Introduction
Tuvalu is a Polynesian Island nation consisting of
nine islands and reefs, located in the southwest Pacific Ocean
(latitude, 5–10° south; longitude 176–179° east) (1). The distance from Tuvalu's capital
(Funafuti) to Fiji's capital (Suva) is ~1,100 km, and about 4,200
km from Funafuti to Sydney (1).
The national land area of Tuvalu is only 25.9 km2, and
the highest point does not exceed 4 m above sea level (1). Currently, an estimated 11,000 people
live in Tuvalu (1). The Taiwan
International Cooperation and Development Fund (Taiwan ICDF) has
coordinated the medical resources of Taiwanese hospitals in order
to provide long-term medical assistance to eight countries in the
Pacific Ocean: Marshall Islands, Kiribati, Solomon Islands, Palau,
Nauru, Tuvalu, Papua New Guinea and Fiji (2). Based on the Mobile Medical Missions,
in 2009 Chung Shan University Hospital sent dermatologists to
Tuvalu. There is little information on the skin conditions of the
Tuvalu population. The aim of the current study was to determine
the most common skin diseases and to assess access to
dermatological care in a sample of Tuvaluan individuals.
Subjects and methods
Patients. All patients presenting with skin
disorders between 2009 and 2012 in Tuvalu (332 patients; age range,
1–76 years old), were assessed for skin diseases via a complete
dermatological examination. All participants were asked about any
previous skin diseases, other medical conditions and family
history. Diagnosis of various cutaneous conditions was based on
characteristic clinical features. In certain instances, the
diagnosis of superficial fungal infections was confirmed by a
potassium hydroxide assay (3,4). The
study was approved by the Ethics Committee of Chung Shan Medical
University Hospital (Taichung, Taiwan, R.O.C.; CS 14137), and
written informed consent was obtained where required.
Results
Dermatological diseases in Tuvalu. Among the
332 patients, 177 (53.3%) were females and 155 (46.7%) were males,
with an average age of 30.2±6.3 years. Frequently observed skin
conditions included pruritus, excoriations, scratching, painful
wounds, unhealed ulcers, skin discoloration, acne and keloids. The
most common dermatological diseases and their respective prevalence
were as follows: Eczema/dermatitis (37.7%), superficial fungal
infections (34.3%), impetigo (21.7%), carbuncles and furuncles
(16.9%), folliculitis (11.1%), cellulitis (9.3%), acne (15.6%),
prurigo nodularis (12.3%), intertrigo (9.6%), scabies (14.4%),
warts (7.5%) and keloids (5.4%) as presented in Table I. Eczema/dermatitis included atopic
dermatitis, seborrheic dermatitis, contact dermatitis, dyshidrotic
eczema, summer eczema, nummular eczema, stasis dermatitis and
lichen simplex chronicus. Superficial fungal infections included
tinea capitis, tinea barbae, tinea corporis, tinea cruris, tinea
mamuum, tineapedis, onychomycosis and mucocutaneous candidiasis.
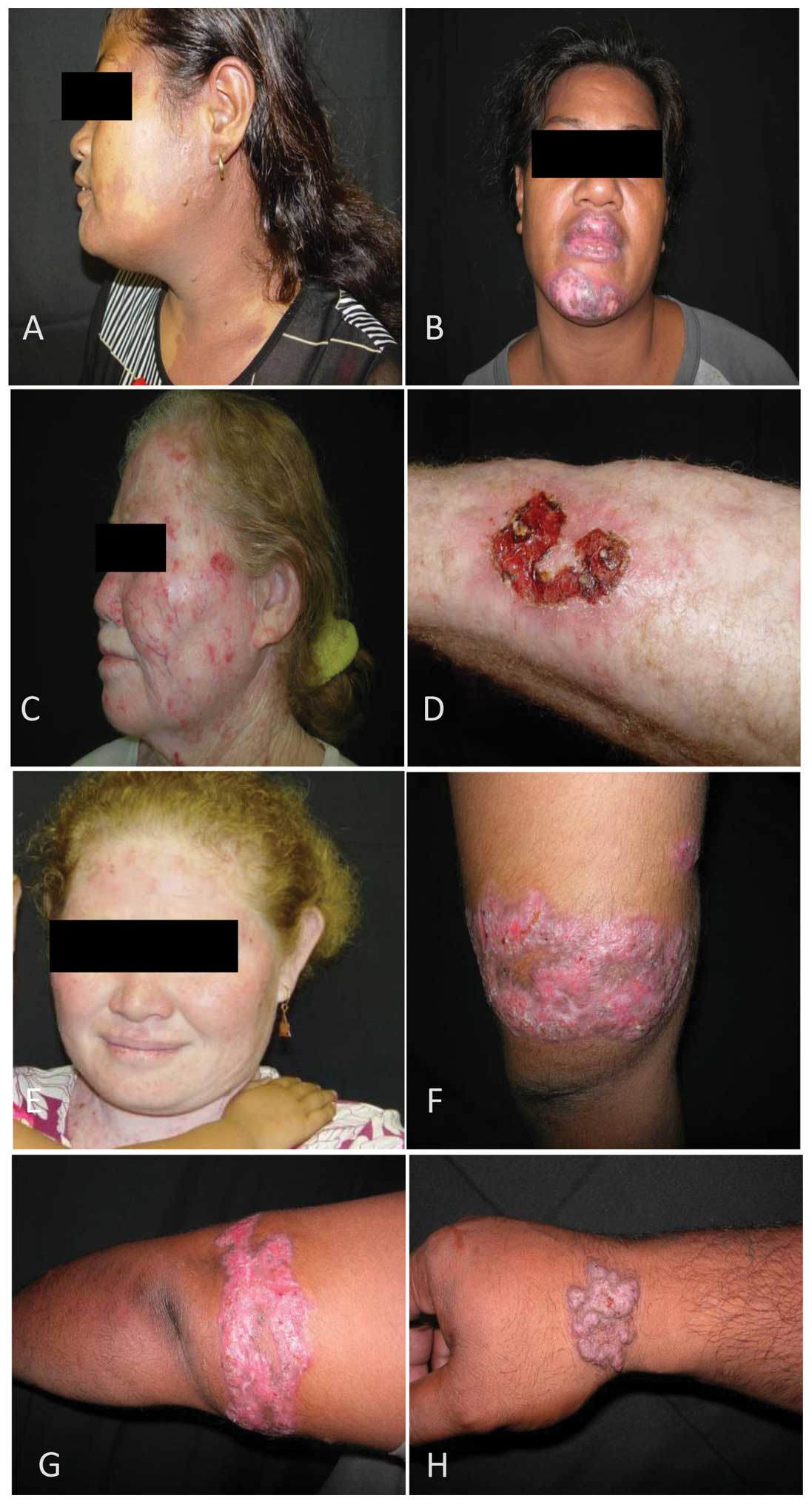
Infrequent skin conditions listed in Table II included port–wine stain
(Fig. 1A), discoid lupus
erythematosus (Fig. 1B), vitiligo,
mammary Paget's diseases, albinism (Fig. 1C–E), actinic keratosis, squamous
cell carcinoma and infectious granulomatous diseases (Fig. 1F–H), which all required medical
treatment.
 | Table IThe most common dermatological
diseases in Tuvalu. |
Table I
The most common dermatological
diseases in Tuvalu.
| Disease | n | % |
|---|
| Infectious
diseases | | |
| Superficial fungal
infections | 114 | 34.3 |
| Impetigo | 72 | 21.7 |
| Carbuncles and
furuncles | 56 | 16.9 |
| Folliculitis | 37 | 11.1 |
| Cellulitis | 31 | 9.3 |
| Scabies | 48 | 14.4 |
| Verruca | 25 | 7.5 |
| Inflammatory
diseases | | |
| Eczema | 125 | 37.7 |
| Prurigo
nodularis | 41 | 12.3 |
| Acne | 52 | 15.6 |
| Intertrigo | 32 | 9.6 |
| Miscellanies | | |
| Keloids | 18 | 5.4 |
 | Table IIInfrequent dermatological diseases
requiring medical assistance. |
Table II
Infrequent dermatological diseases
requiring medical assistance.
| Disease | No. of patients |
|---|
| Infectious
diseases | |
| Infectious
granulomatous disease | 6 |
| Inflammatory
diseases | |
| Discoid lupus
erythematosus | 2 |
| Malignancies | |
| Mammary Paget's
disease | 1 |
| Squamous cell
carcinoma | 1 |
| Actinic
keratosis | 2 |
| Miscellanies | |
| Albinism | 3 |
| Vitiligo | 1 |
| Neurofibromas | 1 |
| Port-wine stain | 1 |
Discussion
This report is the first epidemiological study to
investigate the prevalence of dermatological diseases in Tuvalu.
Leppäniemi (5–8) has reported on several surgical procedures and
surgical cases in Tuvalu between 1990-1993. Nelesone et al
(9) established a successful
African outbreak surveillance model for poliomyelitis, cholera,
diarrhoea, dysentery, typhoid, measles, meningococcalmeningitis and
outbreaks of febrile diseases of unknown origin, which may provides
a basis for a potential model for use in Tuvalu (9). However, medical staff and access to
care were inadequate in the past.
In Tuvalu, the climate is usually hot and hygiene is
poor due to the lack of a clean water supply. The majority of the
population collect rainwater from the roofs of buildings and store
it for daily use (1). Skin
infections are a common health problem in Tuvalu, as well as in
other Pacific island nations (10). Superficial fungal infections and
scabies were found in 34.3 and 14.4% of individuals in Tuvalu
respectively, and the ratio of scabies was similar to that observed
in the population of Tanna in Vanuatu (10). The results of the current study are
in agreement with Steer et al (11) in that the most common skin problems
in children in Fiji were infected scabies (22.2%), impetigo
(20.2%), non–infected scabies (9.7%) and abscesses or localized
cellulitis (8.1%). Following the introduction of crotamiton lotion
and/or permethrin cream, the incidence of scabies in Tuvalu has
been observed by the authors of the current study to be in decline.
In addition, the present study determined that following education
on the treatment of skin wounds (avoiding contact with seawater),
other infectious diseases, such as impetigo, carbuncles, furuncles
and cellulitis were cured with short courses of amoxicillin or
cephalosporin.
The rare but important issue was the observation of
infectious granulomatous diseases in Tuvalu. Skin biopsy,
histopathology and tissue culture were not available, and so the
diagnosis of these granulomatous diseases was difficult. Tuvalu's
predominant diseases are tuberculosis, leprosy and parasitic
infections (1). Four non–endemic
cases in patients from Pacific Islands are described to have
chromoblastomycosis caused by Fonsecaea pedrosoi (12). Chromoblastomycosis, deep fungal
infection, leprosy, tuberculosis cutis or sarcoidosis must be
included in the differential diagnosis in these patients with
granulomatous diseases (Fig.
1F–H).
In the current study, a number of patients with
albinism suffered from severe photosensivities, actinic keratosis
and skin cancer (Fig. 1E–G).
Similar issues have been described in Africa (12). This is particularly problematic for
individuals with albinism living in tropical countries with intense
UV exposure, and these individuals are negatively impacted
emotionally and physically from dermatological malignancies
(13–15). Variants of the MC1R gene in patients with oculocutaneous
albinism increased susceptibility to skin cancer (14). Frequent skin evaluations should be
performed, in addition to education for patients regarding sun
protection.
This study is the first epidemiological report of
skin disorders in Tuvalu. Future studies are required, in which
clinical assessments are made and current treatment approaches are
evaluated.
Acknowledgments
The authors would like to thank the Medical Project
in the Pacific Island Countries and Mobile Medical Missions
supported by the Taiwan International Cooperation and Development
Fund (Taiwan ICDF) and the Chung Shan Medical University Hospital
(Taiwan). The authors would like to acknowledge the epidemiological
information provided by the Bureau of Consular Affairs, Ministry of
Foreign Affairs, Republic of China (Taiwan), and would like to
recognise the help from Dr Nese Ituaso, Dr Stephen Homasi, Mr.
Pelesala Kaleia, and the medical team from the Princess Margaret
Hospital (Tuvalu).
References
|
1
|
Tuvalu demographics: Bureau of Consular
Affairs, Ministry of Foreign Affairs, Republic of China (Taiwan).
http://www.boca.gov.tw/ct.asp?xItem=829&ctNode=753&mp=1
(In Chinese). Accessed March 24, 2015.
|
|
2
|
Medical Project in the Pacific Island
Countries: Taiwan International Cooperation and Development Fund
(TaiwanICDF). http://www.icdf.org.tw/np.asp?ctNode=29872&mp=2.
Accessed March 24, 2015.
|
|
3
|
Sasmaz S and Celik M: Skin diseases in
Turkish soldiers. Dermatol Sinica. 29:44–46. 2011. View Article : Google Scholar
|
|
4
|
Yamamoto T, Hung WC, Takano T and
Nishiyama A: Genetic nature and virulence of community-associated
methi-cillin-resistant Staphylococcus aureus. BioMedicine. 3:2–18.
2013. View Article : Google Scholar
|
|
5
|
Leppäniemi AK: Surgery in Tuvalu: a
10–year review. Aust N Z J Surg. 60:373–376. 1990. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Leppäniemi AK: Intravesical foreign body
after inguinal herni-orrhaphy. Case report. Scand J Urol Nephrol.
25:87–88. 1991. View Article : Google Scholar
|
|
7
|
Leppäniemi AK: Where there is no
anaesthetist. Br J Surg. 78:245–246. 1991. View Article : Google Scholar
|
|
8
|
Leppäniemi AK: Obstetrics and the general
surgeon. Surg Gynecol Obstet. 176:365–367. 1993.PubMed/NCBI
|
|
9
|
Nelesone T, Durrheim DN, Speare R,
Kiedrzynski T and Melrose WD: Short communication: Strengthening
sub-national communicable disease surveillance in a remote Pacific
Island country by adapting a successful African outbreak
surveillance model. Trop Med Int Health. 11:17–21. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Harris M, Nako D, Hopkins T, et al: Skin
infections in Tanna, Vanuatu in 1989. P N G Med J. 35:137–143.
1992.PubMed/NCBI
|
|
11
|
Steer AC, Tikoduadua LV, Manalac EM, et
al: Validation of an integrated management of childhood illness
algorithm for managing common skin conditions in Fiji. Bull World
Health Organ. 87:173–179. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Woodgyer AJ, Bennetts GP and Rush–Munro
FM: Four non-endemic New Zealand cases of chromoblastomycosis.
Australas J Dermatol. 33:169–176. 1992. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Cruz-Inigo AE, Ladizinski B and Sethi A:
Albinism in Africa: stigma, slaughter and awareness campaigns.
Dermatol Clin. 29:79–87. 2011. View Article : Google Scholar
|
|
14
|
Sengupta M, Sarkar D, Mondal M, et al:
Analysis of MC1R variants in Indian oculocutaneous albinism
patients: highlighting the risk of skin cancer among albinos. J
Genet. 92:305–308. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
de Vijlder HC, de Vijlder JJ and Neumann
HA: Oculocutaneous albinism and skin cancer risk. J Eur Acad
Dermatol Venereol. 2012.PubMed/NCBI
|