Introduction
Epidermal cysts (EC) are benign subcutaneous or
intradermal tumors derived from the epidermis or the epithelial
hair follicle. They are formed from cystic enclosure of the
epithelium within the dermis, and filled with keratin and
lipid-rich debris. ECs commonly occur on the face, scalp, neck and
trunk, where the sebaceous glands are more active; the localization
within the bone is extremely uncommon, and the literature contains
~70 cases occurring in the distal phalanges of the fingers
(1); and only 4 into the temporal
bone (2–5).
In the ear region ECs are typically identified in
the posterior skin of the lobule or in the cartilaginous external
auditory canal (EAC) and appear as soft masses indistinguishable
from furuncles (2). Otomicroscopy
may reveal signs of external otitis due to infection or thickening
of the EAC. Clinical symptoms are otorrhea, pain and fullness, and
conductive hearing loss is also common. Computed tomography (CT)
and magnetic resonance imaging (MRI) aid diagnosis and planning of
the therapeutic approach, of which surgery is the most accepted
(2).
The current study presents, to the best of our
knowledge, the first case of EC of the temporal bone following
myringoplasty reported in the literature, focusing on its
development and management and describing a suitable surgical
technique to remove this type of lesion.
Case presentation
Informed consent was obtained from the patient for
publication of this study. A 24-year-old male presented with right
otorrhea and ipsilateral hypoacusia (May, 2016), having previously
undergone right overlay myringoplasty for subtotal eardrum
perforation (April, 2007) at the Ear Nose and Throat (ENT) Unit,
University of Naples Federico II (Naples, Italy). The follow-up
detected regular surgical outcomes until 9 years later, when by
otomicroscopy an erosion of the EAC posterior wall was observed,
with skin dislocated anteriorly and wax adherent to bone without
impairment of the tympanic membrane. Although the patient did not
report hypoacusia, audiometry revealed a right mild conductive
hearing loss. A high-resolution CT scan of the temporal bone
detected a non-homogeneous low-density tissue eroding the nearby
structures and surrounded by a bony capsule. MRI detected a
high-intensity tissue in the right mastoid on T2-weighted images
(Fig. 1).
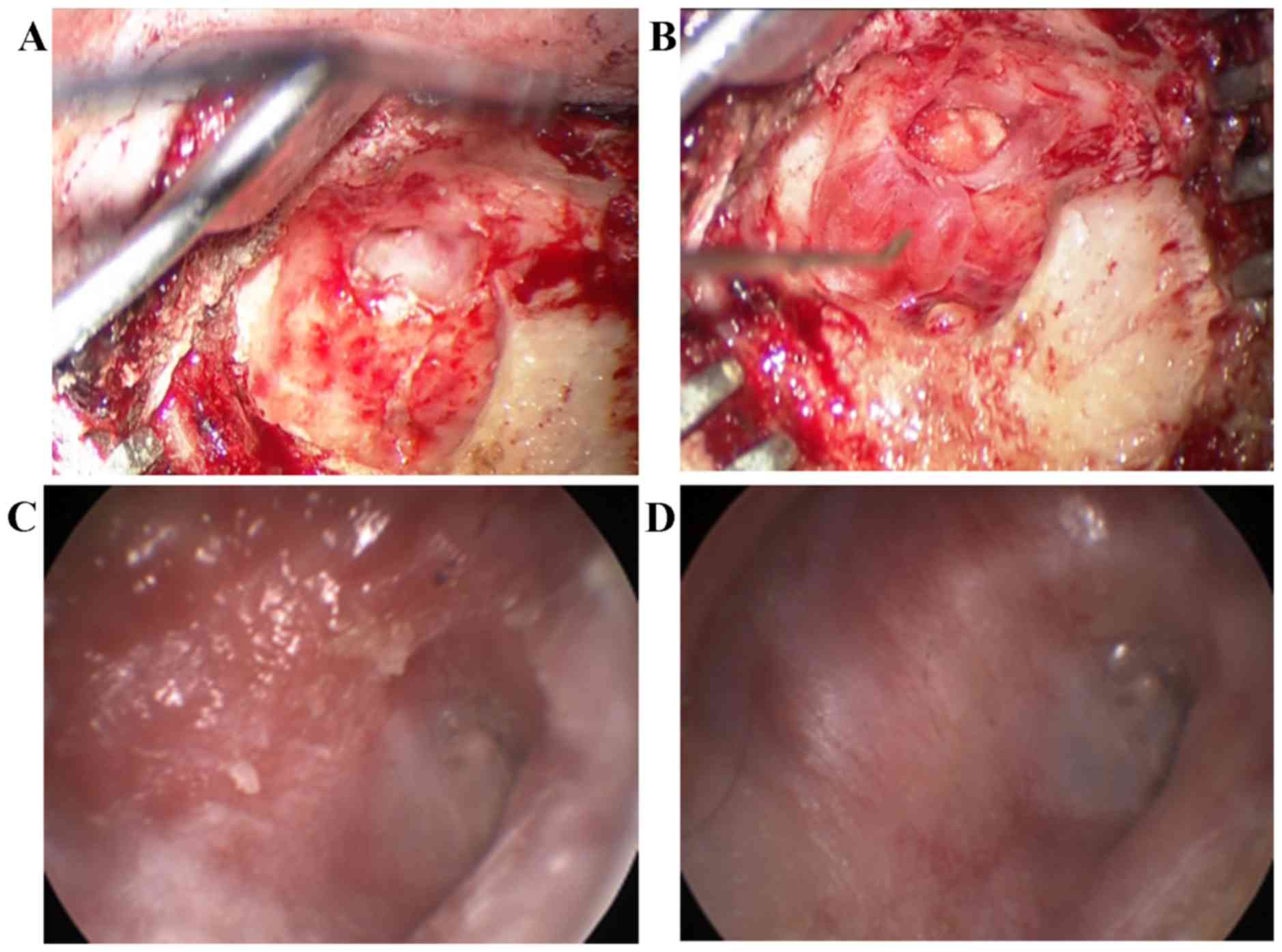
The patient underwent surgical treatment. The
surgical technique consisted of drilling the posterior wall of the
external auditory canal to access the attached cyst (Fig. 2A). The cyst skin coating and wax
within the pocket were removed and a section of temporalis fascia
was placed over the cystic wall in order to facilitate
re-epithelialization (Fig. 2B).
Finally meatoplasty was performed. As the tympanic
membrane did not exhibit any perforation and the cyst was located
laterally to it, the surgical procedure did not affect the middle
ear. The histological evaluation confirmed the diagnosis of EC of
the temporal bone. Epithelialization was effective at the 1-
(Fig. 2C) and 3-month follow-up
(Fig. 2D), and audiometry
examination revealed improvement.
Discussion
Myringoplasty is a common surgical procedure;
however, certain complications may occur, the most frequent of
which are anterior membrane perforations or re-perforations during
the underlay technique and the lateralization and/or blunting of
the membrane in the overlay technique (6,7).
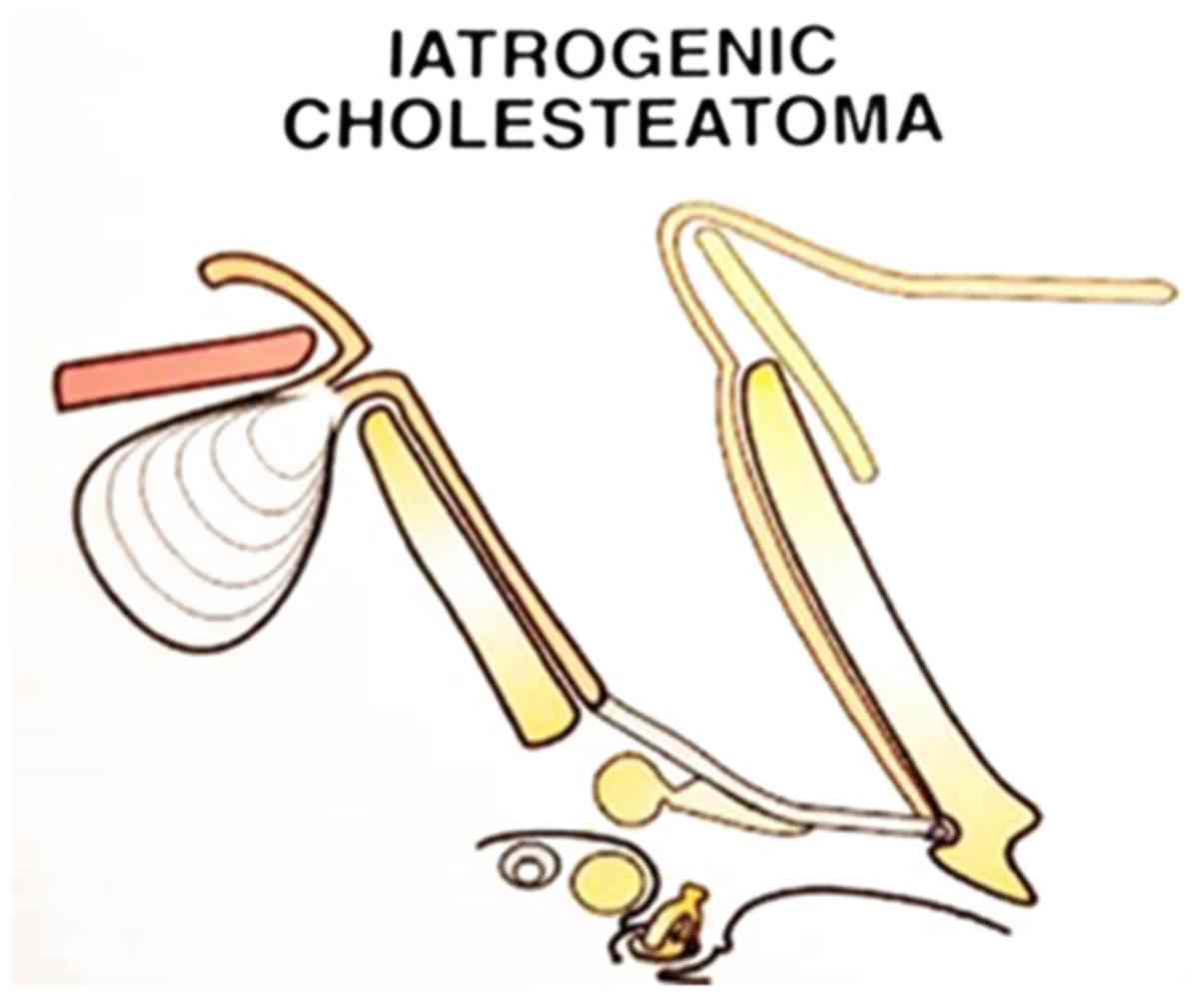
Irrespective of the surgical technique, a high degree of accuracy
is required in the repositioning of the skin flaps (Fig. 3) (8).
EC in the bone are extremely rare lesions (0.7% of cystic lesions)
typically occurring in the distal phalanges of the fingers
(2,8). The current study is, to the best of our
knowledge, the first case reported in the literature of temporal
bone EC following overlay myringoplasty.
Two main pathophysiological hypotheses on the
development of ECs exist; they may arise from the sequestration of
epidermal rests during embryonic growth, or from the implantation
of mature epithelial elements in the bony tissue as a consequence
of trauma, injury or surgery (2,9).
Due to the absence of components of the dermis,
which are present in dermoid cysts, the present study does not
support for the first hypothesis, whereas the second may be more
likely. Indeed, the history of earlier trauma or surgery prior to
the onset of the EC in the current case suggested the possible
migration of epidermis into the site of the injury. Furthermore, to
support the hypothesis of the implantation of mature epithelial
elements, Zadek and Cohen (10)
generated experimentally identical lesions by implantation of
epidermis in bone tissue.
In the current case, the trauma during the
myringoplasty was derived from the drilling of the bony EAC, where
loci minoris resistentiae, such as tympanosquamous and
tympanomastoid sutures, represented potentially suitable areas for
the migration of epithelial components from the sub-optimally
repositioned posterior meatal flap to the subperiostum. Over time,
the epithelial components led to cystic cavity formation in the
temporal bone.
In conclusion, for even simple surgical steps such
as myringoplasty, care must be taken to avoid complications. Errors
including poor repositioning of the skin flap may impact the
outcome of procedure a number of years later. The patient in the
current case remained free of symptoms. Occasionally during
follow-up, a ‘crack’ in the external auditory canal was detected
and radiological investigations were recommended. For this reason,
it is important to consider the relevance of clinical and
radiological follow-up in ear surgery.
Glossary
Abbreviations
Abbreviations:
|
EC
|
epidermal cysts
|
|
EAC
|
external auditory canal
|
|
CT
|
computed tomography
|
|
MRI
|
magnetic resonance imaging
|
References
|
1
|
Memon F, Panjwani TR and Patankar H:
Intraosseous epidermoid inclusion cyst of distal phalanx: A rare
entity. J Clin Diagn Res. 10:RJ01–RJ02. 2016.PubMed/NCBI
|
|
2
|
Yu WN, Fu SC and Lai JC: Epidermal cyst of
the bony external auditory canal. Kaohsiung J Med Sci. 29:237–238.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
de Gaudemar I, Elmaleh M, Cortez A,
Peuchmaur M and François M: Unusual presentation of a first
branchial cleft. Eur Arch Otorhinolaryngol. 252:57–60. 1995.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Suzuki T, Taki M, Shibata T, Matsunami T,
Sakaguchi H, Yamamoto S and Hisa Y: Epidermal cyst of the bony
external auditory canal. Otolaryngol Head Neck Surg. 136:155–156.
2007. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Alimoglu Y, Mercan H, Karaman E and Oz B:
Epidermal inclusion cyst of external auditory canal. J Craniofac
Surg. 21:1290–1291. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Sergi B, Galli J, De Corso E, Parrilla C
and Paludetti G: Overlay versus underlay myringoplasty: Report of
outcomes considering closure of perforation and hearing function.
Acta Otorhinolaryngol Ital. 31:366–371. 2011.PubMed/NCBI
|
|
7
|
Sarkar S: A review on the history of
tympanoplasty. Indian J Otolaryngol Head Neck Surg. 65 Suppl
3:455–460. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Sanna M, Sunose H, Mancini F, Russo A and
Taibah AH: Middle ear and mastoid microsurgery. 2nd. Thieme;
2012
|
|
9
|
Doğanavşargil B, Ayhan E, Argin M,
Pehlivanoğlu B, Keçeci B, Sezak M, Başdemir G and Öztop F: Cystic
bone lesions: Histopathological spectrum and diagnostic challenges.
Turk Patoloji Derg. 31:95–103. 2015.PubMed/NCBI
|
|
10
|
Zadek I and Cohen HG: Epidermoid cyst of
the terminal phalanx of a finger; with a review of the literature.
Am J Surg. 85:771–774. 1953. View Article : Google Scholar : PubMed/NCBI
|