Introduction
Lung cancer is the most frequent cancer, with
>220,000 estimated new cases per year and accounting for
>140,000 estimated cancer deaths in the US (1). Despite the advance of therapeutic
strategy for this malignancy, the prognosis of patients with
advanced- or recurrent lung cancer is still poor, with 5-year
survival estimates of ~5% (1).
The programmed death-1 (PD-1) receptor, which is
expressed on activated T cells, is engaged by the ligands PD-1
ligand 1 (PD-L1) and PD-L2, which are expressed by tumor cells and
infiltrating immune cells (2). The
interaction of PD-1 with PD-L1 and PD-L2 inhibits T-cell activation
and promotes tumor immune escape (3,4).
Nivolumab is a fully human IgG4 anti-PD-1 antibody that disrupts
PD-1-mediated signaling and restores antitumor immunity (5). Immune checkpoint inhibitors (ICIs)
including nivolumab have been approved for the treatment of several
types of cancer, including advanced non-small cell lung cancer
(NSCLC), on the basis of recent clinical trials demonstrating that
it prolongs survival compared with that of cytotoxic chemotherapy
(6,7). However, treatment with ICIs such as
nivolumab is often accompanied by immune-related adverse events
(irAEs). A clear understanding of the precise indications and
management of irAEs is important for harnessing the full potential
of these agents. The recommended management of irAEs is based on
clinical experience or in accordance with procedures for the
management of autoimmune disease. While skin- or
gastrointestinal-related irAEs have been relatively well studied
(8), there are few reports regarding
nivolumab-induced cholangitis. Thus, few information is available
with regard to clinical manifestation and treatment outcome of this
rare type of irAE. Herein, we report a series of four cases of
nivolumab-induced cholangitis with NSCLC and review the literature
on cholangitis induced by nivolumab.
Patients and methods
We retrospectively reviewed the data from patients
with advanced or recurrent NSCLC who were treated with nivolumab
between December 2015 and December 2018 at Tottori University
Hospital (Yonago, Japan). Nivolumab (3.0 mg/kg) monotherapy was
administered intravenously every 2 weeks until disease progression
or irAE occurrence. Treatment-related select adverse events those
were potentially immune related (skin, gastrointestinal, endocrine,
hepatic, hypersensitivity/infusion reaction, pulmonary, and renal)
without any other causes were defined as irAEs (6,7). PD-L1
expression was assessed using the commercially available PD-L1 IHC
22C3 pharmDx assay (Dako North America). Expression was categorized
according to the tumor proportion score (TPS). A PD-L1 TPS of
<1% was considered negative.
Clinicopathological data, including the duration of
nivolumab treatment, response to nivolumab treatment, laboratory
abnormalities, radiological findings, and management of
nivolumab-related cholangitis, were analyzed. The data regarding
tumor specimens (histology, PD-L1 expression, and driver gene
alteration) was obtained at the diagnosis of disease. The other
data was obtained when nivolumab treatment was administered.
Computed tomography (CT) of the chest, abdomen, and/or pelvis was
performed prior to and every 2 months during nivolumab treatment.
Patients underwent abdominal CT and additional imaging tests,
including endoscopic retrograde cholangiopancreatography (ERCP),
endoscopic ultrasonography (EUS), or magnetic resonance
cholangiopancreatography (MRCP) upon abnormal hepatobiliary
function test (HFT) results during or after nivolumab treatment.
Cholangitis was defined as HFT abnormalities with a dominant
increase in biliary enzymes (alkaline phosphatase and γ-glutamyl
transferase) compared to transaminase (aspartate aminotransferase
and alanine aminotransferase) levels. Adverse events were graded
according to the National Cancer Institute Common Terminology
Criteria for Adverse Events (CTCAE), version 4.0. In this study, we
particularly focused on describing the clinical manifestation and
treatment outcome of nivolumab-induced cholangitis, one of rare
irAEs. In that sense, we performed computer searches of the
literature using the PubMed database, with the following keywords:
‘non-small cell lung cancer’; ‘nivolumab’; ‘cholangitis’; ‘biliary
injury’. Meeting abstracts were excluded from analysis, as were
articles written in languages other than English.
The patient characteristics and response to
nivolumab treatment were compared between patients with and without
irAEs using Mann-Whitney test for age, and Chi-square test for the
other characteristics, respectively. Statistical analyses were
performed using PASW Statistics 19 (IBM SPSS Statistics). P<0.05
was considered to indicate a statistically significant
difference.
Results
Clinicopathological characteristics of
patients with nivolumab-induced cholangitis
A total of 59 patients with advanced or recurrent
NSCLC were treated with nivolumab between December 2015 and
December 2018 at Tottori University Hospital. Among these 59
patients, we identified four patients who experienced
nivolumab-related cholangitis, yielding an incidence rate of 6.8%.
irAEs other than cholangitis that resulted in discontinuation of
nivolumab were observed in five (9.8%) patients (rash, n=2;
interstitial lung disease, n=1; hypopituitarism, n=1; diarrhea,
n=1). No patients experienced irAEs in multiple organs.
The baseline characteristics of patients are
summarized in Table I. There was no
significant difference between patients with and without irAEs. The
ages of the four patients with cholangitis ranged from 55 to 82
years (median age, 78 years). Among the four patients, three had
adenocarcinoma, and the other patient had squamous cell carcinoma.
Metastases to the liver upon the administration of nivolumab were
observed in one patient (case 4). None of the four patients had any
history of cholangitis or pancreatitis prior to the administration
of nivolumab treatment. PD-L1 expression was assessed in 31 (52.5%)
out of the 59 patients. Among the patients tested, all four
patients with any irAE were positive for PD-L1 expression (1–49%,
n=1; ≥50%, n=3). Among the 27 patients without irAEs in whom PD-L1
expression was assessed, 14 (51.9%) were positive for PD-L1
expression (1–49%, n=8; ≥50%, n=6). Driver gene alterations were
detected in three patients [KRAS mutation: Cases 2 and 3;
MET exon 14 skipping: Case 4; gene alterations were not
investigated in the patient with squamous cell carcinoma (case
1)].
 | Table I.Characteristics of patients with and
without irAEs (nivolumab-induced cholangitis or others). |
Table I.
Characteristics of patients with and
without irAEs (nivolumab-induced cholangitis or others).
| Characteristic | Patients with
cholangitis (n=4), n (%) | Patients with irAEs
other than cholangitis (n=5), n (%) | Patients without any
irAEs (n=50), n (%) | P-value |
|---|
| Age, range
(median) | 55–82 (78) | 62–79 (71) | 43–91 (66) | 0.16 |
| Sex |
|
|
| 0.98 |
| Male | 2 (50) | 5 (100) | 39 (78.0) |
|
|
Female | 2 (50) | 0 | 11 (22.0) |
|
| Histology |
|
|
| 0.97 |
|
Adenocarcinoma | 3 (75) | 2 (40.0) | 29 (58.0) |
|
| Squamous
cell carcinoma | 1 (25) | 2 (40.0) | 17 (34.0) |
|
|
LCNEC | 0 | 0 | 1
(2.0) |
|
|
NSCLC-NOS | 0 | 1 (20.0) | 3
(6.0) |
|
| Performance
status |
|
|
| 0.37 |
| 0–1 | 3 (75.0) | 3 (60.0) |
|
|
| 2–4 | 1 (25.0) | 2 (40.0) |
|
|
| Liver metastasis |
|
|
| 0.11 |
| Yes | 1 (25) | 1 (20.0) | 3
(6.0) |
|
| No | 3 (75) | 4 (80.0) | 47 (94.0) |
|
| Brain metastasis |
|
|
| 0.84 |
| Yes | 0 | 3 (60.0) | 15 (30.0) |
|
| No | 4 (100) | 2 (40.0) | 35 (70.0) |
|
| PD-L1 expression
(tumor proportion score), % |
|
|
| 0.07 |
|
<1 | 0 | 0 | 13 (26.0) |
|
|
1–49 | 0 | 1 (20.0) | 8
(16.0) |
|
|
>50 | 1 (25.0) | 2 (40.0) | 6
(12.0) |
|
|
Unknown | 3 (75.0) | 2 (40.0) | 23 (46.0) |
|
| Driver gene
alteration |
|
|
| 0.09 |
|
EGFR | 0 | 0 | 5
(10.0) |
|
|
ALK | 0 | 0 | 0 |
|
|
KRAS | 2 (50) | 1 (20.0) | 4
(8.0) |
|
|
Others | 1 (25) | 0 | 1
(2.0) |
|
| Not
detected | 0 | 2 (40.0) | 24 (48.0) |
|
|
Unknown | 1 (25) | 2 (40.0) | 16 (32.0) |
|
| Timing of
nivolumab |
|
|
| 0.94 |
|
2nd | 2 (50) | 1 (20.0) | 16 (31.4) |
|
| 3rd or
later | 2 (50) | 4 (80.0) | 34 (68.6) |
|
| Response to
nivolumab |
|
|
| 0.02 |
|
CR+PR | 2 (50) | 4 (80.0) | 14 (27.5) |
|
| SD | 2 (50) | 0 | 17 (33.3) |
|
| PD | 0 | 1 (20.0) | 18 (35.3) |
|
| NE | 0 | 0 | 1
(2.0) |
|
| Smoking |
|
|
| 0.94 |
| Current
or former | 3 (75.0) | 5 (100) | 44 (88.2) |
|
|
Never | 1 (25) | 0 | 6
(11.8) |
|
Nivolumab was administered as second-line therapy in
two patients (cases 2 and 3) and third-line therapy in the other
two patients (cases 1 and 4). The best response to nivolumab
treatment was partial response (PR), which was observed in two
patients (cases 1 and 3), while stable disease (SD) was observed in
the other two patients. Thus, the response rate (RR) and disease
control rate (DCR) in patients with cholangitis were 50 and 100%,
respectively. Among five patients with irAEs other than
cholangitis, PR was observed in four (80.0%) patients and PD in one
(20.0%) patient. The RR and DCR in the 50 patients without any
irAEs were 27.5 and 60.8%, respectively. The RR in patients with
irAEs was significantly higher than that in patients without irAEs
(66.7 vs. 27.5%, P=0.02).
Clinical manifestation of
nivolumab-related cholangitis
HFT abnormalities occurred after 2–24 cycles
(median, 6.5 cycles) of nivolumab treatment. Symptoms were fairly
mild and non-specific, including epigastric pain and appetite loss
at the time HFT abnormalities occurred. Biliary enzymes were
dominantly increased in all cases, with peak alkaline phosphatase
levels of 3,029-9,118 U/l (reference range, <322 U/l) and peak
γ-glutamyl transpeptidase levels of 829–3,442 U/l (reference range,
<32 U/l), compared with levels of hepatic enzymes, with peak
aspartate aminotransferase levels of 284–682 U/l (reference range,
<30 U/l) and peak alanine aminotransferase levels of 235–953 U/l
(reference range, <23 U/l). A moderate increase in total
bilirubin levels of ≤3.8 mg/dl was also observed.
There were no recent changes in medications, aside
from nivolumab. Serological tests for viral hepatitis, autoimmune
hepatitis, or cholangitis were performed to exclude other causes of
cholangitis in all four patients. None of the four patients were
positive for hepatitis B virus (HBV), hepatitis C virus (HCV),
IgG4, anti-smooth muscle antibody, or anti-mitochondrial antibody.
Three (75%) patients were positive for anti-nuclear antibody (ANA)
at the time of diagnosis of nivolumab-induced cholangitis. There
were no data available regarding auto-antibody status before
treatment with nivolumab.
Imaging results
Additional abdominal CT, ERCP, and EUS scans were
performed to diagnose the cause of the hepatobiliary abnormalities.
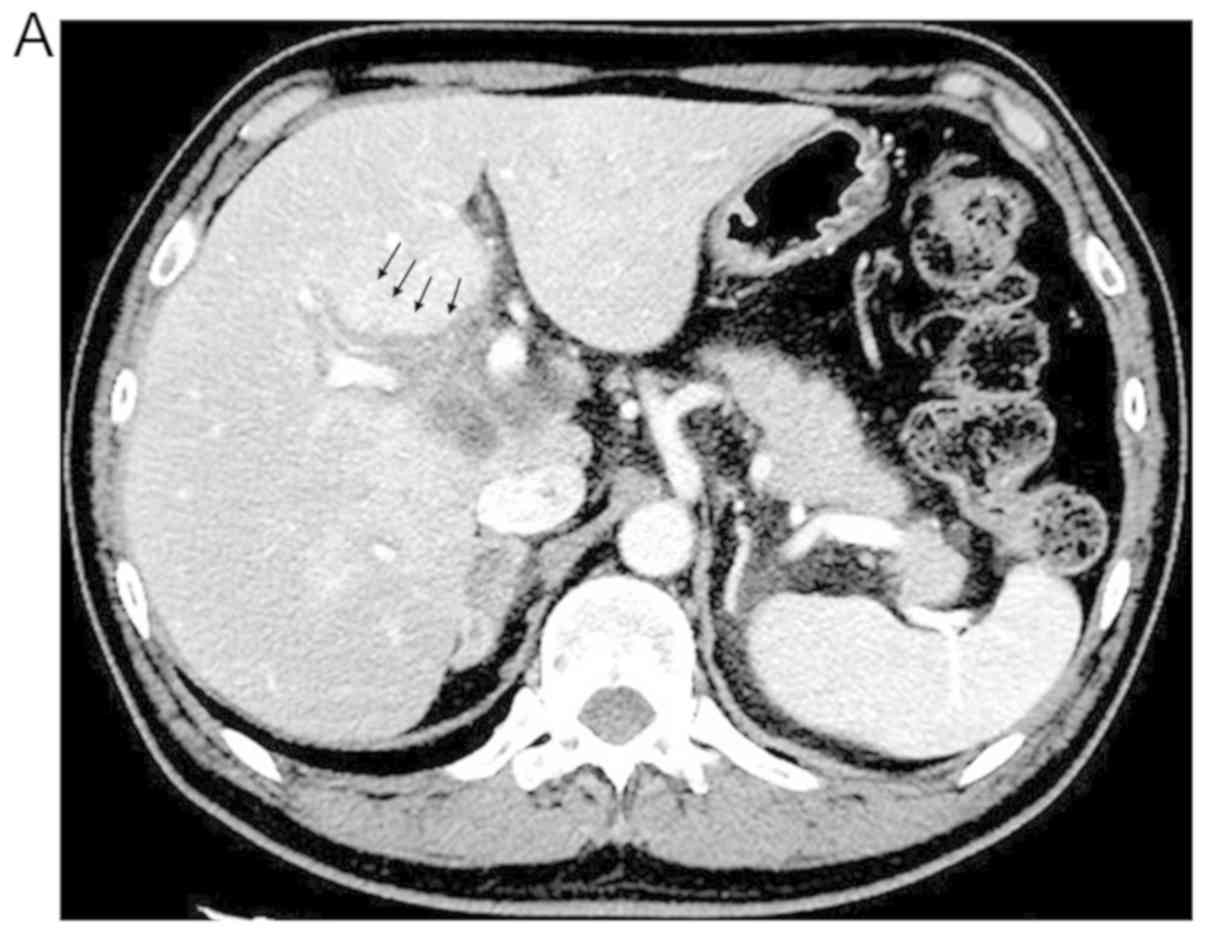
Characteristic imaging results are provided in Table II. In three cases (cases 1, 3, and
4), we identified common imaging patterns, including periportal
edema (PE), extrahepatic biliary duct (EHD) dilatation, and
hypertrophy of EHD, without any obstructive regions, including
stones or malignancy (Fig. 1).
 | Table II.Clinicopathological characteristics
of NSCLC patients with ICI-induced cholangitis. |
Table II.
Clinicopathological characteristics
of NSCLC patients with ICI-induced cholangitis.
| Case | Author, year | Age, years | Sex | Histology | Timing of
nivolumab | No. of cycles | Best response to
treatment with ICI | (Refs.) |
|---|
| 1 | – | 81 | F | Sq | 3rd line | 24 | PR | Present study |
| 2 | – | 75 | M | Ad | 2nd line | 2 | SD | Present study |
| 3 | – | 55 | M | Ad | 2nd line | 11 | PR | Present study |
| 4 | – | 82 | F | Ad | 3rd line | 2 | SD | Present study |
| 5 | Kawakami et
al, 2017 | 64 | M | Ad | 2nd line | 9 | PR | (10) |
| 6 | Kawakami et
al, 2017 | 73 | F | Sq | 4th line | 6 | PR | (10) |
| 7 | Kawakami et
al, 2017 | 82 | F | Sq | 2nd line | 12 | SD | (10) |
| 8 | Gelsomino et
al, 2017 | 79 | M | NSCLC-NOS | NA | 4 | PD | (11) |
| 9 | Kashima et
al, 2018 | 63 | M | Ad | 2nd line | 4 | N/A | (12) |
| 10 | Kuraoka et
al, 2018 | 69 | M | Ad | 3rd line | 3 | N/A | (13) |
Clinical course after onset of
nivolumab-induced cholangitis
From these clinical manifestations, serological
tests, and imaging results, we diagnosed these four cases with
nivolumab-induced cholangitis. Although nivolumab treatment was
immediately postponed, HFT abnormalities did not improve, but
rather worsened. Immunosuppressive treatment with systemic
corticosteroid [methylprednisolone (mPSL), 2.0 mg/kg daily] was
administered to all patients, and cases 1 and 3 were additionally
treated with mycophenolate mofetil (MMF) based on the
recommendation of the European Society for Medical Oncology (ESMO)
clinical practice guideline (9). The
time course of immunosuppressive treatment and HFT in all four
patients is summarized in Fig. 2. In
case 1, we treated with corticosteroid monotherapy (mPSL, 2 mg/kg
daily) first for 2 weeks. We then added MMF (1,000 mg twice daily)
because grade 3 HFT abnormalities persisted. HFT abnormalities
improved to grade 2 or less by 2 weeks after the addition of MMF.
Although she experienced abscess in the liver 1 month after the
administration of immunosuppressive drugs, probably as a side
effect of immunosuppression, the abscess was successfully treated
and managed with antibiotics and percutaneous drainage.
Case 2 was treated with corticosteroid monotherapy
(mPSL, 2 mg/kg daily), but HFT abnormalities did not improve. The
patient died of acute exacerbation of chronic obstructive pulmonary
disease (COPD) two months after the onset of nivolumab-related
cholangitis.
Case 3 had grade 4 cholangitis as with case 1, whose
grade 4 cholangitis was refractory to initial systemic
corticosteroid treatment. We worried about steroid refractory
situation, and decided to treat case 3 with corticosteroid (mPSL, 1
mg/kg daily) and MMF (1,000 mg twice daily) simultaneously. After
these drug administration, HFT abnormalities improved to grade 2 or
less in 2 weeks without any immunosuppressive treatment-related
complication.
In case 4, bacterial infection in the neck was
observed just after the onset of cholangitis; thus, this patient
was first treated with antibiotics for cervical infection.
Subsequently, she was treated with corticosteroid monotherapy
(mPSL, 2 mg/kg daily) for nivolumab-induced cholangitis, and HFT
abnormalities gradually improved.
Upon the improvement of HFT abnormalities,
immunosuppressive agents were tapered gradually in three cases (all
except case 2). Finally, the three cases whose cholangitis had
improved were maintained with an equivalent dose of prednisolone
(≤10 mg), and MMF was successfully terminated. The recurrence of
HFT abnormalities was not observed in any of the three cases.
Moreover, none received subsequent chemotherapy or ICI treatment.
Case 1 survived with SD at the data cut-off point without any
subsequent treatment. Based on the literature review, we identified
seven NSCLC patients with nivolumab-induced cholangitis (10–13).
Discussion
In this study, we present a rare case series of
NSCLC with cholangitis induced by nivolumab, including two cases
treated with a combination of corticosteroid and MMF. Immunotherapy
with monoclonal antibodies targeting cytotoxic T
lymphocyte-associated antigen 4 (CTLA4), as well as PD-1 and its
ligand PD-L1, has become standard care in the treatment of NSCLC,
with an increasing number of indications (6,7,14–16).
Therefore, an increasing number of patients will be exposed to
these drugs along with the risk of developing irAEs from these
treatments. The incidence of irAE is high, with reports of rates of
32.0–64.8% in phase III clinical trials of nivolumab for advanced
NSCLC. Among the irAEs, hepatotoxicity is observed in 1.5–7.7% of
NSCLC patients treated with nivolumab, making it less common than
skin-, gastrointestinal-, or endocrine-associated irAEs (6,7). In
particular, cholangitis induced by nivolumab is much less common,
and there is little information available regarding the
characteristics of patients who develop nivolumab-induced
cholangitis or its clinical manifestations and treatment
outcomes.
As summarized in Table
II, including our four cases, we identified 10 NSCLC patients
with cholangitis induced by nivolumab. The ages of these 10
patients ranged from 55 to 82 years (median age, 74 years), and the
data set included six (60.0%) men. Of the 10 patients, seven
(70.0%) had non-squamous NSCLC [adenocarcinoma: n=6, NSCLC-not
otherwise specified (NOS): n=1], and three (30.0%) had squamous
cell carcinoma. There were no apparent differences in the age
distributions or the proportion of histological types between
patients with nivolumab-induced cholangitis and other NSCLC cohorts
(17).
The results of a recent phase III study of nivolumab
in patients with non-squamous NSCLC showed that a greater RR was
observed as PD-L1 expression increased (7), although in patients with squamous
NSCLC, PD-L1 expression did not affect nivolumab efficacy (6). In addition, Haratani et al
(18) reported that the development
of irAEs is associated with the efficacy of nivolumab in patients
with NSCLC. These results suggest the possibility of an association
between the occurrence of irAEs, the response to nivolumab, and
PD-L1 expression. In this study, the RR and DCR in patients with
irAEs were higher than those in patients without irAEs, concomitant
with positive PD-L1 expression. In addition, of the eight cases
available for evaluation in terms of response to nivolumab
treatment, four (50.0%) achieved a PR and three (37.3%) had SD,
reflecting higher rates than those achieved in previous clinical
trials (6,7).
The response to nivolumab in patients with
cholangitis was comparable to that in patients with other irAEs,
indicating the possibility that nivolumab-induced cholangitis
occurs more frequently in patients with better responses to
nivolumab, as with other irAEs. In other words, irAEs, including
cholangitis, may occur particularly in patients who exhibit a
better response to nivolumab treatment. However, these associations
should be further investigated in future studies with larger sample
sizes.
Although irAEs can occur at any time, most develop
within a few weeks to a few months (6,7,19). Skin-related irAEs can develop
earlier, within 2–3 weeks after treatment, while hepatic irAEs
develop within 6–7 weeks (19). In
the 10 cases of nivolumab-induced cholangitis identified in this
study, cholangitis occurred after 2–24 cycles (median, 5 cycles) of
treatment, with three (30.0%) occurring after more than 10 cycles
of treatment. This indicates that ICI-induced cholangitis can also
occur later, as with other hepatic irAEs. Clinicians should
therefore keep in mind that a delayed effect of ICIs may occur
during follow-up.
The dilatation and hypertrophy of the EHD were
commonly observed according to imaging, being present in eight
(88.8%) of nine patients with imaging available for evaluation. PE
was also identified commonly, being present in three (75%) out of
our four cases (Table III). Kim
et al (20) reported that
such findings could be observed in ICI-associated hepatitis caused
by ipilimumab; however, both of these are non-specific and can be
observed in other hepatic diseases. These results demonstrate the
difficulty in distinguishing nivolumab-induced cholangitis from
other hepatobiliary diseases using imaging results alone.
 | Table III.Clinical manifestation and treatment
of nivolumab-induced cholangitis. |
Table III.
Clinical manifestation and treatment
of nivolumab-induced cholangitis.
|
|
|
| Imaging
results |
|
|
|---|
|
|
|
|
|
|
|
|---|
| Case | Symptoms | Grade | PE | EHD dilatation | IHD dilatation | Hypertrophy of
EHD | Treatment for
cholangitis | Improvement of
cholangitis |
|---|
| 1 | Low back pain | 4 | + | + | + | + | mPSL (2.0
mg/kg); | Yes |
|
|
|
|
|
|
|
| MMF (500 mg,
bid); |
|
|
|
|
|
|
|
|
| EST, EBD+stent |
|
| 2 | General fatigue,
appetite loss | 3 | – | – | – | – | mPSL (2.0
mg/kg) | No |
| 3 | Epigastric
pain | 4 | + | + | + | + | mPSL (2.0
mg/kg); | Yes |
|
|
|
|
|
|
|
| MMF (500 mg, bid);
EST |
|
| 4 | None | 3 | + | + | + | + | mPSL (2.0
mg/kg) | Yes |
| 5 | Fever, general
fatigue | 3 | – | + | – | + | EBD+stent;
Antibiotics | No |
| 6 | Itching,
jaundice | 4 | N/A | N/A | N/A | N/A | mPSL (1.0
mg/kg) | Yes |
| 7 | Fever, abdominal
discomfort | 3 | – | + | – | + | PSL (0.5
mg/kg) | Yes |
| 8 | Fever, vomiting,
abdominal discomfort, diarrhea | 3 | – | + | – | + | PSL (0.5 mg/kg);
EBD+stent | Yes |
| 9 | Epigastric pain,
soft stool | 3 | – | + | – | + | EBD+stent; PSL (2.0
mg/kg); Antibiotics | Yes |
| 10 | Pruritic rash | N/A | – | + | – | + | PSL (60 mg/day)
-> mPSL (500 mg/day) | No |
Cholangitis grade was severe in all nine patients
with data available, exhibiting grade 3 in six (66.6%) patients and
grade 4 in three (33.3%) patients (Table III). In general, the treatment for
an irAE of grade 3 or above is the discontinuation of the suspected
drugs and administration of systemic corticosteroids. When irAEs
are steroid-refractory, other additional immunosuppressive agents
should be considered (9). The
optimal management of irAEs is based on clinical experience or in
accordance with procedures for the management of autoimmune
disease, as no prospective trials have been conducted to evaluate
the best irAE treatment strategy. MMF is recommended for
steroid-refractory hepatitis according to the ESMO guideline
(9) and protocols of clinical trials
for nivolumab for advanced NSCLC (6,7);
however, there have been no case reports of NSCLC patients who
experienced severe nivolumab-induced cholangitis and were treated
with a combination of corticosteroid and MMF. To the best of our
knowledge, our two cases with grade 4 cholangitis were the first
NSCLC cases treated with a combination of corticosteroid and MMF
for nivolumab-induced cholangitis. In these two cases, HFT
abnormalities improved quickly after the administration of MMF
combined with corticosteroid. Although the adverse effects of
immunosuppressive treatment must be considered, especially that of
infection, our cases suggest that this combination treatment is
feasible and indeed effective against nivolumab-induced
cholangitis. It remains to be clarified, however, whether
simultaneous or sequential use of MMF is superior. However, owing
to the rarity of this irAE, prospective trials to evaluate the best
treatment strategy cannot be conducted. Therefore, further case
reports are needed to establish the optimal management of patients
with this irAE.
Limitations of this study include potential biases
associated with the initiation, dosage, choice of immunosuppressive
agents, and duration of immunosuppressive treatment, all of which
are inevitable in a retrospective study. In addition, we were
unable to perform histopathological analyses in the four cases from
this study because of our retrospective design.
In conclusion, we have reported and reviewed a case
series of NSCLC patients who developed cholangitis during ICI
treatment. Nivolumab-induced cholangitis is a rare irAE that is
more likely to develop in patients with better treatment responses
to ICI. The combination of corticosteroid and MMF was an effective
treatment in our two cases with grade 4 nivolumab-induced
cholangitis, and its efficacy should be investigated in additional
case reports.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed in the current
study are not publicly available but are available from the
corresponding author on reasonable request.
Authors' contributions
HI, TI and AYamas conceived and designed the study.
HI, NT, MK, JK, KT, RO, KYaman, YT, AYamam, YS, MY, TS, KYamag, HM
and AYamas acquired, analyzed and interpreted the data. HI drafted
the manuscript. All authors read and approved the final
manuscript.
Ethics approval and consent to
participate
The study design was approved by the Institutional
Review Board of Tottori University (approval no. 1054). Signed
informed consents were obtained from the patients.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
Glossary
Abbreviations
Abbreviations:
|
PD-1
|
programmed death-1
|
|
PD-L1
|
PD-1 ligand 1
|
|
NSCLC
|
non-small cell lung cancer
|
|
irAE
|
immune-related adverse event
|
|
HFT
|
hepatobiliary function test
|
|
PR
|
partial response
|
|
SD
|
stable disease
|
|
PD
|
progressive disease
|
|
RR
|
response rate
|
|
DCR
|
disease control rate
|
|
MMF
|
mycophenolate mofetil
|
|
mPSL
|
methylprednisolone
|
References
|
1
|
Siegel RL, Miller KD and Jemal A: Cancer
statistics, 2019. CA Cancer J Clin. 69:7–34. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Pardoll DM: The blockade of immune
checkpoints in cancer immunotherapy. Nat Rev Cancer. 12:252–264.
2012. View
Article : Google Scholar : PubMed/NCBI
|
|
3
|
Chen Y, Mu CY and Huang JA: Clinical
significance of programmed death-1 ligand-1 expression in patients
with non-small cell lung cancer: A 5-year-follow-up study. Tumori.
98:751–755. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Velcheti V, Schalper KA, Carvajal DE,
Anagnostou VK, Syrigos KN, Sznol M, Herbst RS, Gettinger SN, Chen L
and Rimm DL: Programmed death ligand-1 expression in non-small cell
lung cancer. Lab Invest. 94:107–116. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Topalian SL, Hodi FS, Brahmer JR,
Gettinger SN, Smith DC, McDermott DF, Powderly JD, Carvajal RD,
Sosman JA, Atkins MB, et al: Safety, activity, and immune
correlates of anti-PD-1 antibody in cancer. N Engl J Med.
366:2443–2454. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Brahmer J, Reckamp KL, Baas P, Crinò L,
Eberhardt WEE, Poddubskaya E, Antonia S, Pluzanski A, Vokes EE,
Holgado E, et al: Nivolumab versus docetaxel in advanced
squamous-cell non-small-cell lung cancer. N Engl J Med.
373:123–135. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Borghaei H, Paz-Ares L, Horn L, Spigel DR,
Steins M, Ready NE, Chow LQ, Vokes EE, Felip E, Holgado E, et al:
Nivolumab versus docetaxel in advanced nonsquamous non-small-cell
lung cancer. N Engl J Med. 373:1627–1639. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Michot JM, Bigenwald C, Champiat S,
Collins M, Carbonnel F, Postel-Vinay S, Berdelou A, Varga A,
Bahleda R, Hollebecque A, et al: Immune-related adverse events with
immune checkpoint blockade: A comprehensive review. Eur J Cancer.
54:139–148. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Haanen JBAG, Carbonnel F, Robert C, Kerr
KM, Peters S, Larkin J and Jordan K; ESMO Guidelines Committee, :
Management of toxicities from immunotherapy: ESMO Clinical Practice
Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 28
(Suppl 4):iv119–iv142. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Kawakami H, Tanizaki J, Tanaka K, Haratani
K, Hayashi H, Takeda M, Kamata K, Takenaka M, Kimura M, Chikugo T,
et al: Imaging and clinicopathological features of
nivolumab-related cholangitis in patients with non-small cell lung
cancer. Invest New Drugs. 35:529–536. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Gelsomino F, Vitale G and Ardizzoni A: A
case of nivolumab-related cholangitis and literature review: How to
look for the right tools for a correct diagnosis of this rare
immune-related adverse event. Invest New Drugs. 36:144–146. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Kashima J, Okuma Y, Shimizuguchi R and
Chiba K: Bile duct obstruction in a patient treated with nivolumab
as second-line chemotherapy for advanced non-small-cell lung
cancer: A case report. Cancer Immunol Immunother. 67:61–65. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Kuraoka N, Hara K, Terai S, Yatabe Y and
Horio Y: Peroral cholangioscopy of nivolumab-related (induced)
ulcerative cholangitis in a patient with non-small cell lung
cancer. Endoscopy. 50:E259–E261. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Rittmeyer A, Barlesi F, Waterkamp D, Park
K, Ciardiello F, von Pawel J, Gadgeel SM, Hida T, Kowalski DM, Dols
MC, et al: Atezolizumab versus docetaxel in patients with
previously treated non-small-cell lung cancer (OAK): A phase 3,
open-label, multicentre randomised controlled trial. Lancet.
389:255–265. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Hellmann MD, Ciuleanu T-E, Pluzanski A,
Lee JS, Otterson GA, Audigier-Valette C, Minenza E, Linardou H,
Burgers S, Salman P, et al: Nivolumab plus ipilimumab in lung
cancer with a high tumor mutational burden. N Engl J Med.
378:2093–2104. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Reck M, Rodríguez-Abreu D, Robinson AG,
Hui R, Csőszi T, Fülöp A, Gottfried M, Peled N, Tafreshi A, Cuffe
S, et al: Pembrolizumab versus chemotherapy for PD-L1-positive
non-small-cell lung cancer. N Engl J Med. 375:1823–1833. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Abernethy AP, Arunachalam A, Burke T,
McKay C, Cao X, Sorg R and Carbone DP: Real-world first-line
treatment and overall survival in non-small cell lung cancer
without known EGFR mutations or ALK rearrangements in US community
oncology setting. PLoS One. 12:e01784202017. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Haratani K, Hayashi H, Chiba Y, Kudo K,
Yonesaka K, Kato R, Kaneda H, Hasegawa Y, Tanaka K, Takeda M and
Nakagawa K: Association of immune-related adverse events with
nivolumab efficacy in non-small-cell lung cancer. JAMA Oncol.
4:374–378. 2017. View Article : Google Scholar
|
|
19
|
Weber JS, Kähler KC and Hauschild A:
Management of immune-related adverse events and kinetics of
response with ipilimumab. J Clin Oncol. 30:2691–2697. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Kim KW, Ramaiya NH, Krajewski KM,
Jagannathan JP, Tirumani SH, Srivastava A and Ibrahim N:
Ipilimumab- associated hepatitis: Imaging and clinicopathologic
findings. Invest New Drugs. 31:1071–1077. 2013. View Article : Google Scholar : PubMed/NCBI
|