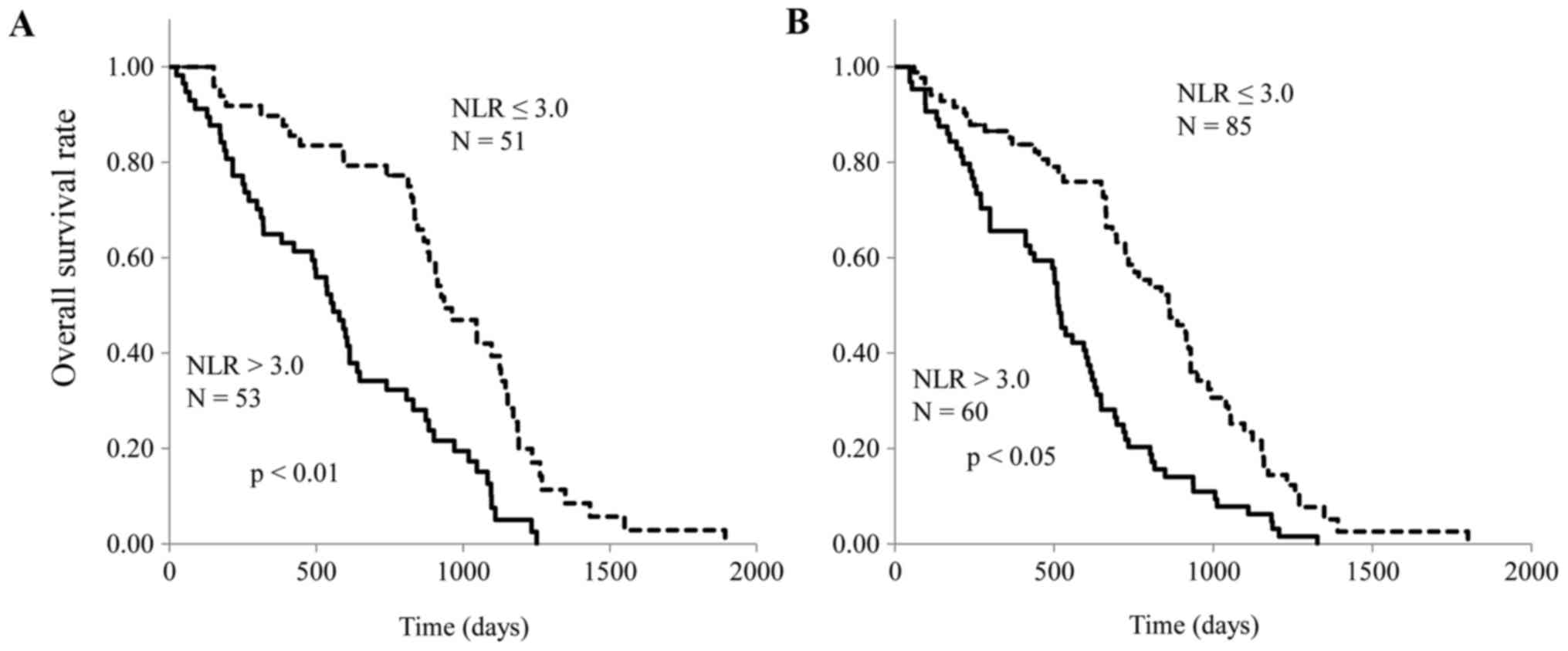
Table II). Fig. 5 demonstrates the relationship between
NLR and OS in patients with ESCC treated with CRT and FP. OS of
patients with CRT and FP were both significantly worse in patients
with a high NLR than in those with a low NLR (Fig. 5; P<0.01 and P<0.05,
respectively).
 | Table II.Responses of CRT and FP. |
Table II.
Responses of CRT and FP.
| Responses | CR | PR | SD | PD | n | P-value |
|---|
| CRT |
|
|
|
|
|
|
|
NLR>3 | 0 | 11 (19.3%) | 18 (31.6%) | 28
(49.1)a | 57 | <0.05 |
|
NLR≤3 | 1 (1.9%) | 29
(54.7%)a | 15 (28.3%) | 8 (15.1%) | 53 |
|
| FP |
|
|
|
|
|
|
|
NLR>3 | 0 | 8 (13.1%) | 24 (39.3%) | 29
(47.6%)a | 61 | <0.05 |
|
NLR≤3 | 0 | 35
(39.3%)a | 37 (41.6%) | 17 (19.1%) | 89 |
|
Discussion
In the present study, the ability of NLR to serve as
a prognostic indicator of survival in patients with locally
advanced and metastatic ESCC treated with CRT or FP was analyzed.
The results demonstrated that NLR was a useful marker of
malnutrition, systemic inflammation and immune suppression, and was
also a strong prognostic indicator.
Various inflammation-related markers such as CRP,
NLR and GPS are influenced by the production of pro- and
anti-inflammatory cytokines, and are associated with a poor
prognosis in various types of cancer (22–24). Immune
suppression was closely associated with increased NLR as the levels
of SI were significantly inversely correlated to increased NLR. The
authors previously reported that increasing levels of circulating
myeloid-derived suppressor cells (MDSCs) correlate with decreased
SI, malnutrition, and increased vascular endothelial growth factor
(VEGF) levels in patients with cancer (36,37). The
authors speculated that immune suppression may also occur with
increased MDSC levels, activated by inflammation or tumor-produced
VEGF.
It remains unclear why tumor responses to
chemotherapy are associated with NLR or systemic inflammation.
Because malnutrition, immune suppression and PS are closely
associated with one other, patients with a fair PS may be able to
receive higher doses of chemotherapeutic drugs or a dose-dense
chemotherapy schedule. Another possibility was recently raised.
Immunogenic cell death after chemotherapy or radiotherapy has been
reported (38,40,41).
Moreover, it is possible that lymphocytes in cancer-bearing hosts
can recognize neoantigens, tumor-specific mutation-derived antigens
(42). Because immune function depends
upon systemic inflammation, the anti-tumor activity of cytotoxic T
lymphocytes that recognize tumor cells may be suppressed in
patients with high inflammation, and the response to chemotherapy
and the prognosis of these patients may be poor.
In conclusion, the results of the present study
suggested that NLR may serve as a useful marker of the tumor
response, immune suppression, malnutrition and prognosis upon CRT
or FP in patients with locally advanced or metastatic ESCC.
However, because NLR is easily influenced by infection or stress, a
useful cut-off level needs to be investigated in clinical practice.
Furthermore, a combination of anti-inflammatory with
chemotherapeutic agents may have therapeutic benefits in ESCC;
thus, further studies in this area are needed.
References
|
1
|
Ferlay J, Soerjomataram I, Dikshit R, Eser
S, Mathers C, Rebelo M, Parkin DM, Forman D and Bray F: Cancer
incidence and mortality worldwide: Sources, methods and major
patterns in GLOBOCAN 2012. Int J Cancer. 136:E359–E386. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Sohda M and Kuwano H: Current status and
future prospects for esophageal cancer treatment. Ann Thorac
Cardiovasc Surg. 23:1–11. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Coussens LM and Werb Z: Inflammation and
cancer. Nature. 420:860–867. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Balkwill F and Mantovani A: Inflammation
and cancer: Back to Virchow? Lancet. 357:539–545. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Jaiswal M, LaRusso NF, Burgart LJ and
Gores GJ: Inflammatory cytokines induce DNA damage and inhibit DNA
repair in cholangiocarcinoma cells by a nitric oxide-dependent
mechanism. Cancer Res. 60:184–190. 2000.PubMed/NCBI
|
|
6
|
McMillan DC: The systemic
inflammation-based Glasgow Prognostic Score: A decade of experience
in patients with cancer. Cancer Treat Rev. 39:534–540. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Smith RA, Bosonnet L, Raraty M, Sutton R,
Neoptolemos JP, Campbell F and Ghaneh P: Preoperative
platelet-lymphocyte ratio is an independent significant prognostic
marker in resected pancreatic ductal adenocarcinoma. Am J Surg.
197:466–472. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Tomita M, Shimizu T, Ayabe T, Yonei A and
Onitsuka T: Preoperative neutrophil to lymphocyte ratio as a
prognostic predictor after curative resection for non-small cell
lung cancer. Anticancer Res. 31:2995–2998. 2011.PubMed/NCBI
|
|
9
|
Pinato DJ, Shiner RJ, Seckl MJ, Stebbing
J, Sharma R and Mauri FA: Prognostic performance of
inflammation-based prognostic indices in primary operable non-small
cell lung cancer. Br J Cancer. 110:1930–1935. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhang H, Zhang L, Zhu K, Shi B, Yin Y, Zhu
J, Yue D, Zhang B and Wang C: Prognostic significance of
combination of preoperative platelet count and
neutrophil-lymphocyte ratio (COP-NLR) in patients with non-small
cell lung cancer: Based on a large cohort study. PLoS One.
10:e01264962015. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Shibutani M, Maeda K, Nagahara H, Ohtani
H, Iseki Y, Ikeya T, Sugano K and Hirakawa K: The prognostic
significance of a postoperative systemic inflammatory response in
patients with colorectal cancer. World J Surg Oncol. 13:1942015.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Albayrak S, Zengin K, Tanik S, Atar M,
Unal SH, Imamoglu MA and Gurdal M: Can the neutrophil-to-lymphocyte
ratio be used to predict recurrence and progression of
non-muscle-invasive bladder cancer? Kaohsiung J Med Sci.
32:327–333. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Dong YW, Shi YQ, He LW and Su PZ:
Prognostic significance of neutrophil-to-lymphocyte ratio in rectal
cancer: A meta-analysis. Onco Targets Ther. 9:3127–3134.
2016.PubMed/NCBI
|
|
14
|
Nakamura K, Nagasaka T, Nishida T, Haruma
T, Ogawa C, Kusumoto T, Seki N and Hiramatsu Y: Neutrophil to
lymphocyte ratio in the pre-treatment phase of final-line
chemotherapy predicts the outcome of patients with recurrent
ovarian cancer. Oncol Lett. 11:3975–3981. 2016.PubMed/NCBI
|
|
15
|
Aino H, Sumie S, Niizeki T, Kuromatsu R,
Tajiri N, Nakano M, Satani M, Okamura S, Shimose S, Miyahara K, et
al: The systemic inflammatory response as a prognostic factor for
advanced hepatocellular carcinoma with extrahepatic metastasis. Mol
Clin Oncol. 5:83–88. 2016.PubMed/NCBI
|
|
16
|
Ding PR, An X, Zhang RX, Fang YJ, Li LR,
Chen G, Wu XJ, Lu ZH, Lin JZ, Kong LH, et al: Elevated preoperative
neutrophil to lymphocyte ratio predicts risk of recurrence
following curative resection for stage IIA colon cancer. Int J
Colorectal Dis. 25:1427–1433. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Jung MR, Park YK, Jeong O, Seon JW, Ryu
SY, Kim DY and Kim YJ: Elevated preoperative neutrophil to
lymphocyte ratio predicts poor survival following resection in late
stage gastric cancer. J Surg Oncol. 104:504–510. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Stotz M, Gerger A, Eisner F, Szkandera J,
Loibner H, Ress AL, Kornprat P, AlZoughbi W, Seggewies FS, Lackner
C, et al: Increased neutrophil-lymphocyte ratio is a poor
prognostic factor in patients with primary operable and inoperable
pancreatic cancer. Br J Cancer. 109:416–421. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Li Y, An J, Huang S, He J and Zhang J:
Esophageal cancer-derived microvesicles induce regulatory B cells.
Cell Biochem Funct. 33:308–313. 2015. View
Article : Google Scholar : PubMed/NCBI
|
|
20
|
Gholamin M, Moaven O, Memar B, Farshchian
M, Naseh H, Malekzadeh R, Sotoudeh M, Rajabi-Mashhadi MT, Forghani
MN, Farrokhi F, et al: Overexpression and interactions of
interleukin-10, transforming growth factor beta, and vascular
endothelial growth factor in esophageal squamous cell carcinoma.
World J Surg. 33:1439–1445. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Chen MF, Chen PT, Chen WC, Lu MS, Lin PY
and Lee KD: The role of PD-L1 in the radiation response and
prognosis for esophageal squamous cell carcinoma related to IL-6
and T-cell immunosuppression. Oncotarget. 7:7913–7924.
2016.PubMed/NCBI
|
|
22
|
Grivennikov SI, Greten FR and Karin M:
Immunity, inflammation, and cancer. Cell. 140:883–899. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
McMillan DC: Systemic inflammation,
nutritional status and survival in patients with cancer. Curr Opin
Clin Nutr Metab Care. 12:223–226. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Zahorec R: Ratio of neutrophil to
lymphocyte counts - rapid and simple parameter of systemic
inflammation and stress in critically ill. Bratisl Lek Listy.
102:5–14. 2001.PubMed/NCBI
|
|
25
|
Higuchi K, Koizumi W, Tanabe S, Sasaki T,
Katada C, Azuma M, Nakatani K, Ishido K, Naruke A and Ryu T:
Current management of esophageal squamous-cell carcinoma in Japan
and other countries. Gastrointest Cancer Res. 3:153–161.
2009.PubMed/NCBI
|
|
26
|
Herskovic A, Martz K, al-Sarraf M,
Leichman L, Brindle J, Vaitkevicius V, Cooper J, Byhardt R, Davis L
and Emami B: Combined chemotherapy and radiotherapy compared with
radiotherapy alone in patients with cancer of the esophagus. N Engl
J Med. 326:1593–1598. 1992. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Ishida K, Iizuka T, Ando N and Ide H:
Phase II study of chemoradiotherapy for advanced squamous cell
carcinoma of the thoracic esophagus: Nine Japanese institutions
trial. Jpn J Clin Oncol. 26:310–315. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Finn OJ: Cancer immunology. N Engl J Med.
358:2704–2715. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Yoshimoto Y, Suzuki Y, Mimura K, Ando K,
Oike T, Sato H, Okonogi N, Maruyama T, Izawa S, Noda SE, et al:
Radiotherapy-induced anti-tumor immunity contributes to the
therapeutic efficacy of irradiation and can be augmented by CTLA-4
blockade in a mouse model. PLoS One. 9:e925722014. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Lee Y, Auh SL, Wang Y, Burnette B, Wang Y,
Meng Y, Beckett M, Sharma R, Chin R, Tu T, et al: Therapeutic
effects of ablative radiation on local tumor require CD8+ T cells:
Changing strategies for cancer treatment. Blood. 114:589–595. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Takeshima T, Chamoto K, Wakita D, Ohkuri
T, Togashi Y, Shirato H, Kitamura H and Nishimura T: Local
radiation therapy inhibits tumor growth through the generation of
tumor-specific CTL: Its potentiation by combination with Th1 cell
therapy. Cancer Res. 70:2697–2706. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Shibata M and Gonda K: Cachexia,
immunological participation. In: Horizons in Cancer ResearchNova
Science. Watanabe HS: Publishers Inc.; New York: pp. 19–32.
2015
|
|
33
|
Shibata M, Nezu T, Kanou H, Abe H,
Takekawa M and Fukuzawa M: Decreased production of interleukin-12
and type 2 immune responses are marked in cachectic patients with
colorectal and gastric cancer. J Clin Gastroenterol. 34:416–420.
2002. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Shibata M, Nagata Y, Kimura T, Kanou H,
Nezu T, Takekawa M and Fukuzawa M: Elevated serum concentration of
interleukin-1 receptor antagonist (IL-1ra) is correlated to
interleukin-6 and hypoalbuminemia in cachectic patients with
colorectal cancer. Int J Clin Oncol. 5:116–120. 2000. View Article : Google Scholar
|
|
35
|
Shibata M and Takekawa M: Increased serum
concentration of circulating soluble receptor for interleukin-2 and
its effect as a prognostic indicator in cachectic patients with
gastric and colorectal cancer. Oncology. 56:54–58. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Ohki S, Shibata M, Gonda K, Machida T,
Shimura T, Nakamura I, Ohtake T, Koyama Y, Suzuki S, Ohto H, et al:
Circulating myeloid-derived suppressor cells are increased and
correlated to immune suppression and hypoalbuminemia in patients
with cancer. Oncol Rep. 28:453–458. 2012.PubMed/NCBI
|
|
37
|
Nakamura I, Shibata M, Gonda K, Yazawa T,
Shimura T, Anazawa T, Suzuki S, Sakurai K, Koyama Y, Ohto H, et al:
Serum levels of vascular endothelial growth factor are increased
and correlate with malnutrition, immunosuppression involving MDSCs
and systemic inflammation in patients with cancer of the digestive
system. Oncol Lett. 5:1682–1686. 2013.PubMed/NCBI
|
|
38
|
Suzuki Y, Mimura K, Yoshimoto Y, Watanabe
M, Ohkubo Y, Izawa S, Murata K, Fujii H, Nakano T and Kono K:
Immunogenic tumor cell death induced by chemoradiotherapy in
patients with esophageal squamous cell carcinoma. Cancer Res.
72:3967–3976. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Eisenhauer EA, Therasse P, Bogaerts J,
Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S,
Mooney M, et al: New response evaluation criteria in solid tumours:
Revised RECIST guideline (version 1.1). Eur J Cancer. 45:228–247.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
40
|
Yoshimoto Y, Kono K and Suzuki Y:
Anti-tumor immune responses induced by radiotherapy. Fukushima J
Med Sci. 61:13–22. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
41
|
Garg AD, Galluzzi L, Apetoh L, Baert T,
Birge RB, Bravo-San Pedro JM, Breckpot K, Brough D, Chaurio R,
Cirone M, et al: Molecular and translational classifications of
DAMPs in immunologic cell death. Front Immunol. 6:5882015.
View Article : Google Scholar : PubMed/NCBI
|
|
42
|
Wang RF and Wang HY: Immune targets and
neoantigens for cancer immunotherapy and precision medicine. Cell
Res. 27:11–37. 2017. View Article : Google Scholar : PubMed/NCBI
|