Spandidos Publications style
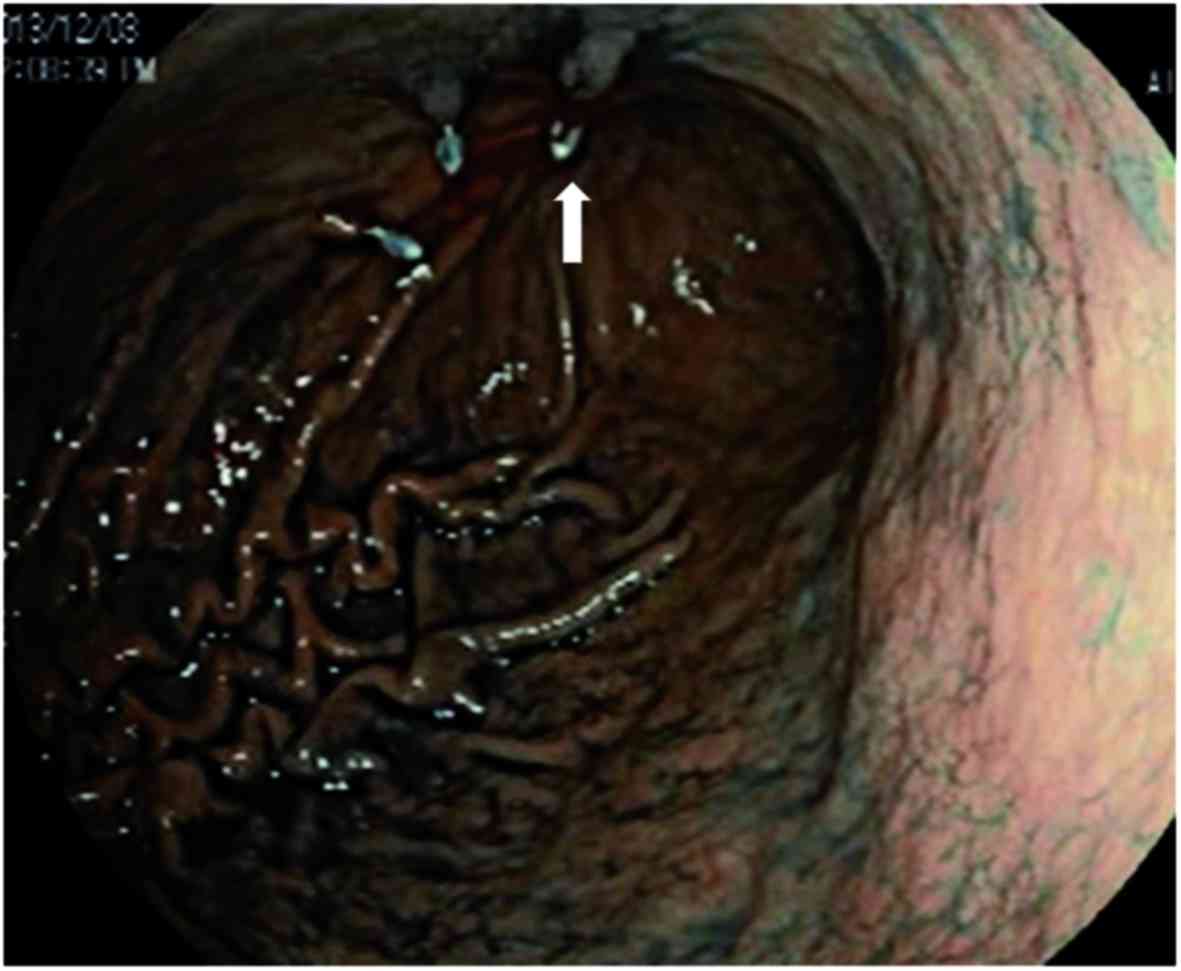
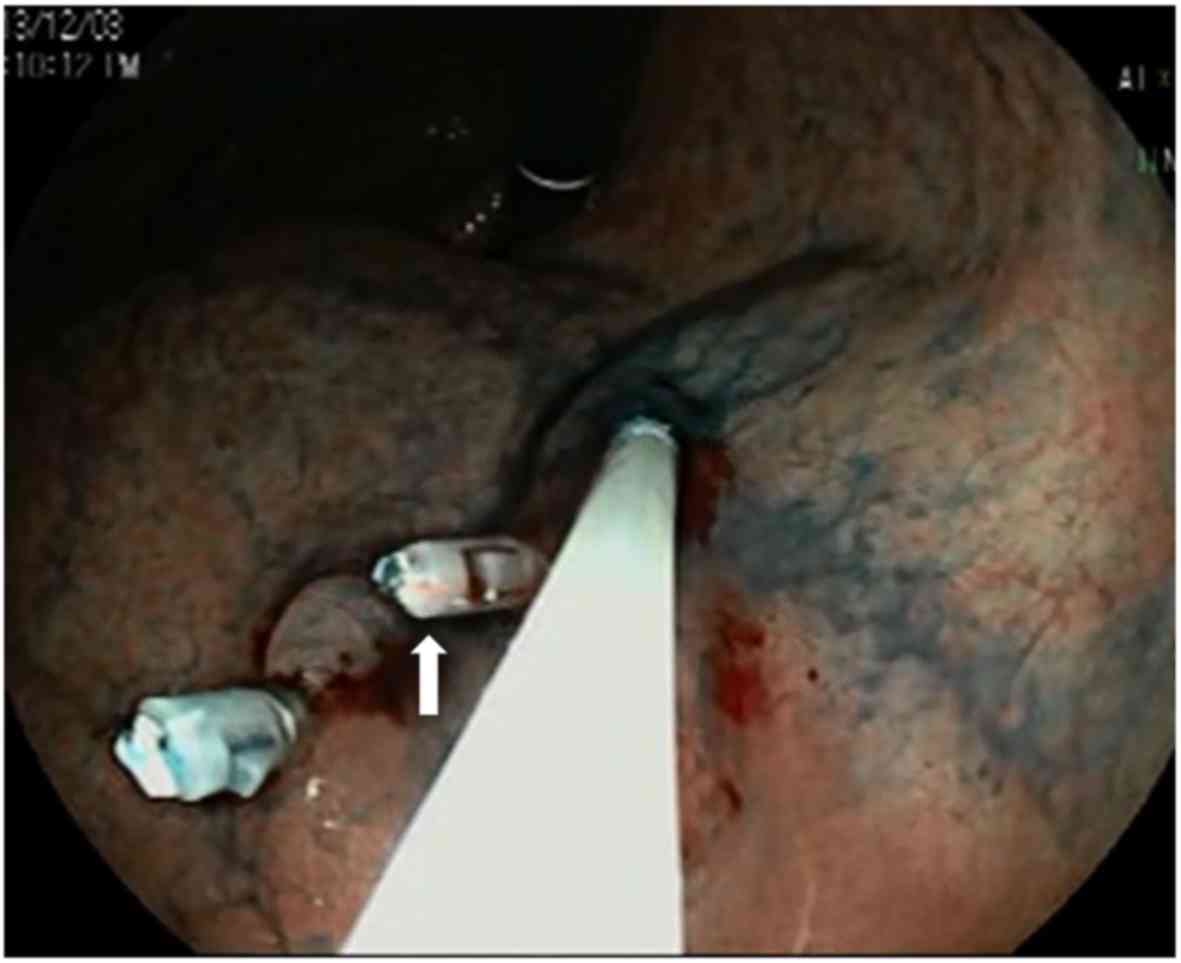
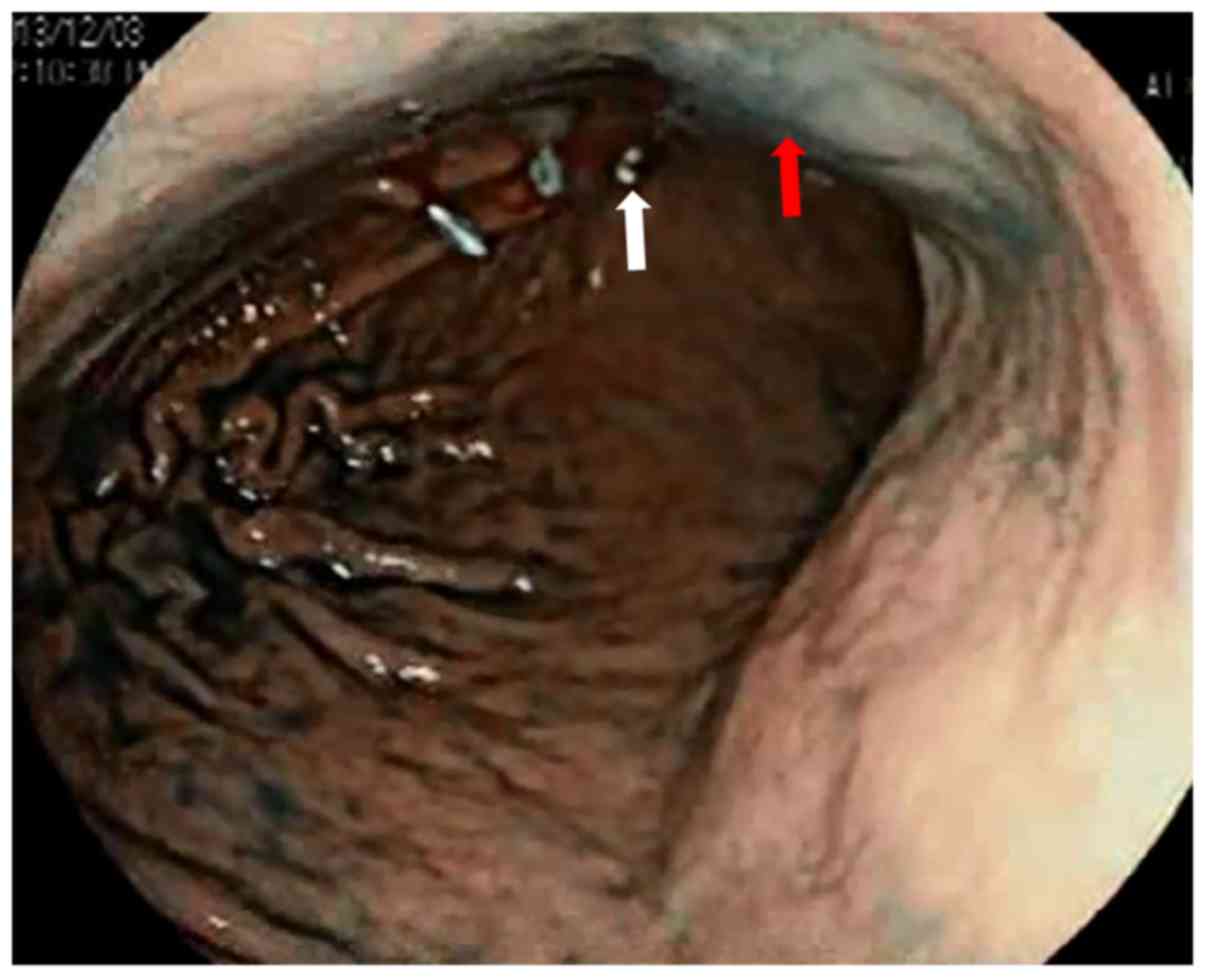
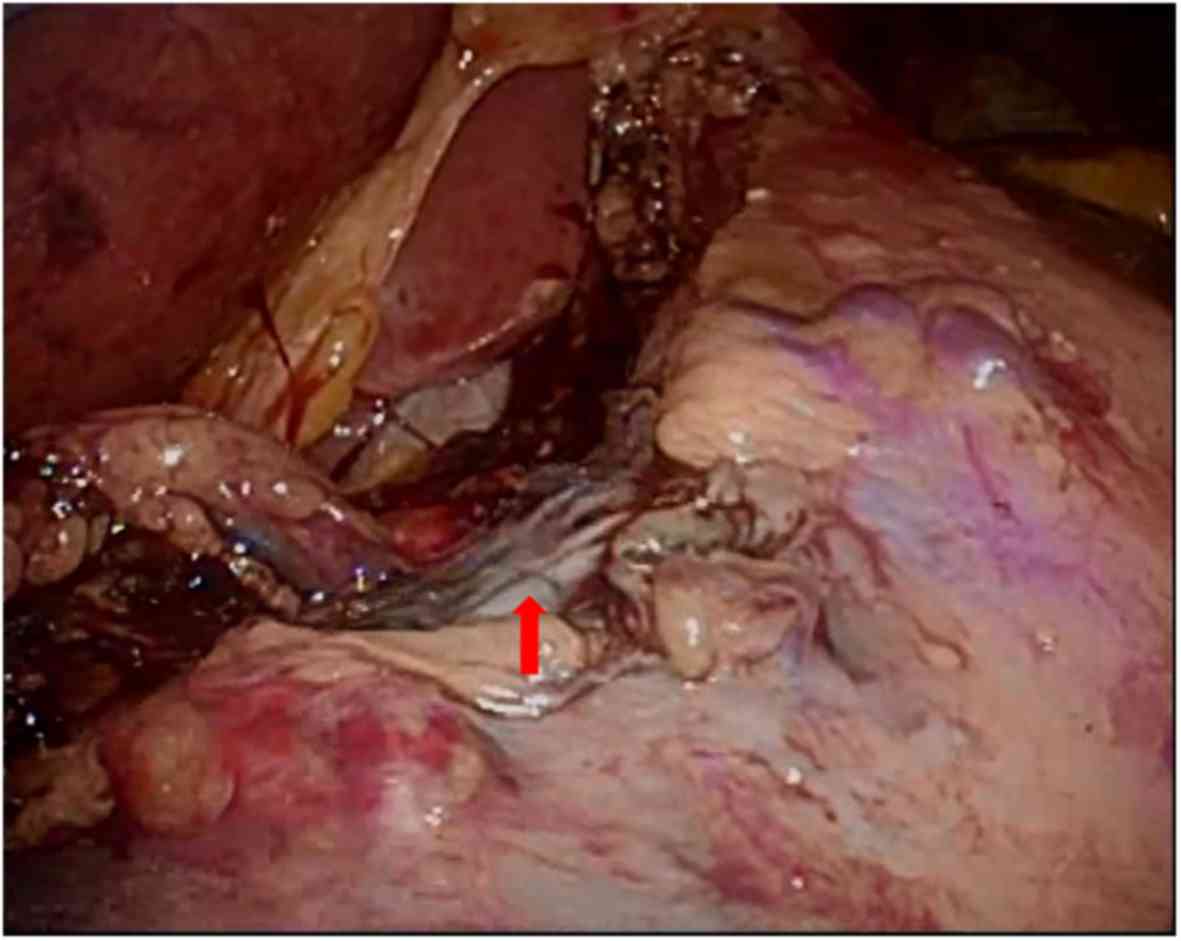
Tokuhara T, Nakata E, Tenjo T, Kawai I, Satoi S, Inoue K, Araki M, Ueda H and Higashi C: A novel option for preoperative endoscopic marking with India ink in totally laparoscopic distal gastrectomy for gastric cancer: A useful technique considering the morphological characteristics of the stomach. Mol Clin Oncol 6: 483-486, 2017.
APA
Tokuhara, T., Nakata, E., Tenjo, T., Kawai, I., Satoi, S., Inoue, K. ... Higashi, C. (2017). A novel option for preoperative endoscopic marking with India ink in totally laparoscopic distal gastrectomy for gastric cancer: A useful technique considering the morphological characteristics of the stomach. Molecular and Clinical Oncology, 6, 483-486. https://doi.org/10.3892/mco.2017.1191
MLA
Tokuhara, T., Nakata, E., Tenjo, T., Kawai, I., Satoi, S., Inoue, K., Araki, M., Ueda, H., Higashi, C."A novel option for preoperative endoscopic marking with India ink in totally laparoscopic distal gastrectomy for gastric cancer: A useful technique considering the morphological characteristics of the stomach". Molecular and Clinical Oncology 6.4 (2017): 483-486.
Chicago
Tokuhara, T., Nakata, E., Tenjo, T., Kawai, I., Satoi, S., Inoue, K., Araki, M., Ueda, H., Higashi, C."A novel option for preoperative endoscopic marking with India ink in totally laparoscopic distal gastrectomy for gastric cancer: A useful technique considering the morphological characteristics of the stomach". Molecular and Clinical Oncology 6, no. 4 (2017): 483-486. https://doi.org/10.3892/mco.2017.1191