Introduction
Ureteral obstruction is a disease that may result
from a diversity of congenital or acquired conditions, ranging from
calculi to strictures and to inflammatory processes and
malignancies (1). The treatment for
choice of urinary tract obstruction is to relieve the obstruction.
However, sustained ureteral obstruction can eventually lead to
progressive glomerulosclerosis, tubulointerstitial fibrosis and the
loss of renal function (2–4). Therefore, rapid diagnosis and initiation
of the treatment are vital to preserve function and/or to slow down
obstructive renal injury.
MicroRNAs (miRNAs/miRs) are endogenous
single-stranded small noncoding RNAs of 21–25 nucleotides that
regulate gene expression at the posttranscriptional level (5). miRNAs are involved in various cellular
biological functions, including apoptosis, proliferation,
differentiation and metabolism. The abnormal expression of miRNAs
has been reported to be associated with the development of many
human diseases (6–8). For example, miR-29a, miR-101-3p and
miR-127a are highly expressed in the kidney, where it acts against
fibrosis by suppressing collagen expression in tubular cells
(9–11).
Downregulated serum levels of miR-29a, miR-101-3p and miR-127a have
been indicated to predict the degree of acute kidney injury (AKI)
in ICU patients (9). Thus, miRNAs may
serve important roles in various kidney diseases, and some of them
even can be used as biomarkers in early diagnosis and detecting
disease development (12,13).
Previous studies of the authors have demonstrated
that the activation of the hedgehog signaling pathway contributes
to renal injury and fibrogenesis via epithelial-mesenchymal
transitions (EMT) in obstructive renal injury (14,15).
Inhibiting the activation of hedgehog signaling or the induction of
EMT can attenuate even reverse obstruction-induced fibrosis
(16). Thus, miRNAs concerning the
regulation of hedgehog signaling or EMT may be potential targets
for obstructive renal injury. A previous study by Ferretti et
al (17) reported that miR-125b,
miR-324-5p and miR-326 serve important roles in cerebellar neuronal
progenitor and tumor cells through targeting the hedgehog signaling
(Smo and Gli1). Other studies have identified that miR-125b and
miR-326 regulate in several cells through suppressing the EMT
process (18–20). In addition, miR-125b is critical for
cardiac fibrosis, and miR-326 regulates profibrotic functions of
tumor growth factor (TGF)-β1 in pulmonary fibrosis (20,21).
Furthermore, miR-324-5p inhibits the induction of EMT and
metastasis of cancer cells (22).
Therefore, the authors hypothesized that miR-125b-5p, miR-324-5p
and miR-326 may be correlated with obstructive renal injury, and as
potential biomarkers for disease diagnosis or prognosis
monitoring.
Patients and methods
Subjects
Consecutive peripheral blood specimens were
collected between January 2015 and July 2015 from 76 controls and
91 patients with ureteral obstruction in the First Affiliated
Hospital of Wenzhou Medical University (Wenzhou, China), and extra
details about the participants are listed in Table I. All patients with ureteral
obstruction were confirmed by B-scan ultrasonography, and the serum
levels of creatinine (SCr), blood urea nitrogen (BUN), cholesterol
(CHE), triglyceride (TG), high-density lipoprotein (HDL) and low
density lipoprotein (LDL) in serum were examined by using an AU5800
automatic biochemistry analyzers (Beckman Coulter, Inc., Brea, CA,
USA).
 | Table I.Demographic and baseline clinical
data. |
Table I.
Demographic and baseline clinical
data.
| Characteristics | Control (n=76) | Patients with
ureteral obstruction (n=91) | Odds ratio (95%
CI) | P-value |
|---|
| Gender |
|
|
|
|
| Male | 41 (53.9%) | 53 (58.2%) | 1.19 (0.64–2.20) |
0.577b |
|
Female | 35 (46.1%) | 38 (41.8%) |
|
|
| Age (year) | 42.20±12.79 | 53.75±12.40 |
|
<0.001a |
|
<50 | 12 (14.8%) | 29 (31.9%) | 2.50 (1.17–5.32) |
0.016b |
| ≥ 50 | 64 (84.2%) | 62 (68.1%) |
|
|
| Urinary tract
obstruction |
|
|
|
|
|
Unilateral (left) | 0 | 49 (53.8%) |
|
|
|
Unilateral (right) | 0 | 31 (34.1%) |
|
|
|
Bilateral | 0 | 9 (9.9%) |
|
|
| Renal function |
|
|
|
|
| SCr
(µmol/l) | 64.76±12.55 | 84.32±34.88 |
|
<0.001a |
| BUN
(mmol/l) | 5.09±1.16 | 7.03±8.01 |
| 0.01a |
| Serum lipid
levels |
|
|
|
|
| CHE
(mmol/l) | 5.21±1.00 | 4.87±0.96 |
| 0.04a |
| TG
(mmol/l) | 1.90±1.43 | 1.79±1.14 |
| 0.93a |
| HDL
(mmol/l) | 1.32±0.50 | 1.08±0.31 |
|
<0.001a |
| LDL
(mmol/l) | 3.10±0.74 | 2.87±0.80 |
| 0.12a |
All subjects were informed about the contents of the
study and gave their informed consent. This study was approved by
the Ethics Committee of Wenzhou Medical University.
Sample preparation and miRNA
extraction
Whole blood specimens were collected by venipuncture
in EDTA K2-treated collection tubes and processed immediately or
stored at 4°C overnight. A total of 0.7 ml EDTA-treated whole blood
and 2.1 ml red blood cell lysis solution (R1010-500; Beijing
Solarbio Science & Technology Co., Ltd., Beijing, China) were
pipetted into a tube and vortex gently for 20 sec. Then the tubes
were put on ice for 15 min, and gently homogenized mixing twice
between blending. The white blood cells were collected by
centrifugation at 450 × g for 10 min at 4°C. Red blood cell
lysis solution (1.4 ml) was added into the tube, and a suspension
of white blood cells was made. The cells were collected by
centrifugation at 450 × g for 10 min at 4°C. TRIzol reagent
(1 ml; P/N: 15596-026; Ambion; Thermo Fisher Scientific, Inc.,
Waltham, MA, USA) were added into the collected cells and total RNA
was extracted according to the manufacturer's instructions.
Reverse transcription-quantitative
polymerase chain reaction (RT-qPCR)
RT was performed using the RevertAid First Strand
cDNA Synthesis kit (Thermo Fisher Scientific, Inc.). The 10 µl RT
reaction mixture contained the following: 1 µl treated RNA (0.1
ng-5 mg), 1 µl RT stem-loop primer (5 µM) and 1 µl U6 RT primer (5
µM), 1 µl dNTP Mix (10 mM), 2 µl 5X reaction buffer (cat no.
K1622), 0.5 µl Ribolock RNase inhibitor (20 U/ml; all Thermo Fisher
Scientific, Inc.), and 0.5 µl RevertAid M-MuLV reverse
transcriptase (200 U/ml; Thermo Fisher Scientific, Inc.). The
mixture was incubated at 25°C for 5 min, and then incubation was
continued at 42°C for 60 min. The reaction was inactivated by
heating at 70°C for 5 min. The RT reaction was performed in
triplicate to remove RT outliers. RT-qPCR was performed using
SYBR-Green fluorescence quantitative PCR reagent kit (cat. no.
QPS-201T; Toyobo Co., Ltd., Osaka, Japan) on a 7500 real-time
quantitative PCR instrument (Applied Biosystems; Thermo Fisher
Scientific, Inc.), and each sample was analyzed in triplicate. The
10 µl PCR volume included 1 µl RT product, 5 µl SYBR-Green
real-time PCR Master Mix (Roche Diagnostics, Basel, Switzerland),
and 1 µl primer (1 µM). The reactions were incubated at 95°C for 3
min, followed by 40 cycles of 95°C for 5 sec, 58°C for 35 sec. The
expression levels of miRNAs (miR-125b-5p, miR-324 and miR-326) were
analyzed by calculating the equation 2−∆∆Cq and
normalized to U6 expression (23,24). All
primers are presented in Table
II.
 | Table II.The primers of RT-quantitative
polymerase chain reaction. |
Table II.
The primers of RT-quantitative
polymerase chain reaction.
| Primer | RT stem-loop primer
sequence (5′-3′) | Forward primer
sequence (5′-3′) | Reverse primer
sequence (5′-3′) |
|---|
| miR-125b-5p |
GAAAGAAGGCGAGGAGCAGATCG | CGCTCCCTGA | CGAGGAAGAA |
|
|
AGGAAGAAGACGGAAGAATGTGC | GACCCTAACT | GACGGAAGAAT |
|
|
GTCTCGCCTTCTTTCTCACAAGT |
|
|
| miR-324-5p |
GAAAGAAGGCGAGGAGCAGATCG | CGCATCCCC | CGAGGAAGAA |
|
|
AGGAAGAAGACGGAAGAATGT | TAGGGCAT | GACGGAAGAAT |
|
|
GCGTCTCGCCTTCTTTCACACCAAT |
|
|
| miR-326 |
GAAAGAAGGCGAGGAGCAGATCG | GCCTCTGG | CGAGGAAGAA |
|
|
AGGAAGAAGACGGAAGAATGTGCG | GCCCTTCC | GACGGAAGAAT |
|
|
TCTCGCCTTCTTTCCTGGAGGA |
|
|
| U6 |
CGCTTCACGAATTTGCGTGTCAB | GCTTCGGCAGCACA | CGCTTCACGAA |
|
|
| TATACTAAAAT | TTTGCGTGTCAT |
Statistical analysis
Statistical analysis was performed using SPSS
software (version 19.0; IBM SPSS, Armonk, NY, USA). All data were
presented as mean ± standard deviation with normal distribution,
and median (lower and upper quartiles) for the others. A binary
logistic regression analysis was conducted to adjust the influence
of age and gender. Data were compared by the Mann-Whitney U test
and Spearman's rank order correlations as appropriate. P<0.05
was considered to indicated a statistically significant difference.
All probabilities were two-tailed.
Results
Risk assessment of obstructive renal
injury
The demographic and baseline clinical data of the
study subjects are summarized in Table
I. The serum levels of SCr (P<0.001) and BUN (P=0.01) in
patients with ureteral obstruction were significantly higher than
those in controls, indicating that ureteral obstruction induced
renal injury and function decline, though the extent of renal
injury did not reach the diagnosis standard of nephropathy (97
µmol/l). In addition, the serum levels of HDL in patients with
ureteral obstruction are significantly lower than those in controls
(P<0.001), suggesting that patients with ureteral obstruction
have a higher risk of hyperlipidemia.
Levels of miRNAs in controls and
patients with obstructive renal injury
As presented in Table
III, there were strong internal correlations in levels among
these three miRNAs (P<0.001). Data were compared by Spearman's
rank order correlations.
 | Table III.Internal correlation among the
miRNAs. |
Table III.
Internal correlation among the
miRNAs.
| Level | miR-125b-5p | miR-324-5p |
|---|
| miR-324-5p |
|
|
| r |
0.764 | – |
| P | <0.001 | – |
| miR-326 |
|
|
| r |
0.858 |
0.842 |
| P | <0.001 | <0.001 |
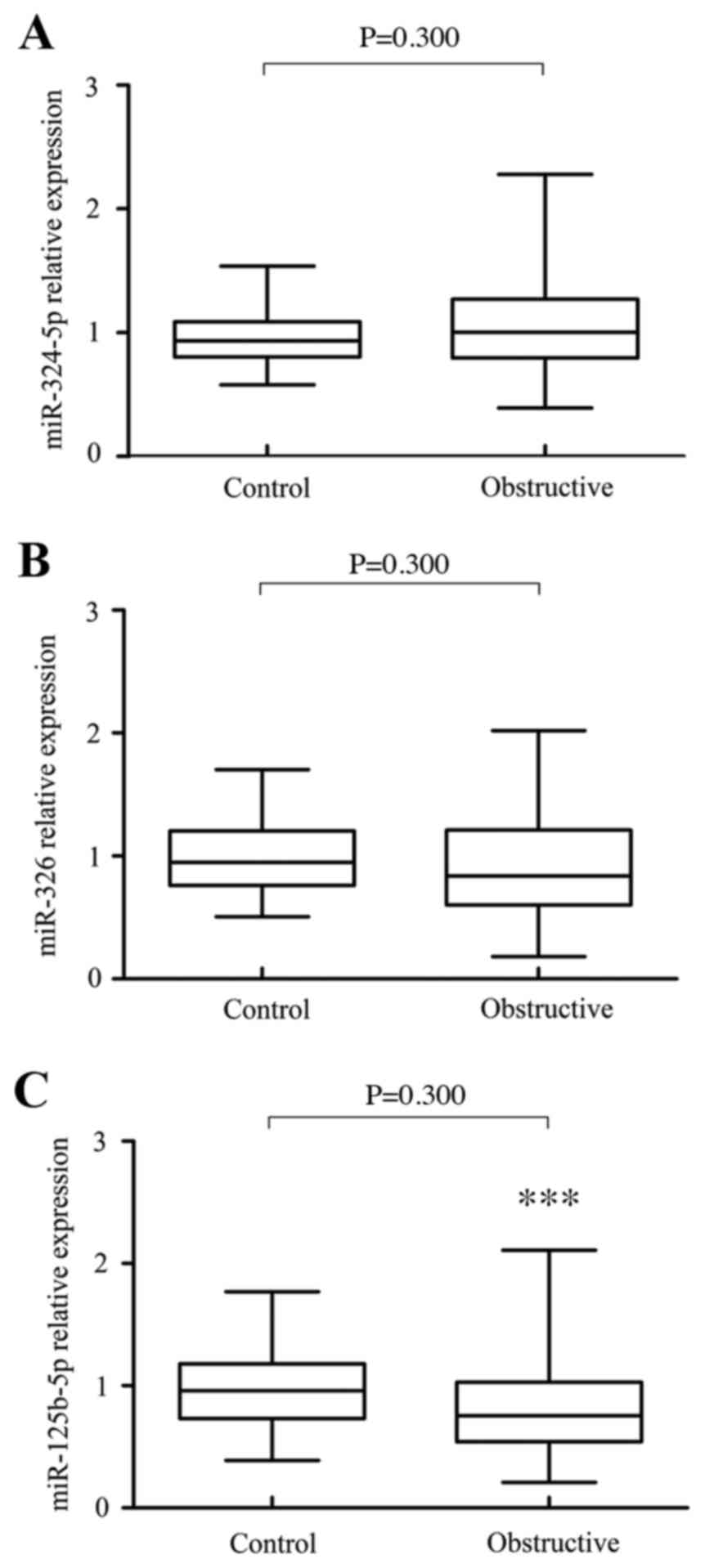
The expression levels of miR-125b-5p, miR-324-5p and
miR-326 are summarized in patients with ureteral obstruction and
controls (Fig. 1). The results
demonstrated that the expression of miR-324-5p [1.003 (0.391–2.279)
vs. 0.934 (0.579–1.539), P=0.300] and miR-326 [0.840 (0.180–2.020)
vs. 0.949 (0.507–1.702), P=0.050] did not suggest any significant
difference (Figs. 1A and B). However,
the expression of miR-125b-5p [0.755 (0.210–2.110) vs. 0.960
(0.390–1.770), P=0.002] in patients with ureteral obstruction was
significantly lower than those in controls, indicating that
miR-125b-5p may be potential protective biomarkers in patients with
obstructive renal injury (Fig. 1C).
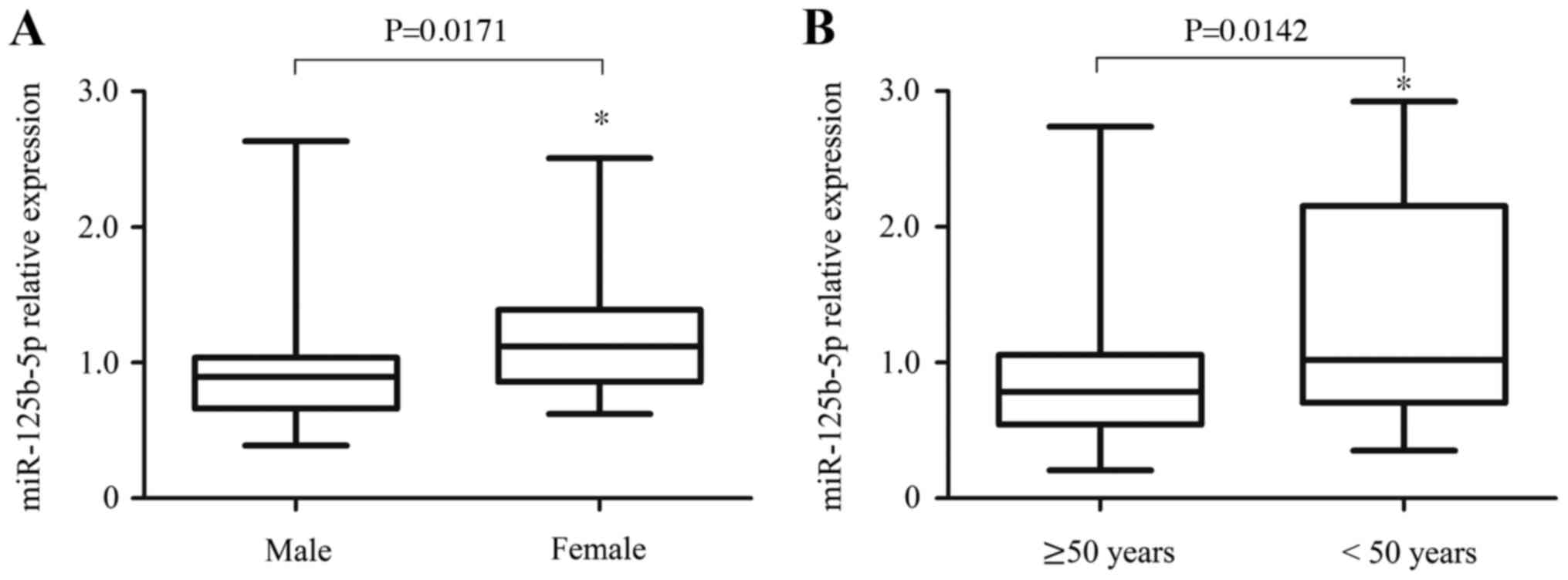
Interestingly, the authors identified that the protective effect of
miR-125b-5p has a significant correlation with gender and age. In
patients with ureteral obstruction, the levels of miR-125b-5p in
male were lower than those in female [0.965 (0.833–1.097) vs. 1.222
(1.055–1.389), P=0.0171; Fig. 2A].
Moreover, the levels of miR-125b-5p in the older patients (≥50
years) were lower than those in the younger patients [<50 years,
0.966 (0.801–1.131) vs. 1.359 (1.066–1.652), P=0.0142; Fig. 2B]. Thus, higher levels of miR-125b-5p
in younger and female patients may be an important protective
biomarker against obstructive renal injury.
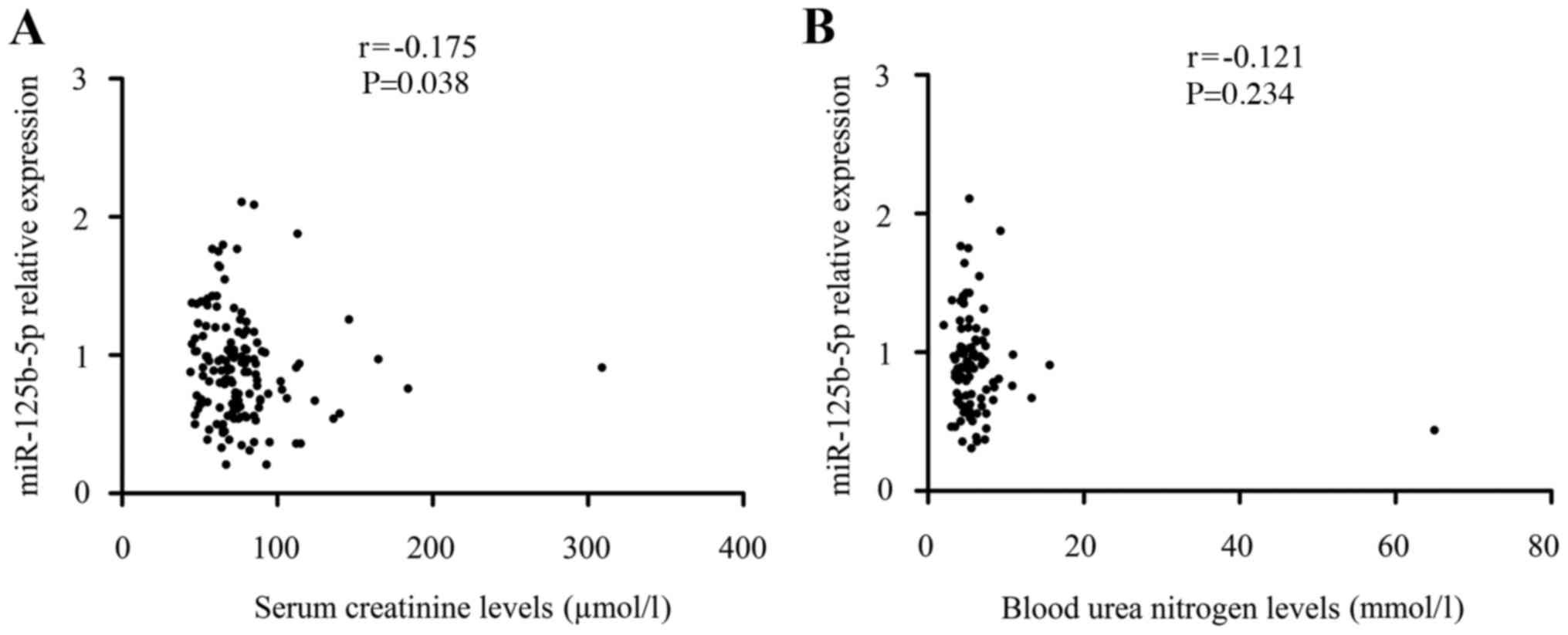
Association between miR-125b-5p levels
and renal function
Given that miR-125b-5p can exert its protective
effects on obstructive renal injury, the authors investigated
whether the effects of miR-125b-5p correlated with renal function.
As demonstrated in Fig. 3, the levels
of miR-125b-5p (r=−0.175, P=0.038) in patients with ureteral
obstruction were significantly negatively correlated to the serum
levels of SCr, though not correlated to the levels of BUN
(P>0.05). These results confirmed again to some extent that the
protective roles of miR-125b-5p in obstructive renal injury may be
associated with downregulated SCr levels. There were no significant
internal correlation between miRNA levels and serum lipid levels
(P>0.05; Table IV).
 | Table IV.Internal correlation between miRNA
levels and serum lipid levels. |
Table IV.
Internal correlation between miRNA
levels and serum lipid levels.
| Level | CHE | TG | HDL | LDL |
|---|
| miR-125b-5p |
|
|
|
|
| r | −0.014 | 0.059 | −0.027 | −0.022 |
| P |
0.869 | 0.485 |
0.748 |
0.794 |
| miR-324-5p |
|
|
|
|
| r | −0.112 | −0.045 | −0.152 | −0.046 |
| P |
0.182 |
0.595 |
0.067 |
0.580 |
| miR-326 |
|
|
|
|
| r | −0.057 | −0.042 | −0.026 | 0.001 |
| P |
0.496 |
0.614 |
0.750 | 0.988 |
Discussion
Obstruction of the ureter resulted in renal
dysfunction with marked increases in BUN and SCr (2,25). In the
current study, the authors demonstrated that the levels of SCr in
patients with ureteral obstruction were significant higher than
those in controls. Upregulated levels of SCr following ureteral
obstruction indicated that the kidney was injured, but the extent
of injury did not reach the diagnosis standard of nephropathy, and
thereby did not cause marked renal dysfunction. A previous study
has indicated that HDL can reduce renal ischemia/reperfusion injury
and mortality via modulation of the expression of adhesion
molecules and pro-inflammatory enzymes (26). HDL levels in patients with ureteral
obstruction were significantly lower (P<0.001), when compared
with control samples, identifying the protective role of HDL in
obstructive renal injury.
A number of studies have demonstrated that miRNAs
were involved in the development and progression of obstructive
renal injury and fibrosis (27,28).
Smad3-mediated upregulation of miR-21 promotes fibrosis in
established obstructive renal injury (27). TGF-β/Smad3 signaling promotes renal
fibrosis by inhibiting miR-29 (28).
miR-192 mediates TGF-beta/Smad3-driven renal fibrosis (29). In the current study, levels of
miR-125b-5p in patients with ureteral obstruction were
significantly lower than those in controls, though miR-324-5p
levels did not present any significant difference. Moreover,
compared with the younger or female patients, the levels of
miR-125b-5p in male or elder patients were lower. Further
examination revealed that miR-125b-5p levels were negatively
correlated with SCr levels, suggesting that miR-125b-5p may be a
protective biomarker for obstructive renal injury. However, the
levels of miR-125b-5p were not associated with serum lipid levels,
indicating that the effects of miR-125b-5p and serum lipid on renal
injury are independent of each other.
Currently, the roles and functions of miR-125b-5p in
obstructive renal injury remain unknown. A previous study of the
authors indicated that injury-induced activation of the hedgehog
signaling pathway stimulated TGF-β1 expression and promoted the
induction of EMT, resulted in excessive ECM component synthesis and
deposition in the cortical interstitium of kidneys (16). In vivo and in vitro, the
activity of hedgehog signaling may be regulated by miR-125b, which
serves an important role in cell proliferation and differentiation
and tissue regeneration (17,30). miR-125b exerts its inhibitory effects
on EMT and EMT-associated traits in tumorigenesis by antagonizing
TGF-β1/Smad signaling pathway (19).
Taken together, these findings provide some suggestive evidence of
the protective biomarkers of miR-125b-5p for obstructive renal
injury. Further studies should be performed to investigate the
functions of these two miRNAs involved in the regulation of the
hedgehog and TGF-β1/Smad signaling pathway in various experimental
models.
However, it should be noted that there are some
other limitations in the present study. The sample size was too
small to evaluate the stage of renal injury in patients with
ureteral obstruction due to the lack of pathological evidence.
Additionally, these results revealed that there were strong
correlations in levels among three miRNAs, but we did not know how
to interact with each other. Furthermore, whether these miRNAs can
be used as biomarkers in early diagnosis and detecting disease
development, and whether to have high sensitivity and specificity
should be further studied.
In conclusion, these findings indicated that the
expression levels of miR-125b-5p and miR-326 were decreased in
patients with ureteral obstruction, and correlated with the loss of
renal function. Thus, miR-125b-5p may be a potential protective
biomarker for obstructive renal injury.
Acknowledgements
The current study was sponsored by the Natural
Science Foundation of Zhejiang Province (grant no. LY17H050005) and
the Wenzhou Municipal Science and Technology Plan Project (grant
no. Y20150037). The project was also supported by the Natural
Science Foundation of China (grant no. 81572087).
References
|
1
|
Dikmen B, Yagmurdur H, Akgul T, Astarci M,
Ustun H and Germiyanoglu C: Preventive effects of propofol and
ketamine on renal injury in unilateral ureteral obstruction. J
Anesth. 24:73–80. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Ucero AC, Benito-Martin A, Izquierdo MC,
Sanchez-Niño MD, Sanz AB, Ramos AM, Berzal S, Ruiz-Ortega M, Egido
J and Ortiz A: Unilateral ureteral obstruction: Beyond obstruction.
Int Urol Nephrol. 46:765–776. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Kinn AC and Bohman SO: Renal structural
and functional changes after unilateral ureteral obstruction in
rabbits. Scand J Urol Nephrol. 17:223–234. 1983. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Klahr S: New insights into the
consequences and mechanisms of renal impairment in obstructive
nephropathy. Am J Kidney Dis. 18:689–699. 1991. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Lee RC, Feinbaum RL and Ambros V: The C.
elegans heterochronic gene lin-4 encodes small RNAs with antisense
complementarity to lin-14. Cell. 75:843–854. 1993. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Glowacki F, Savary G, Gnemmi V, Buob D,
van der Hauwaert C, Lo-Guidice JM, Bouyé S, Hazzan M, Pottier N,
Perrais M, et al: Increased circulating miR-21 levels are
associated with kidney fibrosis. PLoS One. 8:e580142013. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Sayed D and Abdellatif M: MicroRNAs in
development and disease. Physiol Rev. 91:827–887. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Wang G, Kwan BC, Lai FM, Chow KM, Li PK
and Szeto CC: Urinary miR-21, miR-29, and miR-93: Novel biomarkers
of fibrosis. Am J Nephrol. 36:412–418. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Aguado-Fraile E, Ramos E, Conde E,
Rodríguez M, Martín-Gómez L, Lietor A, Candela Á, Ponte B, Liaño F
and García-Bermejo ML: A Pilot Study Identifying a Set of microRNAs
As Precise Diagnostic Biomarkers of Acute Kidney Injury. PLoS One.
10:e01271752015. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Wang B, Komers R, Carew R, Winbanks CE, Xu
B, Herman-Edelstein M, Koh P, Thomas M, Jandeleit-Dahm K,
Gregorevic P, et al: Suppression of microRNA-29 expression by
TGF-β1 promotes collagen expression and renal fibrosis. J Am Soc
Nephrol. 23:252–265. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Aguado-Fraile E, Ramos E, Sáenz-Morales D,
Conde E, Blanco-Sánchez I, Stamatakis K, del Peso L, Cuppen E,
Brüne B and Bermejo ML: miR-127 protects proximal tubule cells
against ischemia/reperfusion: Identification of kinesin family
member 3B as miR-127 target. PLoS One. 7:e443052012. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Fan PC, Chen CC, Chen YC, Chang YS and Chu
PH: MicroRNAs in acute kidney injury. Hum Genomics. 10:292016.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Liu Z, Wang S, Mi QS and Dong Z: MicroRNAs
in Pathogenesis of Acute Kidney Injury. Nephron. 134:149–153. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Bai Y, Lu H, Lin C, Xu Y, Hu D, Liang Y,
Hong W and Chen B: Sonic hedgehog-mediated epithelial-mesenchymal
transition in renal tubulointerstitial fibrosis. Int J Mol Med.
37:1317–1327. 2016.PubMed/NCBI
|
|
15
|
Hu L, Lin X, Lu H, Chen B and Bai Y: An
overview of hedgehog signaling in fibrosis. Mol Pharmacol.
87:174–182. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Bai Y, Lu H, Wu C, Liang Y, Wang S, Lin C,
Chen B and Xia P: Resveratrol inhibits epithelial-mesenchymal
transition and renal fibrosis by antagonizing the hedgehog
signaling pathway. Biochem Pharmacol. 92:484–493. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Ferretti E, De Smaele E, Miele E, Laneve
P, Po A, Pelloni M, Paganelli A, Di Marcotullio L, Caffarelli E,
Screpanti I, et al: Concerted microRNA control of Hedgehog
signalling in cerebellar neuronal progenitor and tumour cells. EMBO
J. 27:2616–2627. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Zhang J, Na S, Liu C, Pan S, Cai J and Qiu
J: MicroRNA-125b suppresses the epithelial-mesenchymal transition
and cell invasion by targeting ITGA9 in melanoma. Tumour Biol.
37:5941–5949. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Zhou JN, Zeng Q, Wang HY, Zhang B, Li ST,
Nan X, Cao N, Fu CJ, Yan XL, Jia YL, et al: MicroRNA-125b
attenuates epithelial-mesenchymal transitions and targets stem-like
liver cancer cells through small mothers against decapentaplegic 2
and 4. Hepatology. 62:801–815. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Das S, Kumar M, Negi V, Pattnaik B,
Prakash YS, Agrawal A and Ghosh B: MicroRNA-326 regulates
profibrotic functions of transforming growth factor-β in pulmonary
fibrosis. Am J Respir Cell Mol Biol. 50:882–892. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Nagpal V, Rai R, Place AT, Murphy SB,
Verma SK, Ghosh AK and Vaughan DE: miR-125b Is Critical for
Fibroblast-to-Myofibroblast Transition and Cardiac Fibrosis.
Circulation. 133:291–301. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Song L, Liu D, Zhao Y, He J, Kang H, Dai
Z, Wang X, Zhang S and Zan Y: Sinomenine inhibits breast cancer
cell invasion and migration by suppressing NF-κB activation
mediated by IL-4/miR-324-5p/CUEDC2 axis. Biochem Biophys Res
Commun. 464:705–710. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Bustin SA, Benes V, Garson JA, Hellemans
J, Huggett J, Kubista M, Mueller R, Nolan T, Pfaffl MW, Shipley GL,
et al: The MIQE guidelines: Minimum information for publication of
quantitative real-time PCR experiments. Clin Chem. 55:611–622.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(−Delta Delta C(T)) Method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Butler J, Chirovsky D, Phatak H, McNeill A
and Cody R: Renal function, health outcomes, and resource
utilization in acute heart failure: A systematic review. Circ Heart
Fail. 3:726–745. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Thiemermann C, Patel NS, Kvale EO,
Cockerill GW, Brown PA, Stewart KN, Cuzzocrea S, Britti D,
Mota-Filipe H and Chatterjee PK: High density lipoprotein (HDL)
reduces renal ischemia/reperfusion injury. J Am Soc Nephrol.
14:1833–1843. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Zhong X, Chung AC, Chen HY, Meng XM and
Lan HY: Smad3-mediated upregulation of miR-21 promotes renal
fibrosis. J Am Soc Nephrol. 22:1668–1681. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Qin W, Chung AC, Huang XR, Meng XM, Hui
DS, Yu CM, Sung JJ and Lan HY: TGF-β/Smad3 signaling promotes renal
fibrosis by inhibiting miR-29. J Am Soc Nephrol. 22:1462–1474.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Chung AC, Huang XR, Meng X and Lan HY:
miR-192 mediates TGF-beta/Smad3-driven renal fibrosis. J Am Soc
Nephrol. 21:1317–1325. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Hyun J, Wang S, Kim J, Kim GJ and Jung Y:
MicroRNA125b-mediated Hedgehog signaling influences liver
regeneration by chorionic plate-derived mesenchymal stem cells. Sci
Rep. 5:141352015. View Article : Google Scholar : PubMed/NCBI
|